
Heghine Khachatryan: Homocysteine – A Small Molecule with Big Clinical Consequences
Heghine Khachatryan, Editor-in-Chief of Hemostasis Today, Head of Hemophilia and Thrombosis Center at Yeolyan Hematology and Oncology Center, shared a post on LinkedIn:
“Homocysteine: a small molecule with big clinical consequences
Homocysteine is an amino acid formed during the metabolism of methionine, which we obtain from protein-rich foods (eggs, meat, fish, cheese, rice, soy, etc.). On its way through metabolic pathways, homocysteine should either be converted to glutathione – our key intracellular antioxidant – or to SAMe (S-adenosylmethionine), a universal methyl donor involved in hundreds of reactions.
Both pathways depend on adequate levels of specific cofactors:
- For homocysteine → glutathione: vitamins B2, B6 and zinc
- For homocysteine → SAMe: vitamins B2, B6, B9, B12, zinc, magnesium and trimethylglycine (TMG, betaine)
When these cofactors are deficient, the reactions slow down, homocysteine accumulates, and we face hyperhomocysteinaemia. In addition to nutritional deficiency, functionally significant variants of the MTHFR gene can impair conversion of folic acid to methylfolate and further disturb homocysteine metabolism.
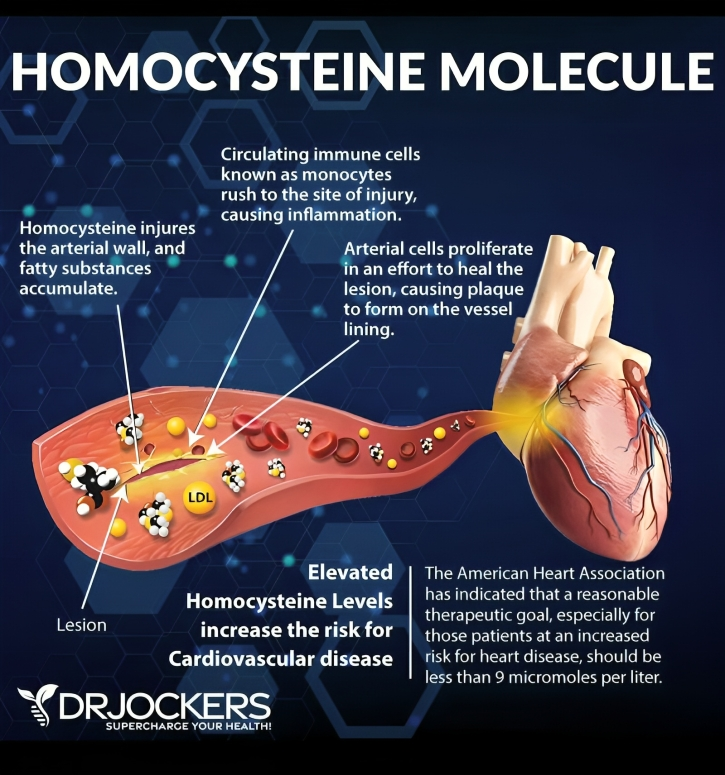
From a clinical perspective, persistently elevated homocysteine (ideally we aim for <8–9 µmol/L; >20 µmol/L is considered high risk) is associated with:
- Ischaemic stroke
- Alzheimer’s and other dementias
- Parkinson’s disease
- Schizophrenia and other neuropsychiatric disorders
- Atherosclerosis and cardiovascular disease
- Osteoporosis
- Adverse pregnancy outcomes
What can we do in practice?
- Measure homocysteine in appropriate risk groups.
- Assess and correct deficiencies of B-group vitamins, zinc and magnesium (through diet and, when necessary, supplementation).
- Consider the impact of smoking, chronic stress and polypharmacy on micronutrient status.
- In selected cases, evaluate for MTHFR variants and adapt folate therapy (e.g. methylfolate) accordingly.
Homocysteine is a simple marker that sits at the intersection of nutrition, genetics and vascular risk. It deserves more attention both in routine clinical practice and in patient education.”
Stay informed with Hemostasis Today.
-
Apr 30, 2026, 12:45Chokri Ben Lamine: Methemoglobinemia in Hematology – Causes, Diagnosis, Antidote
-
Apr 30, 2026, 08:11Navya Sree: Breaking Down DVT From Theory to Practice
-
Apr 30, 2026, 06:06Shashank Joshi: The Emerging Role of Inflammatory Biomarkers in Acute CVS Thrombosis
-
Apr 30, 2026, 05:30John Bramble: Ensuring Safe AI Integration in Medicine
-
Apr 30, 2026, 04:55Danielle Stull: Raising Awareness of CVS Thrombosis in Young Women
-
Apr 29, 2026, 17:25Robert Brodsky: Ravulizumab Appears To Be Safe And Effective In Pregnancy
-
Apr 29, 2026, 16:53Chokri Ben Lamine: IV Iron Showdown – FCM vs Ferric Derisomaltose vs Iron Dextran
-
Apr 29, 2026, 16:46Deep Vein Thrombosis Risk in Jobs with Prolonged Sitting – NBCA
-
Apr 29, 2026, 16:41Vikramaditya Gangakar: Essential Pharmacy Facts You Should Know About Aspirin

