
Abdul Mannan: When Blood Clots Show Up in Unexpected Places
Abdul Mannan, Consultant Haematologist at Betsi Cadwaladr University Health Board, shared a post on LinkedIn:
“When Blood Clots Show Up in Unexpected Places
Most doctors think DVT and PE when they hear ‘blood clot.’
But as a Thrombosis Lead, I spend a lot of time managing clots that don’t follow the textbook. The ones that form in the brain. In the liver veins. In the portal system.
These are the cases that keep haematologists busy — and they demand a completely different mindset.
Let’s talk about two locations that matter:
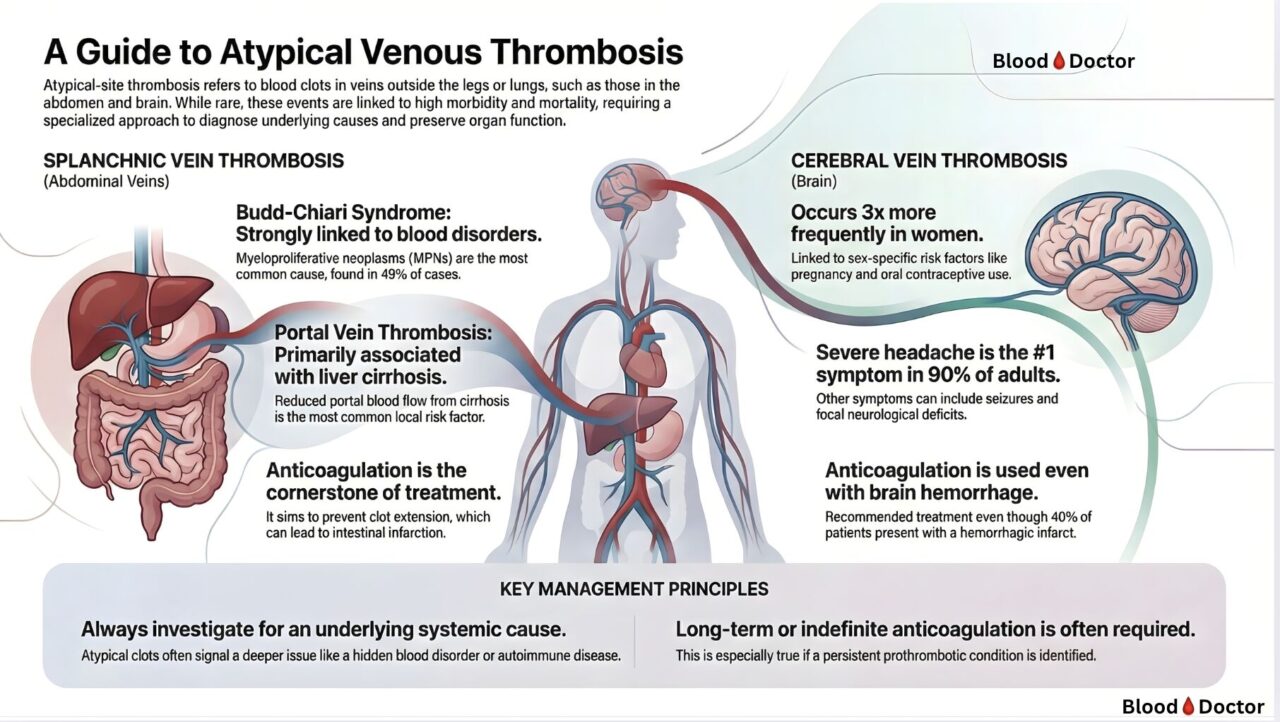
Splanchnic Vein Thrombosis (Abdomen)
When I see Budd-Chiari syndrome, my first question isn’t “why did this clot form?”
It’s “which myeloproliferative neoplasm am I going to find?”
Because MPNs account for nearly half of all cases. That’s 49%. And here’s the thing — sometimes the clot appears before any other sign of the blood cancer. The thrombosis IS the presentation.
Portal vein thrombosis tells a different story. Liver cirrhosis dominates here. Sluggish flow. Damaged vessels. The perfect storm for clot formation.
In both scenarios, anticoagulation remains the treatment backbone — even when it feels counterintuitive. Without it, clot extension leads to intestinal infarction. And that’s a disaster.
Cerebral Vein Thrombosis (Brain)
Three times more common in women. Pregnancy. Oral contraceptives. The hormonal connection is undeniable.
90% present with severe headache. Not a mild one — the kind that brings patients to A&E thinking the worst.
Now here’s what surprises many colleagues:
We anticoagulate even when there’s hemorrhage on imaging.
Yes, you read that right. About 40% of CVT patients have hemorrhagic transformation at diagnosis. We still anticoagulate. The evidence supports it. The clot needs treatment, and the bleeding is usually a consequence of venous congestion, not arterial rupture.
Two principles I live by:
1. Always hunt for the underlying cause. Atypical clots are often the tip of the iceberg. MPNs. Paroxysmal nocturnal haemoglobinuria. Antiphospholipid syndrome. Behçet’s disease. Don’t stop until you’ve looked.
2. Think long-term. These aren’t your standard three-month anticoagulation cases. When we find a persistent prothrombotic condition, indefinite treatment becomes the conversation.
Atypical site thrombosis is rare. But when it happens, getting it right changes lives.
Have you encountered challenging atypical thrombosis cases? What was the underlying diagnosis?”
Find more posts featuring Abdul Mannan on Hemostasis Today.
-
Apr 30, 2026, 15:38Ahvie Herskowitz: Is It Iron or ‘Oxidized Rust’? – A New Predictor of Aging.
-
Apr 30, 2026, 15:01Neil Morgan: New Collaborative Research Review on Large‐Scale Genetic Analysis in the Bleeding Disorders Community
-
Apr 30, 2026, 14:52Neema Ngugi: Understanding the D-Dimer Test – A Key Tool in Detecting Blood Clots
-
Apr 30, 2026, 14:33Abdul Mannan: The Clinical Pattern That Should Make You Think of VEXAS
-
Apr 30, 2026, 14:28Jennifer Le Mac: How the Immune System Shapes Venous Thrombosis
-
Apr 30, 2026, 14:22Samantha Xavier: Successfully Defended My PhD Thesis on P-Selectin as a Biomarker for Venous Thromboembolism
-
Apr 30, 2026, 14:09Robert Lufkin: Anti-Amyloid Drugs Fail Alzheimer’s Patients
-
Apr 30, 2026, 13:54Matthew D. Neal: A Major Step Forward in Trauma and Resuscitation Science
-
Apr 30, 2026, 13:35Day 2 of the EHC Youth Leadership Workshop 2026

