
Pooja Choradia: Recognizing Pulmonary Embolism in Pregnancy Before It Is Too Late
Pooja Choradia, Critical Care Associate at P.D. Hinduja Hospital Khar, shared a post on LinkedIn:
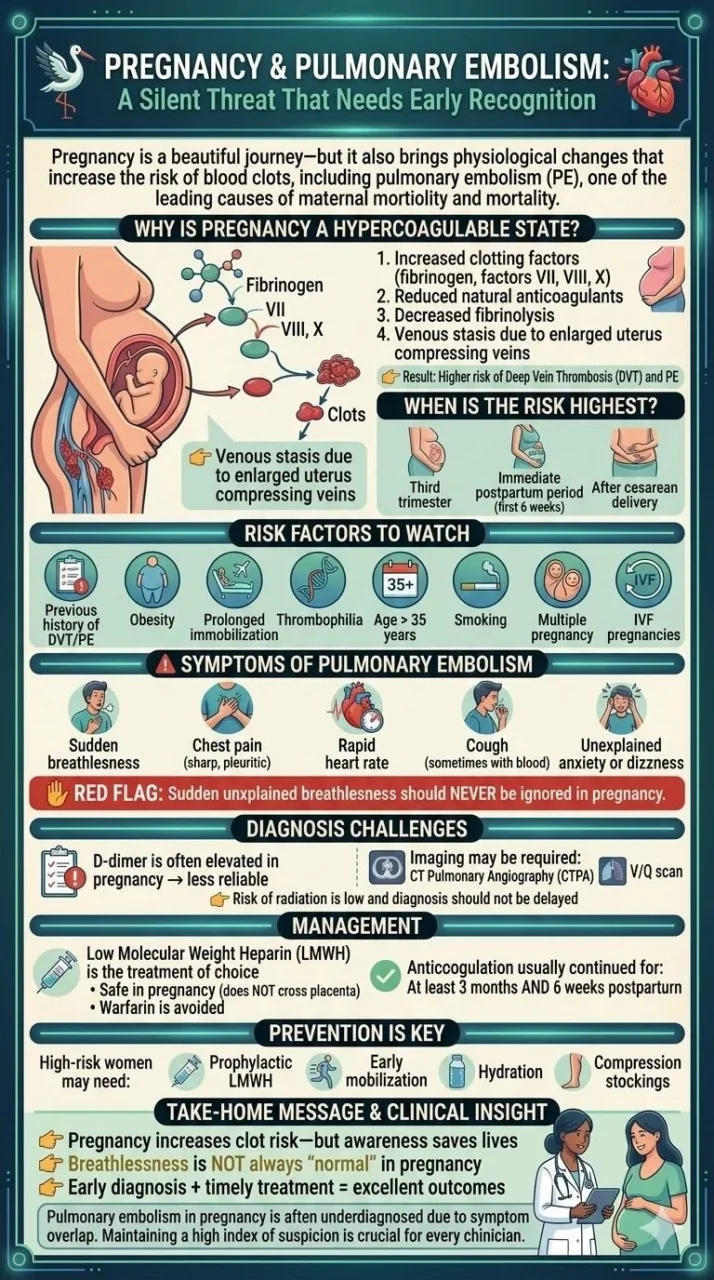
“Pregnancy and Pulmonary Embolism
A Silent Threat That Needs Early Recognition
Pregnancy is a beautiful journey—but it also brings physiological changes that increase the risk of blood clots, including pulmonary embolism (PE), one of the leading causes of maternal morbidity and mortality.
Why is pregnancy a hypercoagulable state?
During pregnancy, the body naturally prepares to prevent excessive bleeding during delivery.
This leads to:
- Increased clotting factors (fibrinogen, factors VII, VIII, X)
- Reduced natural anticoagulants
- Decreased fibrinolysis
- Venous stasis due to enlarged uterus compressing veins
Result: Higher risk of deep vein thrombosis (DVT) and PE
When is the risk highest?
- Third trimester
- Immediate postpartum period (first 6 weeks)
- After cesarean delivery
Risk factors to watch
- Previous history of DVT/PE
- Obesity
- Prolonged immobilization (bed rest, travel)
- Thrombophilia (inherited/acquired)
- Age more than 35 years
- Smoking
- Multiple pregnancy
- IVF pregnancies
Symptoms of pulmonary embolism
Symptoms can be subtle and often overlap with normal pregnancy changes—making diagnosis tricky.
Look out for:
- Sudden breathlessness
- Chest pain (sharp, pleuritic)
- Rapid heart rate
- Cough (sometimes with blood)
- Unexplained anxiety or dizziness
Red flag: Sudden unexplained breathlessness should Never be ignored in pregnancy.
Diagnosis challenges
D-dimer is often elevated in pregnancy – less reliable.
Imaging may be required:
- CT Pulmonary Angiography (CTPA)
- V/Q scan
Risk of radiation is low and diagnosis should not be delayed
Management
Low molecular weight heparin (LMWH) is the treatment of choice.
- Safe in pregnancy (does NOT cross placenta)
Warfarin is avoided during pregnancy.
Anticoagulation usually continued for:
- At least 3 months
- And 6 weeks postpartum
Prevention is key
High-risk women may need:
- Prophylactic LMWH
- Early mobilization
- Hydration
- Compression stockings
Take-home message
- Pregnancy increases clot risk – but awareness saves lives
- Breathlessness is not always ‘normal’ in pregnancy
- Early diagnosis plus timely treatment equals excellent outcomes
Clinical insight
Pulmonary embolism in pregnancy is often underdiagnosed due to symptom overlap.
Maintaining a high index of suspicion is crucial for every clinician.”
Stay updated with Haemostasis Today.
-
May 31, 2026, 16:29José Antonio García Erce: Collaborative PBM Implementation in Transfusion Centers and Services
-
May 31, 2026, 16:22Vera Ignjatović: How Do We Rigorously Study These Drugs in Children to Understand Their True Benefits and Risks?
-
May 31, 2026, 16:21Ksenija Stach: Is This The Future of Lipid-Lowering Lherapy?
-
May 31, 2026, 15:42Antonio Greco: Balancing Bleeding and Thrombotic Risk After PCI
-
May 31, 2026, 15:41Eric Topol: Replication of Plasma p-tau217 Blood Test for Predicting Alzheimer’s Disease
-
May 31, 2026, 15:32ASH Invites Dynamic Members to Apply for 2027 Leadership and Committee Roles
-
May 31, 2026, 14:39Monique Gore-Massy: Redefining Lupus Innovation Through Patient Partnership
-
May 31, 2026, 14:31Mirjam Teboe: The Golden Rule Behind Reliable Lupus Anticoagulant Testing
-
May 31, 2026, 14:20Improving Access to Care for People Living with Haemophilia and Haemoglobinopathies – NNHF

