
Mazou Ngou Temgoua: Cancer and VTE – Toward Truly Personalized Anticoagulation
Mazou Ngou Temgoua, Cardiology Intensive Care Physician at Châteauroux–Le Blanc Hospital Centre, shared a post on LinkedIn:
“Cancer and VTE: toward a truly personalized (and finally nuanced) anticoagulation
A major meta-analysis (>96,000 patients) provides a key message:
- Not all cancers expose thrombosis vs bleeding to the same balance
- And above all, the profiles are not symmetrical
What the study really shows: getting out of shortcuts
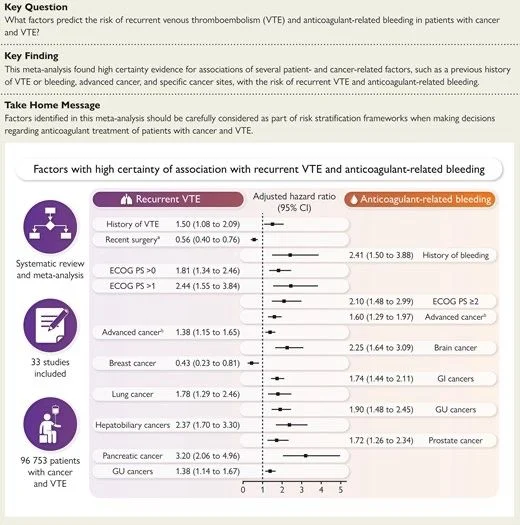
High thromboembolic risk (without necessarily increased bleeding) (e.g. pancreas, hepatobiliary, lung, history of VTE, ECOG >0)
- Dominant pro-thrombotic profile
High bleeding risk (without clear evidence of reduced VTE risk) (e.g. gastrointestinal cancers [non-pancreas/hepatobiliary], brain, prostate, history of bleeding, ECOG ≥2)
- Dominant haemorrhagic profile
- But thrombotic risk is not necessarily low
High dual risk (critical profile) (e.g. cancers of the genitourinary tract, advanced cancer and deterioration of general condition)
- High risk of recurrence and bleeding
Lower risk of recurrence (e.g. recent surgery, breast cancer)
- More favourable profile
- To be recontextualized according to tumor activity
Major implication: reasoning in terms of risk dominance (not simplistic categories)
Dominant thrombotic profile
- Prolonged, intensive anticoagulation (greater than or equal to 6 months, no early reduction)
Dominant bleeding profile
- Cautious, individualized anticoagulation
- Not necessarily short, but adapted to the real context of VTE
High dual risk (the real challenge)
- No standard solution
- Tailor-made strategy:
- LMWH preferred
- Close reassessment
- Multidisciplinary discussion
- Shared decision-making
Lower risk profile (relative)
- Standard anticoagulation
- If active cancer, tendency to still prolong treatment (greater than or equal to 6 months)
What this study really changes
Breaks the simplistic opposition ‘high risk vs low risk’
Shows that some cancers are:
- Purely thrombogenic (pancreas)
- More haemorrhagic (digestive, brain)
- Or mixed (genitourinary)
Bleeding risk does not equal protection against recurrence
Important limitations
Heterogeneity of studies
- Combined factors not assessed
- Absence of biomarkers
- Current scores insufficient
- Uncertain applicability after the acute phase
Key message (essential takeaway)
- The real advance is not to add risk factors
- But to understand their interaction and clinical dominance
Anticoagulation in cancer becomes:
- Dynamic
- Personalized
- Patient-centred
Future progress will require integrated models (clinical, biomarkers, and artificial intelligence) to manage these complex profiles.”
Stay updated with Hemostasis Today.
-
Apr 23, 2026, 13:35Jecko Thachil: Risk Assessment and Clinical Management of Nephrotic Syndrome–Associated Thrombosis
-
Apr 23, 2026, 12:18Mona Ranade: A Contemporary Framework for Managing Right Heart Thrombus in PE
-
Apr 23, 2026, 11:59Strengthening Hemophilia Care Through Collaboration and Commitment in India at IHC X 2026 – Hemophilia Federation India
-
Apr 23, 2026, 08:16David Ferreira: Identifying the True Drivers of Recurrent Thrombosis
-
Apr 23, 2026, 08:05Hugo Antonio Romo Rubio: Biology, Function, and Updated Classification of von Willebrand Disease
-
Apr 23, 2026, 07:50Hassan Raza: A Smarter Risk Prediction in MPNs Using AI
-
Apr 23, 2026, 05:32Why TXA and rFVIIa Are Not Equivalent in Trauma Bleeding Control – RPTH Journal
-
Apr 23, 2026, 04:08Suraj Mali: Pune Team Initiative for World Hemophilia Day 2026 Advances Early Diagnosis in Hemophilia
-
Apr 23, 2026, 03:58Adam Ho: What Does It Actually Mean to ”Prevent” a Stroke?

