
Tareq Abadl: Detecting the Hidden Risk of NAIT in the Lab
Tareq Abadl, Medical Laboratory Specialist and Director of the Blood Bank at Dr. Abdelkader Al-Mutawakkil Hospital, shared a post on LinkedIn:
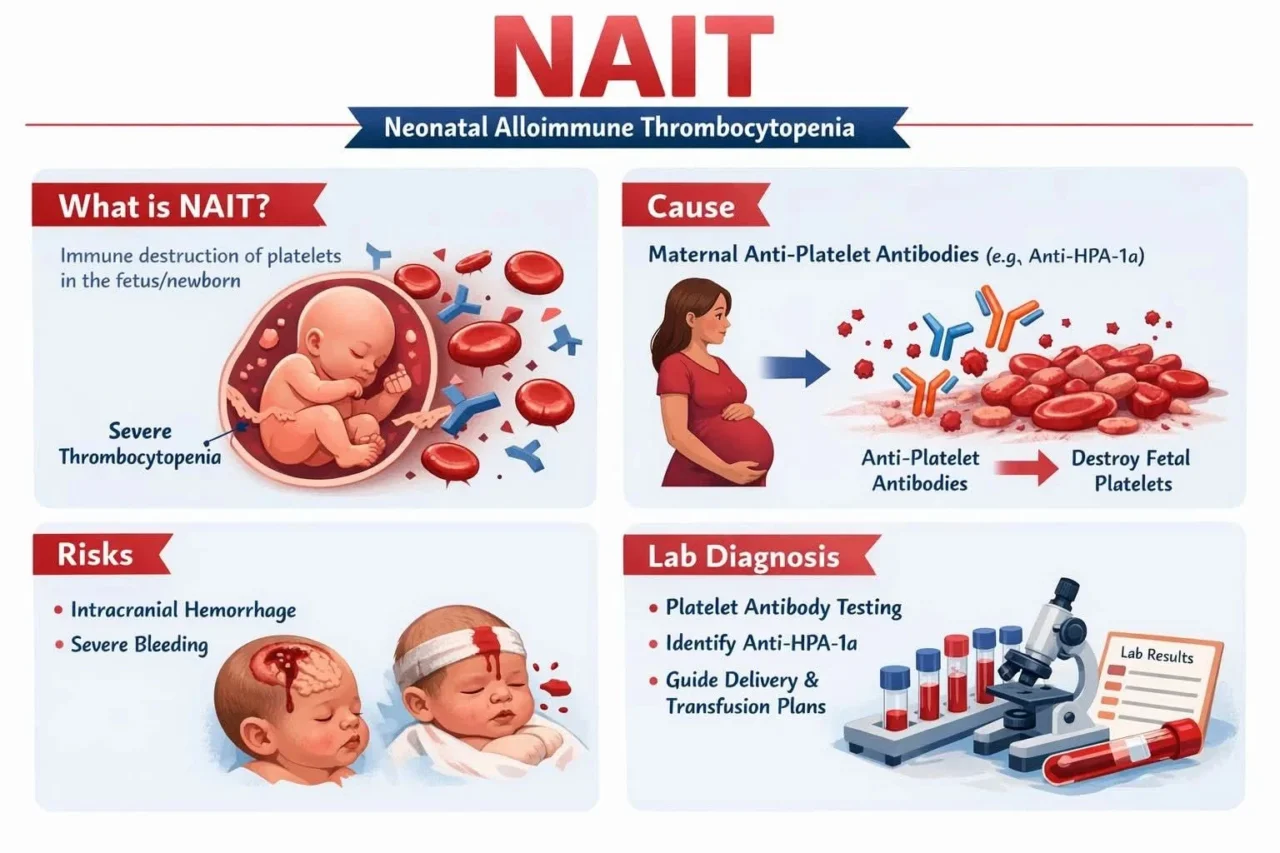
“NAIT (Neonatal Alloimmune Thrombocytopenia): When the Lab Detects the Hidden Risk.
Neonatal Alloimmune Thrombocytopenia (NAIT) is a condition where the fetus or newborn develops severe thrombocytopenia due to maternal anti-platelet alloantibodies.
The most common antibody involved is anti-HPA-1a.
Although rare, NAIT can lead to severe neonatal thrombocytopenia and intracranial hemorrhage, making early laboratory recognition critical.
In many cases, the laboratory alert is what changes the delivery and transfusion plan.
Top red flags the lab should recognize
- History of a previously affected infant: A mother with a prior baby who had unexplained thrombocytopenia or neonatal bleeding should raise suspicion for NAIT.
- Severe thrombocytopenia at birth: Platelet count less than 50 × 10⁹/L in a newborn without an obvious cause.
Clinical signs in the newborn
- Petechiae
- Unexplained bruising
- Bleeding shortly after birth
These findings require immediate communication with neonatology and the transfusion service.
What the laboratory must do — STAT
Maternal and cord blood testing
Send the following samples urgently:
- EDTA blood – CBC plus Peripheral Blood Smear
- Evaluate platelet count and morphology
- Add smear comments if present: petechiae, bleeding signs
Anti-Platelet Antibody Testing
Collect and freeze samples for specialized testing:
- Maternal serum (plain tube)
- Test for anti-HPA antibodies
- especially anti-HPA-1a
Many reference laboratories require frozen serum aliquots, so early preparation saves critical time.
Key diagnostic tests
1. Maternal Anti-Platelet Antibody Screen
Detects antibodies such as:
- Anti-HPA-1a
- Other anti-HPA antibodies
Sent urgently to a reference immunohematology laboratory.
Clinical care should not wait for these results.
2. HPA Genotyping
Performed for:
- Mother
- Father
This test identifies platelet antigen incompatibility between parents and helps guide the selection of compatible platelet donors for the neonate.
Platelet transfusion strategy
If the neonate requires transfusion: HPA-compatible platelets are preferred.
Alternative option:
Maternal platelets
These must be prepared according to transfusion protocols:
- Washed
- Treated as required
- Irradiated if indicated
Proper documentation and preparation by the transfusion service is essential.
Practical bench tips that save time
- Freeze maternal serum early
Many reference labs require frozen samples with minimal handling.
- Document obstetric history clearly
Include details of previous pregnancies and neonatal outcomes on the request form.
- Maintain a list of HPA-compatible platelet donors
Or the nearest reference transfusion service that can provide compatible units quickly.
In suspected NAIT, minutes matter.
Why This Matters? In suspected NAIT, the laboratory plays a central role in early detection, diagnosis, and management planning.”
Other posts featuring Tareq Abadl on Hemostasis Today.
-
Apr 29, 2026, 07:12Matteo Foschi: Is There a Benefit to Switching DOACs After Breakthrough Stroke?
-
Apr 29, 2026, 07:02Enrico Ferro: Stroke Risk in PFA vs Radiofrequency Ablation
-
Apr 29, 2026, 06:03Proud to Recognize 6 Early Career Investigators as the Recipients of the 2026 JTH Editors’ Awards – JTH
-
Apr 29, 2026, 05:55On Hemophilia Care Advances, Collaboration and Access in India at IHC X 2026 – Hemophilia Federation India
-
Apr 29, 2026, 05:46Rajendra Tapadia: Strengthening Last-Mile Hemophilia Care Through Structured Community Outreach
-
Apr 29, 2026, 05:37Masoabi Sefojane: Whose Realities Shape Global Priorities in Hemophilia Care?
-
Apr 29, 2026, 05:24Filippo Cademartiri: Mandatory Reading for Anyone Who Mistakes Expertise for Certainty
-
Apr 29, 2026, 02:52Fengqian Chen: Another Reality Check for the Factor XI Inhibitor Race – Novartis’ Abelacimab Setback
-
Apr 29, 2026, 02:18Arnaud Baldivia: Peri-Procedural Stroke – An Underestimated Emergency in the Operating Room and in the ICU

