
Wolfgang Miesbach: From Heparin to Vaccines – The Expanding Biology of Anti-PF4 Immunothrombosis
Wolfgang Miesbach, Professor of Medicine at Frankfurt University Hospital, shared a post on LinkedIn:
”Anti-PF4 Immunothrombosis: From HIT to VITT and Beyond – Andreas Greinacher and Linda Schönborn (Greifswald University Hospital) delivered one of the standout sessions of the 70th GTH Annual Meeting, tracing the full spectrum of anti-PF4 immunothrombosis:
How PF4 becomes immunogenic:
PF4 (CXCL-4), a positively charged tetrameric protein stored in platelet α-granules, forms immunogenic complexes with polyanions.
This drives FcγRIIA-mediated platelet activation to thrombin generation – thrombosis with thrombocytopenia.
The same mechanism links three clinical entities:
- Classic HIT — triggered by heparin/PF4 complexes
- VITT — triggered by adenoviral vector-based COVID-19 vaccines, 5–30 days post-injection, causing thrombosis at unusual sites
- Spontaneous HIT — autoantibodies activate platelets even without heparin or any polyanion
- HIT antibodies are not VITT antibodies — they bind distinct epitopes on PF4, a critical distinction for diagnosis and management.
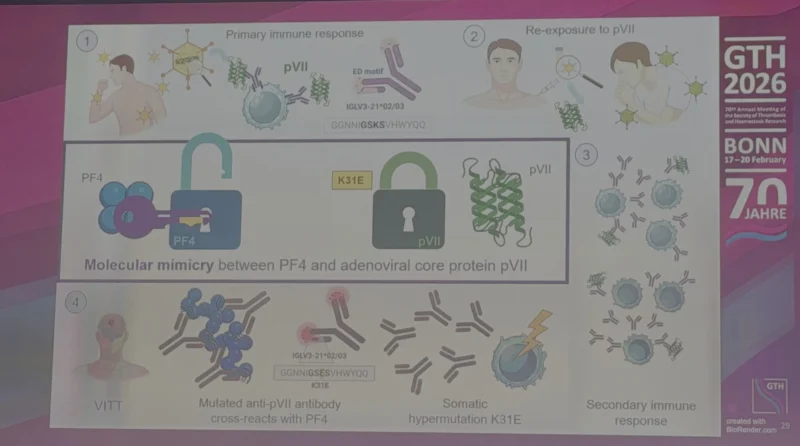
New insights: molecular mimicry plus somatic mutation.
Molecular mimicry between PF4 and adenoviral core protein pVII is the trigger.
In individuals carrying the IGLV3-21*02/03 light chain haplotype (~60% of Caucasians), primary exposure to pVII generates an antibody with an ED motif.
Upon re-exposure, a somatic K31E hypermutation creates an antibody that cross-reacts with PF4 — triggering VITT via a clonal secondary immune response.
These findings just published in N Engl J Med 2026.
Broader implications
This model also illuminates acquired haemophilia post-vaccination, postinfectious APS, ITP in children, posttransfusion purpura, and more.
For future adenoviral vaccine platforms — Ebola, HIV, Zika, Rabies — modifying pVII in the vector could prevent VITT entirely.”
Stay updated with Hemostasis Today.
-
Apr 29, 2026, 16:17W. Alberto Sifuentes Giraldo: Non-Criteria Manifestations of Antiphospholipid Syndrome
-
Apr 29, 2026, 16:12Mavis Agnes Kisakye: Concluding a Successful Entrepreneurship Training for Our Mothers
-
Apr 29, 2026, 15:48Kriti Batni: Happy to Share on Our Chapter Being Published in Medicine Update 2026
-
Apr 29, 2026, 15:46Dima Shulkin: Comparing HALP and PIV for Mortality Prediction in ACS
-
Apr 29, 2026, 15:44Sonal Sonu: Securing First Prize in Research Oral Presentation at the CME
-
Apr 29, 2026, 15:43Andrew Shaw: Long COVID First Diagnostic Classification with 69% accuracy
-
Apr 29, 2026, 15:41Yazan Abou-Ismail: Contributing Evidence-Based Topic Review on the Evaluation of Easy Bruising
-
Apr 29, 2026, 15:36Mohamed Sherif Salem: Expanding the Role of Tenecteplase in Acute Ischemic Stroke
-
Apr 29, 2026, 15:31WFH Humanitarian Aid Program Reflects on a Result of Years of Consistent Work with AHTA – Yeolyan Hematology and Oncology Center

