
Antoine Francis – Brent vs Plasma: The Other Strategic Resource
Antoine Francis, Chairman at Global Plasma Supply, shared a post on LinkedIn:
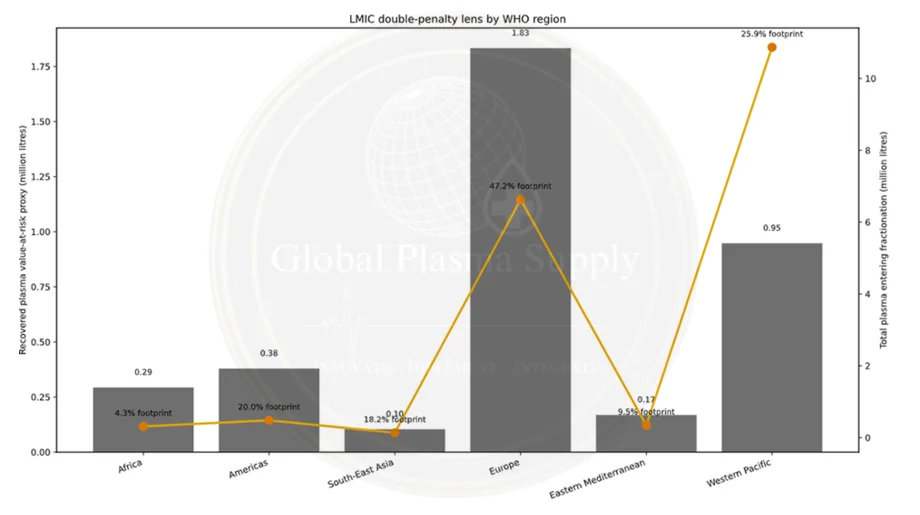
”Global attention routinely locks onto energy benchmarks (oil, gas) because the data are visible, liquid, and updated in near-real time. By contrast, plasma-derived medicinal products (PDMPs)-including immunoglobulins, albumin, and plasma-derived coagulation factors-sit in a less transparent market despite being essential for survival and long-term functioning in immune deficiency, bleeding disorders, and critical care. WHO notes that only 56 of 171 reporting countries produce PDMPs from domestically collected plasma, while 91 countries reported importing all PDMPs-structural dependence that is most dangerous for low- and middle-income countries (LMICs). [1]
The evidence base strongly supports the editorial frame that plasma is ‘strategic’ in the way energy is strategic, because (a) supply is geographically concentrated, (b) production has long lead times, (c) cross-border logistics are critical, and (d) shocks cascade quickly into rationing and treatment interruption. Peer-reviewed analysis of PDMP supply reports that the United States contributed approximately 71% of global source plasma (2017) and collected close to 40 million litres of source plasma in 2019, illustrating concentration risk. [2]
LMICs face a dual bind: import dependence plus constrained purchasing power and weaker logistics buffers. WHO explicitly states PDMP shortages are occurring globally and ‘most severely’ affect patients in LMICs, driven in part by insufficient domestic supply of plasma suitable for fractionation and limited technical/financial capacity for domestic programmes. [3] Evidence from the literature further highlights wastage of recovered plasma in LMICs and high costs of imported PDMPs, contributing to limited patient access. [4]
Finally, the ‘geopolitical shock’ lens is currently salient. Recent reporting describes disruption to pharmaceutical air routes through major hubs due to conflict, with risks for temperature-sensitive medicines and rising freight stress. [5] In parallel, UNCTAD documents how chokepoint disruptions and rerouting (e.g., around the Cape of Good Hope) extend voyage times and increase costs-exactly the conditions that degrade biologics resilience. [6]
LMICs lose twice
The burden on LMICs does not begin only when they enter the import market. It begins earlier, inside the blood system itself. As component therapy expands, many countries generate recovered plasma in excess of direct clinical need, but that plasma often fails to become fractionation feedstock because the surrounding system is not yet strong enough in traceability, validation, processing controls, and GMP-compatible handling.
WHO’s guidance is explicit on this point: inadequacy of PDMP access in LMICs is linked not only to global shortage, but also to insufficient domestic supplies of plasma of a quality suitable for fractionation. [7]
That is the first loss. A potentially strategic biological resource is created, but not fully retained as therapeutic value.
The 2024 Vox Sanguinis review states this sharply: there is huge wastage of recovered plasma in LMICs and LICs because GMP is lacking in the production of plasma for fractionation. ISBT echoes the same logic, noting that surplus recovered plasma in LMICs may remain unacceptable for fractionation when GMP is not in place, leading to considerable wastage. [4]
The second loss comes afterward. Once that plasma is not converted into usable fractionation material, the same countries are pushed back into the international market as buyers of finished PDMPs.
There, they face the premium end of dependency: imported immunoglobulins, albumin, and coagulation factors must be purchased in a market already shaped by shortage, concentration of supply, and unequal purchasing power. WHO reports that only 56 of 171 reporting countries produce PDMPs from domestically collected plasma, while 91 countries import all PDMPs. In that context, failure to retain domestic plasma value does not remain a technical problem; it becomes an access penalty. [1]
LMICs lose twice is more than rhetoric. First, they lose the plasma itself as recoverable national value. Then they lose again when patients must rely on scarce imported PDMPs obtained at higher cost and with weaker negotiating leverage. The Vox review ties these two losses together directly: wastage of recovered plasma and the high cost of imported PDMP procurement combine to limit patient access. [4]
What is needed now is a policy shift in mindset. LMICs cannot afford to remain trapped in a purely reactive model, waiting for shortages and then competing for imported PDMPs at the most expensive point of vulnerability. The smarter approach is upstream: stop losing fractionation value before it disappears. Recoverable plasma should be recognized as a strategic national resource, and policy should focus on improving plasma quality, reducing wastage, and building staged pathways toward contract fractionation and eventual domestic strengthening. That is where resilience begins – not at the point of emergency procurement, but at the point where biological value is either preserved or lost.
Price Discovery vs Patient Discovery
Global energy markets operate on continuous price discovery. Benchmarks such as Brent crude are updated in real time, translating geopolitical events and supply disruptions into immediate price signals that guide decision-making across the system. By contrast, plasma-derived medicinal products (PDMPs) lack any equivalent real-time visibility. There is no unified benchmark tracking immunoglobulin availability, albumin supply, or clotting factor access. As a result, scarcity in plasma systems is not priced early but revealed late-typically only when clinical consequences emerge. This difference in visibility fundamentally shapes how systems respond to shortage. [8]
In practice, PDMP scarcity is first detected not through market indicators, but through changes in clinical behavior. Hospitals begin to delay treatment initiation, adjust dosing protocols, or restrict eligibility criteria for therapies such as intravenous immunoglobulin (IVIG). These measures are well documented during periods of global immunoglobulin shortage, where supply constraints have led to rationing and prioritization of patients based on severity. By the time such measures are implemented, the shortage is already active within the system, indicating a delayed recognition of supply imbalance. [9]
This creates a structural visibility gap. In oil markets, scarcity is quantified and transmitted instantly, enabling pre-emptive adjustments in pricing, supply allocation, and logistics. In plasma systems, however, there is no comparable signal.
WHO has highlighted that PDMP shortages are occurring globally and disproportionately affect LMICs, yet these shortages are often identified only after access is compromised at the patient level. The absence of real-time monitoring mechanisms means that system response is inherently reactive rather than anticipatory. [1]
The implications of this gap are particularly severe in LMIC settings. Where systems are already constrained by import dependence and limited procurement flexibility, delayed visibility of shortages further weakens response capacity.
Instead of responding to early indicators of tightening supply, healthcare systems react only when clinical services are affected-when treatments are postponed, reduced, or unavailable. In this context, scarcity is not only a function of supply limitations but also of delayed detection and response.
This reinforces the broader structural imbalance in plasma systems. While energy markets respond to scarcity through immediate price signals, plasma systems rely on delayed clinical signals. In effect, scarcity in PDMPs is not discovered through markets, but through patients-appearing as postponed infusions, restricted access, and silent rationing across healthcare systems. [10] [11]

The ‘invisible embargo’
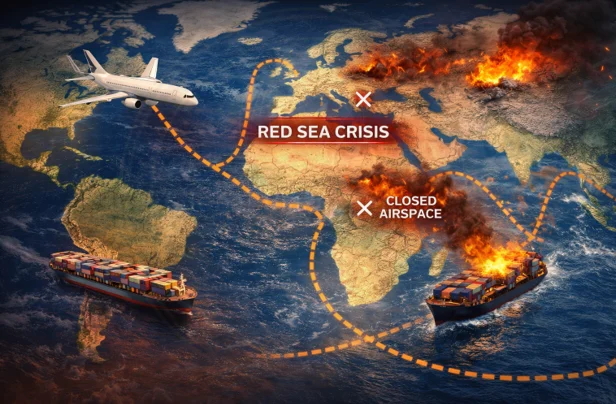
Geopolitical disruptions do not need to take the form of formal sanctions or declared blockades to affect access to plasma-derived medicinal products. Increasingly, the impact is indirect-manifesting through what can be described as an ‘invisible embargo.’ Route closures, airspace restrictions, and maritime rerouting alter the movement of temperature-sensitive biologics, introducing delays, increasing costs, and compromising reliability. Unlike traditional commodities, PDMPs depend on tightly controlled cold-chain logistics, where even minor disruptions can translate into loss of usable product or delayed patient access. [12]
Recent global events have demonstrated how quickly these disruptions propagate. Rerouting of vessels around high-risk zones-such as the Cape of Good Hope instead of the Suez Canal-has extended transit times and increased freight volatility.
For cold-chain dependent products, including plasma-derived therapies, this introduces cumulative risk: longer exposure windows, increased handling, and greater dependence on uninterrupted infrastructure. These factors directly affect the integrity and timely delivery of biologics, even in the absence of explicit trade restrictions. [13]
Air transport-critical for high-value, time-sensitive medicines-has also been affected by geopolitical instability. Airspace closures and conflict-related restrictions reduce available cargo routes and increase reliance on longer, less efficient paths. Industry reports highlight that such disruptions place additional strain on pharmaceutical supply chains, particularly for temperature-sensitive products requiring strict environmental control throughout transit. [14]
For LMICs, the consequences are amplified. With limited local fractionation capacity and heavy reliance on imported PDMPs, any disruption in transport routes translates directly into delayed or reduced access. In this context, the absence of a formal embargo does not equate to supply stability. Instead, access is constrained through logistics-creating a de facto restriction on availability without any explicit policy action.
This dynamic reframes how supply risk must be understood. The challenge is no longer limited to production or procurement, but extends to the resilience of global transport networks. In effect, plasma-derived therapies can become inaccessible not because they are unavailable globally, but because they cannot move reliably across an increasingly fragmented and unstable logistical landscape. [15]
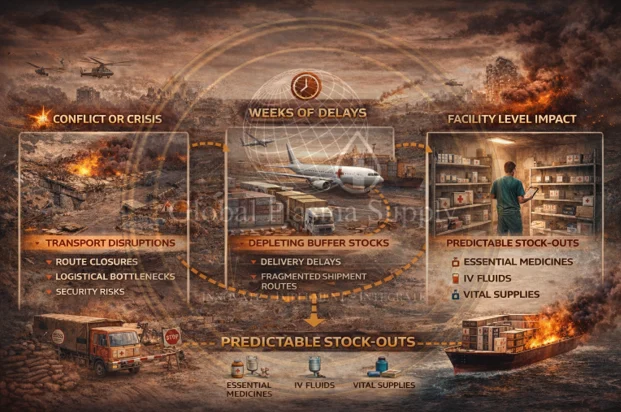
Humanitarian supply chains show the mechanism in fast‑forward
Humanitarian supply chains provide a compressed, real-time view of how disruption translates into medical scarcity.
In conflict and crisis settings, essential medicines-including temperature-sensitive biologics-are frequently delayed for extended periods due to access constraints, infrastructure damage, and logistical bottlenecks. Reports consistently show that shipments of critical medical supplies can be stalled for weeks, with interruptions in transport corridors and administrative barriers compounding delays. These disruptions do not remain isolated events; they translate directly into predictable stock-outs at the facility level, where continuity of care becomes impossible to sustain. [16]
The mechanism is well-documented across humanitarian operations. As supply chains become fragmented, lead times increase, buffer stocks are depleted, and resupply cycles fail to keep pace with clinical demand.
UNICEF and WHO logistics guidance highlights that even short-term disruptions in fragile settings rapidly escalate into systemic shortages, particularly for essential medicines requiring controlled storage and continuous availability. In such environments, stock-outs are not unexpected failures-they are the predictable outcome of prolonged disruption in already constrained systems. [17]
This dynamic mirrors, in accelerated form, what occurs more quietly in global PDMP supply chains. While humanitarian settings expose the mechanism rapidly, the same principles apply more broadly: when transport reliability declines and supply chains fragment, access to critical therapies deteriorates-not abruptly, but progressively, until shortages become embedded within the system. [18]
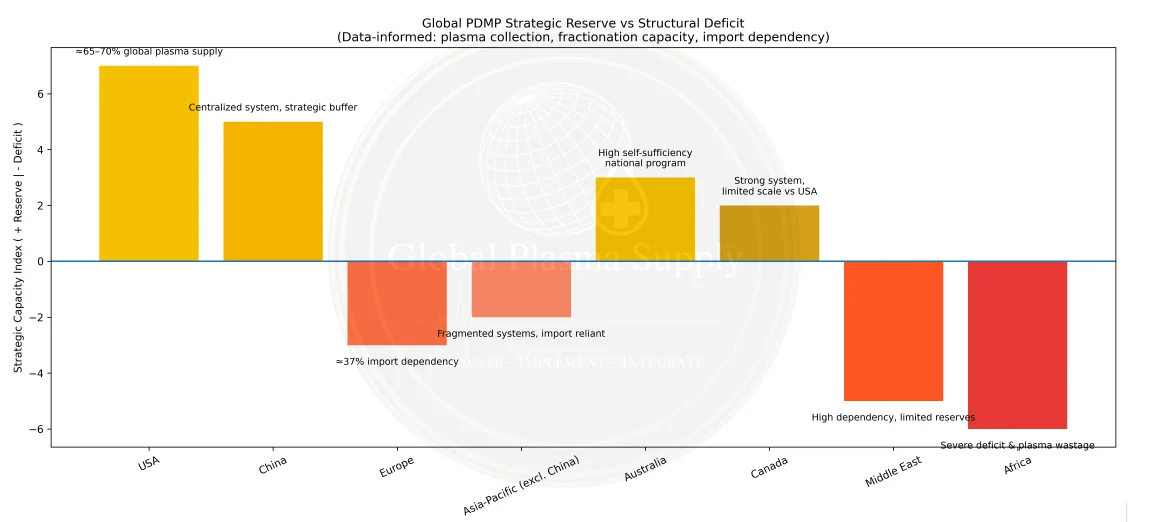
‘Strategic reserves’ shouldn’t be only petroleum
Strategic reserves have long been associated with energy security, yet the same logic applies to essential medicines and their upstream inputs. Frameworks such as the International Energy Agency’s strategic petroleum reserves demonstrate how coordinated stockpiling can buffer supply shocks, stabilize access, and provide time for system response during crises. By contrast, medicines-particularly plasma-derived therapies-remain largely outside formal strategic reserve structures, despite their critical role in sustaining life and health systems. [19]
Global health authorities have increasingly emphasized the need to treat essential medicines as part of national and international preparedness strategies.
The World Health Organization highlights that shortages of critical health products-including biologics-are becoming more frequent and that resilient supply systems must include stockpiling, diversified sourcing, and emergency preparedness mechanisms rather than relying solely on procurement cycles. [7]
This gap is particularly significant for plasma and plasma-derived medicinal products. Given long production lead times, complex fractionation processes, and dependence on stable logistics, plasma cannot be rapidly scaled in response to sudden demand spikes. Without strategic reserves or upstream buffering mechanisms, systems remain exposed to disruption-where delays in collection, processing, or transport translate directly into reduced availability of finished therapies. In this context, preparedness must extend beyond purchasing power to include structured reserve strategies that recognize plasma as a critical, time-sensitive biological resource. [20]
Life – The only metric
A new metric is needed-one that forces the world to look beyond Brent and toward what is already happening in silence.
A Patient Exclusion Index to track, in real time, the consequences of plasma scarcity: missed doses, non-initiations, and therapeutic substitution. These are not theoretical outcomes. In documented immunoglobulin shortages, up to 78% of patients required treatment modification, with delays, dose reductions, and even interruptions of therapy, leading to measurable clinical deterioration. [21] [22]
And yet, there is no global signal for this.
The world watches oil. It reacts, recalibrates, and mobilizes within hours when Brent moves. But plasma-this essential biological resource-remains largely invisible, even as shortages disrupt care across continents. Hospitals run low, therapies are rationed, and patients are switched, delayed, or simply not treated at all.
This is the imbalance we must confront.
Yes, Brent matters. It may shape economies, influence markets, and reflect geopolitical tension. But plasma scarcity is already doing something far more immediate-it is withdrawing care, one patient at a time. While the world tracks energy with precision, it fails to track the absence of treatment with the same urgency.
This must change.
We must begin to track plasma with the same discipline, visibility, and responsiveness. We must measure not only what is produced or traded, but what is missed, delayed, or denied. The system must evolve toward a single, uncompromising standard:
A new metric: Life – the only metric we should be tracking. Track missed doses, track non-initiations, track therapeutic substitution – as routinely as fuel prices.
Because in the end, the true signal is not the price of a barrel. It is the presence – or absence – of care.

Stay updated on all scientific advances with Hemostasis Today.
-
Jun 9, 2026, 17:55Can We Prevent Postpartum Blood Clots without Putting Most Women on Heparin? – RPTH Journal
-
Jun 9, 2026, 17:54Lucky Oseghale Oloboh: Health Is Power, Health Is Personal, and Health Is Our First Responsibility in Life’s Journey on Mother Earth
-
Jun 9, 2026, 17:53Ajay Samkaria: How ABO Subgroups Directly Impact Transfusion Safety
-
Jun 9, 2026, 17:51Alejandro González Veliz: Most Reported Aspirin Allergies Are Not True Hypersensitivity
-
Jun 9, 2026, 17:50Mary Cushman: It’s Time to Apply to Be on an ISTH SSC
-
Jun 9, 2026, 15:56Wolfgang Miesbach: A New Genetic Perspective on the Worldwide Burden of von Willebrand Disease
-
Jun 9, 2026, 15:34Shanon Marie Corsino: Nationwide Insights into Cancer-Associated Thrombosis in Filipino Patients
-
Jun 9, 2026, 15:20Murtuza Ali: Types of Blood Transfusions – A Quick Clinical Guide
-
Jun 9, 2026, 15:18Mital Jhaveri: TRACK Trial Findings Highlight the Unique Challenges of Advanced CKD

