
Arun V J: Do You Know What SDP or Apheresis Platelet Is?
Arun V J, The Leader of Transfusion Medicine at Malabar Medical College, shared on LinkedIn:
”Do You Know What SDP or Apheresis Platelet Is?
Most doctors, donors, and even healthcare workers don’t truly understand what an SDP is — or how it’s different from an RDP.
Because when we misunderstand science, patients pay the price.
First, what are we talking about?
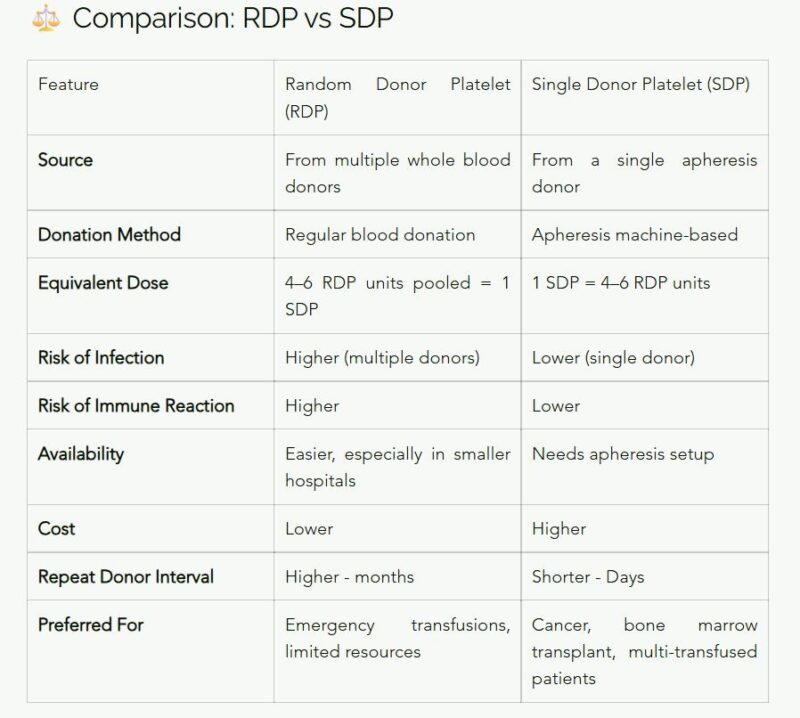
RDP (Random Donor Platelet):
Platelets separated from whole blood donations.
A single unit gives a small platelet yield.
So, for one patient, you usually pool platelets from 4–6 different donors to reach the required dose.
SDP (Single Donor Platelet):
Collected through apheresis, where a machine selectively removes platelets and returns the rest of your blood.
One SDP = 4–6 RDPs in platelet count — but from one donor only.
Why this matters
- When a patient receives RDPs, they’re exposed to multiple immune systems.
- Each donor’s platelets have different antigens.
- This increases risks like immune reactions and platelet refractoriness (when the patient stops responding to transfusions).
- SDP minimizes this risk.
That’s why it’s preferred for cancer patients, bone marrow transplants, and those needing repeated transfusions — not for “faster rise.”
Why SDP Costs More
- It’s not “premium blood.”
- The cost includes sterile single-use kits, apheresis machine use, longer donation time, and trained personnel.
- But it gives safer platelets, traceable donors, and fewer complications.
Common Myths (Let’s Bust Them)
Myth 1: “SDP gives faster platelet count rise.”
False. Rise depends on the patient’s body, not platelet type.
Myth 2: “SDP is only for rich people.”
False. Many hospitals subsidize or cover it under insurance.
Myth 3: “SDP donation is painful.”
False. It’s smooth, safe, and you get your red cells back.
The Bigger Picture
- In developed countries, apheresis platelets are the standard.
- In India and similar regions, we’re still transitioning — mainly because of awareness gaps & cost of technology.
- If every doctor and donor understood the difference, we’d save time, cost, and lives.
The Third Thinker Takeaway
- Blood donation isn’t just kindness.
- It’s applied science.
- Every time you donate — or prescribe — you shape someone’s tomorrow.
Because better understanding leads to better care.
Read the detailed version here.
If you learned something new, drop a or share it — more awareness means fewer misconceptions, and more lives saved.”
Stay updated with Hemostasis Today.
-
May 27, 2026, 17:51Nita Radhakrishnan: Post Graduate Institute of Child Health Receives WFH Data Quality Certification for Excellence
-
May 27, 2026, 17:51Fiona Robinson: What exactly Are Rebalancing Agents for Bleeding Aisorders?
-
May 27, 2026, 17:14Khurram Nasir: Can Earlier LDL-C Lowering Change the Trajectory of Cardiovascular Disease?
-
May 27, 2026, 17:09Yvonne Jongejan: Allele-Selective Silencing Therapy for VWD and Thrombotic Disorders
-
May 27, 2026, 16:58Catherine Moran: Important Step Forward as 1st WHO Resolution on Stroke Gets Adopted at WHA79
-
May 27, 2026, 16:08Heghine Khachatryan: Thrombosis in Oncology Remains a Major Healthcare Burden
-
May 27, 2026, 16:00Revealing Critical Gaps in Hemophilia Diagnosis and Access to Care in India – WFH
-
May 27, 2026, 16:00Melissa Hollo: Women Deserve Proactive Care, Not Reactive Care
-
May 27, 2026, 15:59Piotr Czempik: First Report of ROTEM Findings in Triple-Positive APS and Hageman Anomaly

