
Richard Mason: Cervical Arterial Dissection, Genetics, and Medications – A Safety‑First Approach for Chiropractors
Richard Mason, Educational Consultant at KMC University, shared a post on LinkedIn:
“First time mother presents to our office recently:
Subjective.
A 6-month postpartum 28-year-old female presents with a 2–3-month onset of intermittent dull, achy, stiff/sore pain in the posterior cervical and upper thoracic regions, worsened by poor posture, desk/computer work, stress, and reaching/lifting.
Current pain 6/10 (VAS).
Onset 2–3 months ago after repetitive infant care and lifting.
Occasional non‑persistent headaches; no migraine history; no numbness/tingling in extremities; no recent injuries/falls.
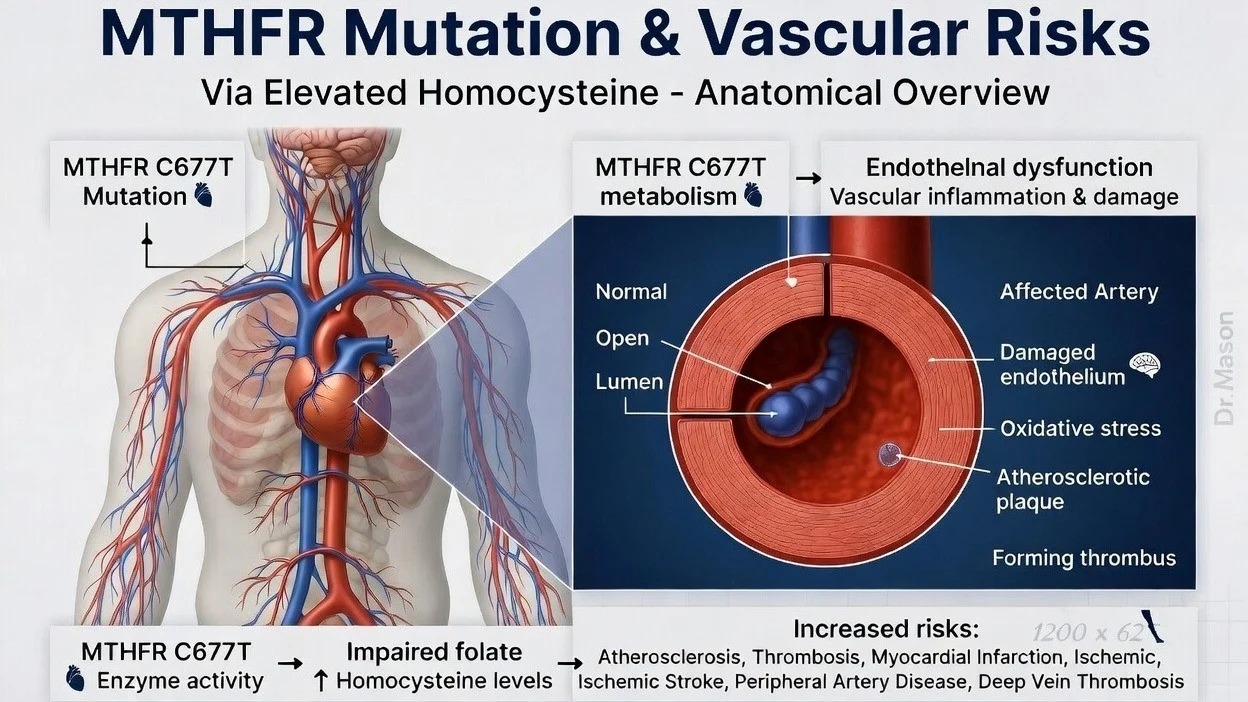
She has taken daily aspirin for nearly 2 years for an MTHFR gene variant associated with thrombosis/cervical arterial dissection risk (prescribed by PCP).
She reports generalized lower‑back/hip tightness that worsens with prolonged standing and infant holding.
Objective.
- Vitals: 97.8°F; HR 83; BP 95/68 seated; well,‑appearing, no distress. Posture: Upper Cross Syndrome; no antalgic posture.
- Segmental restrictions/tenderness: C2, C3, C5–C6, T1–T2, T4–T5; bilateral first ribs; myofascial rigidity in bilateral cervical paraspinals, trapezii, mid‑thoracic, and lumbar regions. Neuro exam: AandO×3; cranial nerves II–XII intact; UE/LE strength 5/5; sensation (C5–T1, L3–S1) intact; DTRs 2plus throughout; Babinski negative; Romberg negative.
- Cervical AROM: flex 50/50, ext 60/60 (no pain); LLF 40/45 and RLF 43/45 with stiffness; L rot 75/80 and R rot 74/80 with stiffness.
- Orthopedic tests: Spurling and foraminal compression reproduce mild local lower cervical pain bilaterally without radicular signs; Distraction, O’Donoghue, Valsalva, Soto‑Hall negative; Lhermitte negative; shoulder depression negative; cervical percussion unremarkable.
- Gait/station: normal, heel/toe WNL.
Why this matters:
This patient is typical of a new mother caring for an infant with posture‑related cervical/thoracic pain – but she also has a genetic thrombophilia marker (MTHFR) and is on antiplatelet therapy.
The latter facts should prompt enhanced vascular risk screening and conservative selection of manipulative techniques.
What We Know About Cervical Artery Dissection (CeAD)
CeAD (vertebral or internal carotid) is rare (nearly 2.6–3.0 per 100,000/year) yet a leading cause of stroke in younger adults, often following minor trauma or infection, and sometimes occurring spontaneously.
Evidence regarding a causal link between cervical manipulation and stroke is inconclusive at the population level; however, pre‑existing vascular vulnerability may modulate risk and warrants clinical caution.
Informed consent and risk stratification remain best practice. [1,7–8]
Genetics and Connective‑Tissue Vulnerability: Spotlight on MTHFR
Large systematic reviews identify genetic factors among CeAD risk contributors – specifically MTHFR C677T TT homozygosity, migraine, connective‑tissue features, and matrix metalloproteinase variation. Certainty is moderate for MTHFR TT and migraine. [1–2]
Early genetic association studies and a meta‑analysis suggest the MTHFR 677TT genotype confers higher odds of CeAD (pooled OR nearly1.6–1.7), with stronger signals in multiple dissections, plausibly via hyperhomocysteinemia and vessel wall fragility. [2–3]
Clinical implication:
When patients volunteer MTHFR status, consider them vascular‑vulnerable and modify cervical procedures accordingly. [1–3]
Medications: Why Antiplatelets/Anticoagulants Should Trigger a Deeper Conversation
In CeAD treatment, both antiplatelet and anticoagulant strategies are used; multiple meta‑analyses and RCT syntheses show no clear overall difference in composite outcomes at 3 months, though anticoagulation may reduce early ischemic stroke at the cost of higher major bleeding in pooled observational plus trial data. [4–5]
What this means in the clinic:
A patient already on daily aspirin does not have a higher manipulation‑specific risk solely due to aspirin, but the prescription signals underlying vascular risk as noted by another provider. That should prompt meticulous history, vascular red‑flag screening, and preference for lower‑force cervical options.
Pre‑Treatment Vascular Screening: What to Do (and What to Stop Doing) [4–5]
Do:
Emphasize history‑based risk assessment (genetic/connective tissue disorders, migraine, recent infection, minor trauma, cardiovascular risks, and antithrombotic use) and focused neuro exam. Surveys show many clinicians interview well but still rely on outdated tests. [9]
Do not:
Rely on pre‑manipulative positional vertebrobasilar tests; contemporary peer‑reviewed analyses argue their poor diagnostic utility and recommend abandoning them. [13]
Rationale: The literature questions whether head/neck positioning meaningfully predicts vascular compromise; a negative test does not ensure safety, and false reassurance can be dangerous. [13]
Technique Selection:
Alternatives to HVLA Cervical Manipulation
- Cervical mobilization (Grades I–IV). In clinician surveys, mobilization is perceived as safer than manipulation. [9]
- Thoracic spine thrust manipulation. Improves neck pain/function without end‑range cervical rotation; systematic reviews and meta‑analyses support short‑term improvements in pain and disability. [10–12]
- Instrument‑assisted/low‑force cervical techniques and first‑rib mobilization, tailored to regional dysfunction – appropriate given this patient’s bilateral first‑rib restriction.
- Soft‑tissue/myofascial care, postural retraining, endurance/strength for cranio‑cervical and periscapular muscles, and ergonomics for deskwork and infant‑care demands.
Practical Chairside Checklist
Assess patients frequently for:
- Genetics/connective tissue: MTHFR status, EDS features, family history of aneurysm/CeAD. [1–3]
- Medications: Antiplatelets/anticoagulants; recent changes. [4–5]
- Recent infection/trauma/migraine: Especially with new, unfamiliar, moderate‑to‑severe neck pain or headache. [1–2,7–8,13]
- Red flags: 5D’s/3N’s, Horner’s, cranial nerve changes, progressive neuro findings – urgent referral. [13]
Choose techniques accordingly: Prefer mobilization, thoracic manipulation, and low‑force options before considering cervical HVLA in potentially high-risk patients. [9–12]
Communicate risks/benefits:
Serious events are rare, but consequences are high – use clear informed consent and align with patient preferences. [7–8,13]
Conclusion
Cervical spine care remains an effective and valuable component of chiropractic practice, but optimal patient outcomes depend on individualized risk assessment and evidence‑informed clinical decision‑making.
This case highlights how factors such as genetic variability (e.g., MTHFR mutations) and medication use (antiplatelet therapy) may signal underlying vascular vulnerability that is not apparent on routine orthopedic or neurologic examination.
While cervical arterial dissection and stroke are rare, their potential severity warrants a safety‑first approach that emphasizes thorough history taking, informed consent, and judicious technique selection.
By integrating current research, recognizing non-modifiable risk factors, and utilizing effective, lower-risk alternatives to HVLA cervical manipulation when appropriate, chiropractors can continue to deliver high-quality, patient-centered care while minimizing preventable risk.
Ultimately, clinical excellence in chiropractic is not defined by any single technique, but by the ability to adapt care to each patient’s unique presentation and risk profile.
References
- Jacobs W, Wright DS, Pohlman K, et al. Risk factors for cervical artery dissection: a systematic review and meta-analysis. Stroke Vasc Neurol. 2025;–. doi:10.1136/svn-2025-004186.
- Debette S, Markus HS. The genetics of cervical artery dissection: a systematic review. Stroke. 2009;40(6):e459-e466. doi:10.1161/strokeaha.108.534669.
- Kloss M, Wiest T, Hyrenbach S, et al. MTHFR 677TT genotype increases the risk for cervical artery dissections. J Neurol Neurosurg Psychiatry. 2006;77(8):951-952. doi:10.1136/jnnp.2006.089730.
- Kaufmann JE, Harshfield EL, Gensicke H, et al. Antithrombotic treatment for cervical artery dissection: a systematic review and individual patient data meta-analysis. JAMA Neurol. 2024;81(6):630-637. doi:10.1001/jamaneurol.2024.1141.
- Yaghi S, Shu L, Fletcher L, et al. Anticoagulation versus antiplatelets in spontaneous cervical artery dissection: a systematic review and meta-analysis. Stroke. 2025;–. doi:10.1161/STROKEAHA.124.047310.
- Markus HS, Levi C, King A, et al.; CADISS Investigators. Antiplatelet therapy vs anticoagulation in cervical artery dissection: final results of CADISS. J Vasc Surg. 2019;70(6):2098-2099. doi:10.1016/j.jvs.2019.09.035.
- Haynes MJ, Vincent K, Fischhoff C, Bremner AP, Lanlo O, Hankey GJ. Assessing the risk of stroke from neck manipulation: a systematic review. Int J Clin Pract. 2012;66(10):940-947. doi:10.1111/j.1742-1241.2012.03004.x.
- Rothwell DM, Bondy SJ, Williams JI. Chiropractic manipulation and stroke: a population-based case-control study. Stroke. 2001;32(5):1054-1060. doi:10.1161/01.STR.32.5.1054.
- Hutting N, Mourad F, Taylor A, et al. Pre-treatment risk factor assessment and safe management of the cervical spine: a survey among physical therapists. Musculoskelet Sci Pract. 2026;–. doi:10.1016/j.msksp.2026.103542.
- Masaracchio M, Kirker K, States R, Hanney WJ, Liu X, Kolber MJ. Thoracic spine manipulation for mechanical neck pain: systematic review and meta-analysis. PLoS One. 2019;14(2):e0211877. doi:10.1371/journal.pone.0211877.
- Cross KM, Kuenze C, Grindstaff T, Hertel J. Thoracic spine thrust manipulation improves pain, ROM, and function in mechanical neck pain: systematic review. J Orthop Sports Phys Ther. 2011;41(9):633-642. doi:10.2519/jospt.2011.3670.
- Masaracchio M, Kirker K, Dewan B, Caronia S. Effectiveness of thoracic spine manipulation for neck pain: umbrella review with risk of bias assessment. Healthcare (Basel). 2026;14(2):240. doi:10.3390/healthcare14020240.
- Hutting N, Kranenburg RA, Kerry R. Yes, we should abandon pre-treatment positional testing of the cervical spine. Musculoskelet Sci Pract. 2020;49:102181. doi:10.1016/j.msksp.2020.102181.
- Haldeman S, Carey P, Townsend M, Papadopoulos C. Arterial dissections following cervical manipulation: the chiropractic experience. CMAJ. 2001;165(7):905-906.
- Abidoye O, Ogbuagu H, Al-Rubaye R. Carotid artery dissection following cervical spine manipulation: association or causation? Chest. 2022;161(6 Suppl):A76.”
Stay updated on all scientific advances with Hemostasis Today.
-
May 13, 2026, 15:07Tung Nguyen Thanh: New Perspective on Thrombosis in Hematological Malignancies in Vietnam
-
May 13, 2026, 15:03Haji Siyamuddin Ansari: The Key Difference Between Plasma and Serum
-
May 13, 2026, 14:45Masoabi Sefojane: The Cost of a 35-Year Diagnosis Delay
-
May 13, 2026, 14:39Ahmed Mohsen: Managing DVT During Pregnancy and Lactation
-
May 13, 2026, 14:38The Coffee Shop Origins of Factor V Leiden – ISTH
-
May 13, 2026, 14:33Moustafa Abdou: Could a Commonly Prescribed Drug Trigger Life-Threatening Hemolysis?
-
May 13, 2026, 14:04Lester Leung: The Lancet Highlights TAPIS Trial at ESOC 2026
-
May 13, 2026, 13:15Priyanka Kasatkar: How One Research Idea Became a Diagnostic Innovation in Hemostasis
-
May 13, 2026, 13:09Ram Mohan Jaiswal։ Celebrating International Nurses Day with Voluntary Blood Donation

