
David Ferreira: Identifying the True Drivers of Recurrent Thrombosis
David Ferreira, Director of the Immuno-hemotherapy Service at ULSGE at Gaia and Espinho Local Health Unit, shared a post on LinkedIn:
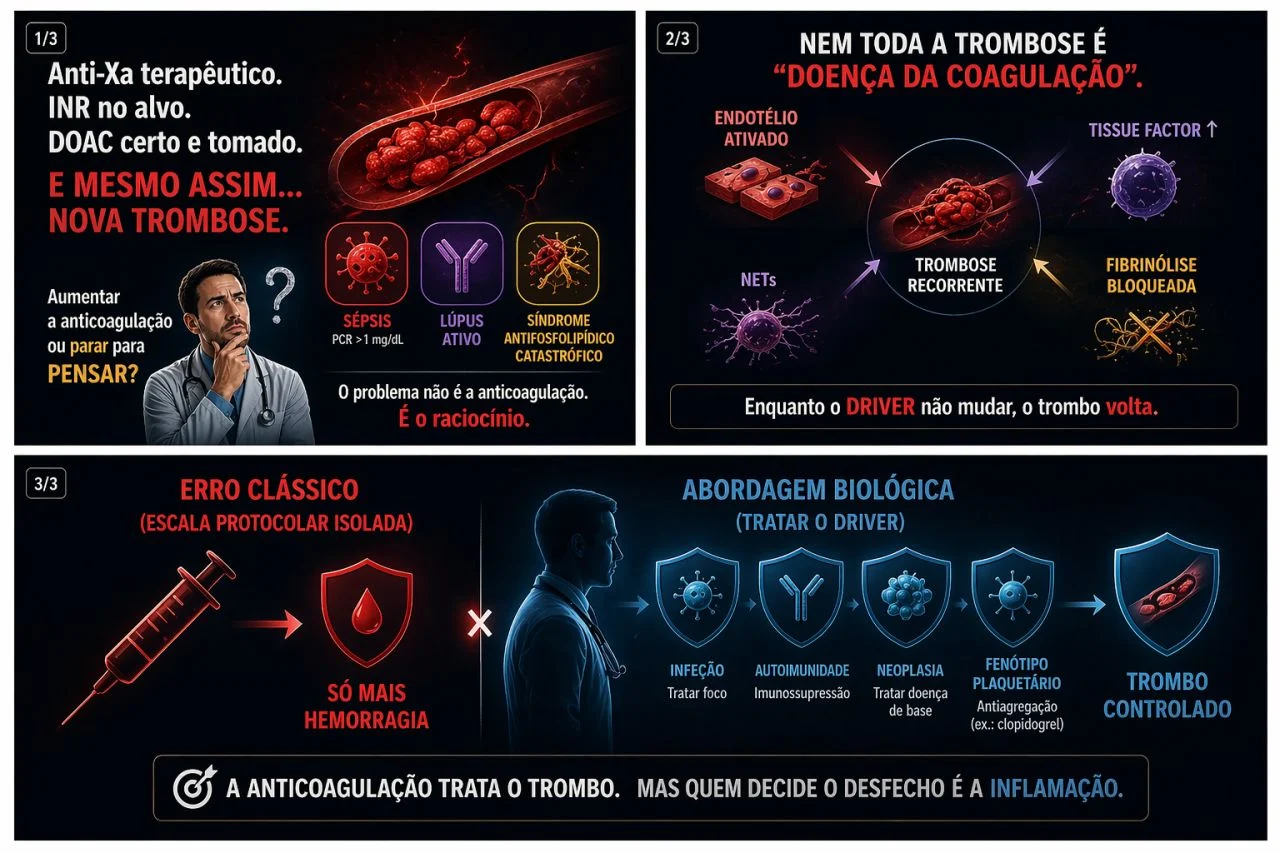
“Therapeutic anti-Xa.
INR on target.
DOAC in the right dose — and taken.
And yet… new thrombosis.
What now?
Increase hypocoagulation?
Change drugs?
Or stop for 30 seconds to think?
There is a pattern that repeats itself — and is rarely questioned: thrombosis patient – correct hypocoagulation – new thrombosis – escalate or change hypocoagulation.
Three very real examples:
- Sepsis. Activated endothelium, systemic inflammation.
Will it solve with more hypocoagulation? - Lupus Flare/ Immune system in overdrive.
Will it solve with more hypocoagulation? - Catastrophic antiphospholipid syndrome (or similar phenotype). Cascading microthrombosis, consumption.
Will it solve with more hypocoagulation?
The problem is not hypoglutilation.
It is the reasoning. We increased doses. We changed drugs.
Because these patients are not thrombosing due to ‘lack of anticoagulant.’
They are thrombosing because:
- Activated endothelium
- High tissue factor
- NETs
- blocked fibrinolysis
In a word – Thrombo-Inflammation!
The system is thus mandatorily programmed to thrombo.
And how do we respond?
More hypocoagulation, hypocoagulant exchange.
This is not therapeutic failure.
It is conceptual failure.
The right question is not ‘What’s the next hypocoagulant?’, but ‘What is fueling this thrombosis?’
And in practice, what changes?
Confirm that you are well hypocoagulated.
Search for the driver.
And then act where it matters:
- Sepsis/infection – aggressive focus control
- Active autoimmune disease – immunosuppression (e.g., corticosteroids) plus/minus targeted therapy
- Severe antiphospholipid syndrome – combined approach (hypocoagulation plus immune modulation depending on context)
- Active neoplasm – treat the underlying disease
- Arterial/platelet phenotype – consider antiplatelet therapy (e.g., clopidogrel) in an appropriate context
Hypocoagulation continues.
But it is no longer the center of the strategy.
Because the reality is this:
Hypocoagulation treats the thrombus.
But who decides the outcome… it is inflammation.
If this bothers you, great.
It’s supposed.
At the end of the day, the most important thing about auscultation is not the stethoscope.
It is between the ears of those who wear it.”
Stay updated with Hemostasis Today.
-
Apr 23, 2026, 08:05Hugo Antonio Romo Rubio: Biology, Function, and Updated Classification of von Willebrand Disease
-
Apr 23, 2026, 07:50Hassan Raza: A Smarter Risk Prediction in MPNs Using AI
-
Apr 23, 2026, 05:32Why TXA and rFVIIa Are Not Equivalent in Trauma Bleeding Control – RPTH Journal
-
Apr 23, 2026, 04:08Suraj Mali: Pune Team Initiative for World Hemophilia Day 2026 Advances Early Diagnosis in Hemophilia
-
Apr 23, 2026, 03:58Adam Ho: What Does It Actually Mean to ”Prevent” a Stroke?
-
Apr 23, 2026, 03:49Jakob Krebs Christensen: Mobile Stroke Units Bring Imaging and Treatment Directly to the Patient
-
Apr 23, 2026, 03:30Kimberly Waddell: Mismatch in Post-Stroke Discharge Decisions Impacts Long-Term Recovery
-
Apr 23, 2026, 03:18Pablo Corral: Key Take‑Home Messages on Familial Hypercholesterolemia
-
Apr 23, 2026, 03:17Wolfgang Miesbach: The Haemophilia A Gene Therapy Story Is Moving from West to China

