
Hossam Qassem: The Stepwise Investigation Framework for ICU Hemoglobin Drop
Hossam Qassem, ICU Clinical pharmacist at Mabaret AlAsafra Group for Medical Services, shared a post on LinkedIn:
“Hgb dropped 2 g/dL overnight. No visible bleeding.
No bloody output.
Do you transfuse — or do you find out Why
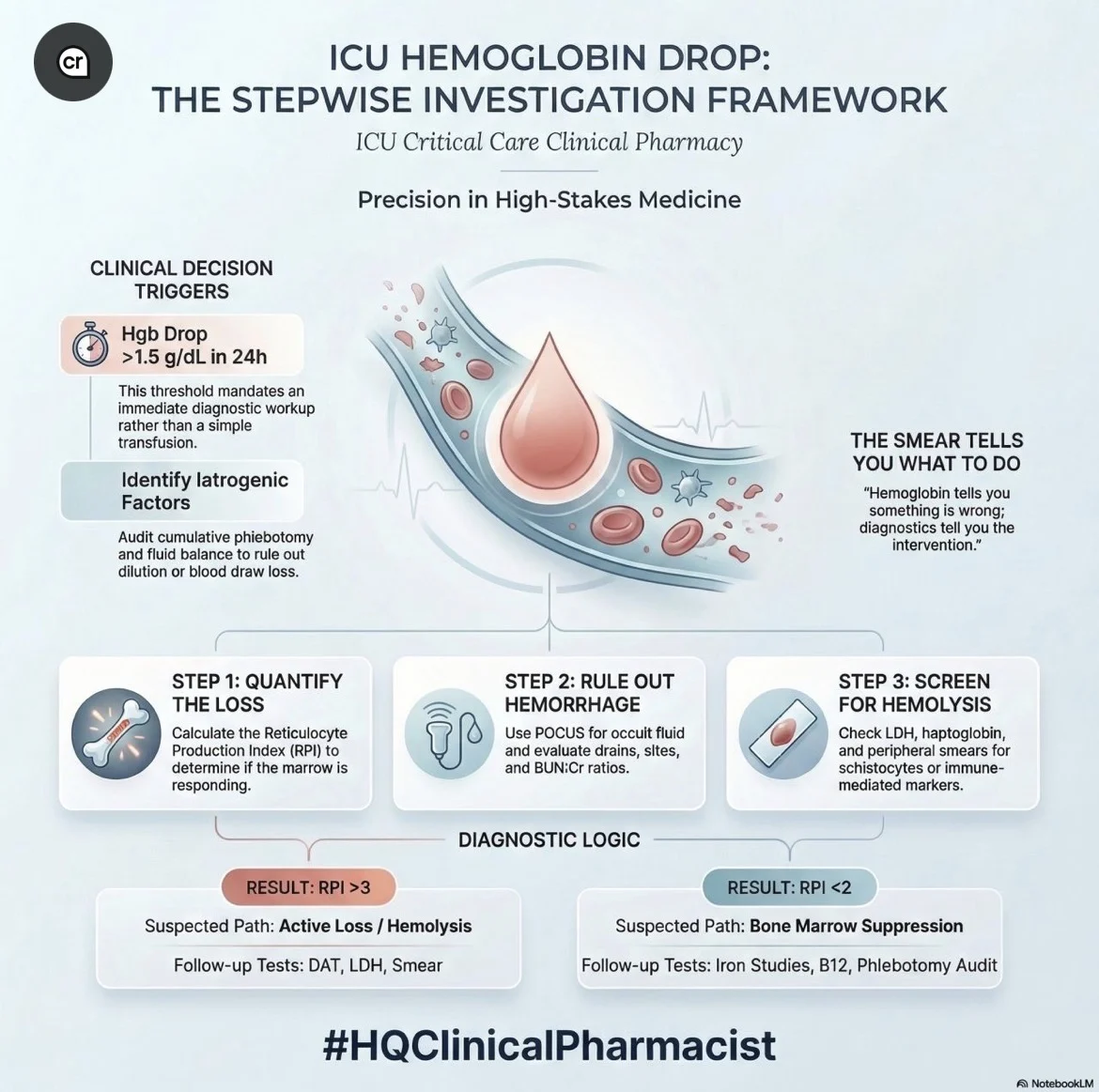
Day 140 – ICU Hemoglobin Drop: The Stepwise Investigation Framework
Why this matters
Unexplained Hgb drop is a diagnostic emergency, not a transfusion trigger.
Missing the cause means missing hemolysis, occult hemorrhage, or iatrogenic loss — all with distinct, time-sensitive workups.
Transfusing without a diagnosis delays correction. And adds harm.
The dilemma
Treat the number OR investigate the cause?
Pattern interrupt: A patient bleeding into a retroperitoneal hematoma or lysing cells in a circuit does not benefit from 2 units of pRBCs without a diagnosis.
The Hgb drop is the symptom.
The investigation is the intervention.
When to investigate urgently
Hgb drop is higher than 1.5 g/dL within 24h indicates the need for mandatory workup
Drop despite recent transfusion suggests active loss OR hemolysis
High HR with Low MAP and falling Hgb should be considered hemorrhage until proven otherwise
Easy to miss: Hgb falling slowly over 3-5 days may reflect cumulative phlebotomy loss or dilution — not ‘just the ICU’
The stepwise investigation
STEP 1 — Quantify (within 1 hour)
- Compare to TRUE baseline — not post-resuscitation Hgb
- Reticulocyte count with Reticulocyte Production Index (RPI)
RPI less than 2 bone marrow not responding (hypoproliferative)
RPI greater than 3 active loss or hemolysis (marrow compensating) - Estimated blood loss is equal to [AHgb divided by Baseline Hgb] multiplied by 70 mL/kg
STEP 2 – Rule Out Hemorrhage (1-2 hours)
Visible sources:
- All drain outputs, wound sites, line insertion points
- NG aspirate if upper GI suspected
- Stool guaiac / rectal exam
Occult hemorrhage:
- POCUS shows free fluid in Morrison’s pouch, splenorenal space
- CT abdomen/pelvis with contrast shows retroperitoneal, hepatic, splenic hematoma
- BUN:Cr greater than 20:1 suggests upper Gi bleed until ruled out
STEP 3 — Rule Out Hemolysis (2-4 hours)
Per ASH 2022:
- High LDH and high indirect bilirubin and haptoglobin less than 25 mg/dL indicates hemolysis confirmed
- Peripheral smear showing schistocytes indicates MAHA (TTP / HUS /DIC)
Direct Coombs (DAT):
- Positive means immune-mediated (AIHA, drug-induced, transfusion reaction)
- Negative means non-immune (mechanical, oxidative, circuit-related)
Review MAR: cephalosporins, piperacillin, NSAIDs added in last 72h?
Post-transfusion drop requires ruling out acute hemolytic transfusion reaction first
STEP 4 — Rule Out Dilution + latrogenic Loss (same day)
- Fluid balance greater than 3L positive suggests dilutional component likely
- Cumulative phlebotomy greater than 150 mL over 72h is clinically significant
Switch to pediatric tubes (reduces draw volume 30-50%) - MCV low prompts ferritin, TIBC and serum iron for iron deficiency
- MCV high prompts B12 and folate evaluation
- ICU stay longer than 7 days with no other cause suggests anemia of critical illness (diagnosis of exclusion)
Pearl:
‘The Hgb tells you something is wrong.
The smear and the retic tell you what to do about it.'”
Stay updated with Hemostasis Today.
-
May 6, 2026, 14:58Insights on Acquired Hemophilia from ‘Bobby’ Duc Tran – Hemophilia of Georgia
-
May 6, 2026, 14:57Amanda S.: Strengthening the Global Network of Psychosocial Professionals in Bleeding Disorders at WFH 2026
-
May 6, 2026, 14:56Sierra Akers: Discussing the importance of Hemophilia Treatment Centers
-
May 6, 2026, 14:52Christy Abele: Helping People Craft Stories That Connect and Resonate at CHB Symposium
-
May 6, 2026, 14:46Joe Dawson: Follow-Up on a Patient with a History of an IVC Thrombus
-
May 6, 2026, 14:20Emmanuel J. Favaloro: Highlights of Global Haemostasis Testing in the Latest Issue
-
May 6, 2026, 14:02Abdul Mannan: Anemia in Myelofybrosis – Five Fires Behind One Falling Hb
-
May 6, 2026, 14:00Mona Alfaraj: Advancing Care in Inherited Platelet Disorders at 2nd International Hematology and Hemostasis Conference
-
May 6, 2026, 13:56Mahesan Subramaniam: Why Delayed Cord Clamping Benefits Newborn Health

