
Abdul Mannan: A Red Eye, a Blood Clot, and Ibrutinib – The Clinical Tightrope
Abdul Mannan, Consultant Hematologist at Betsi Cadwaladr University Health Board, shared a post on LinkedIn:
“A red eye. A blood clot. And ibrutinib. This is the clinical tightrope.
My SLL patient was on ibrutinib 420 mg for her disease and therapeutic anticoagulation for a massive PE.
Then her eye turned red. Spontaneous subconjunctival haemorrhage. No major bleeding anywhere.
The question every haematologist dreads: Do I stop something? And if so, what?
Here is the answer the evidence gives us.
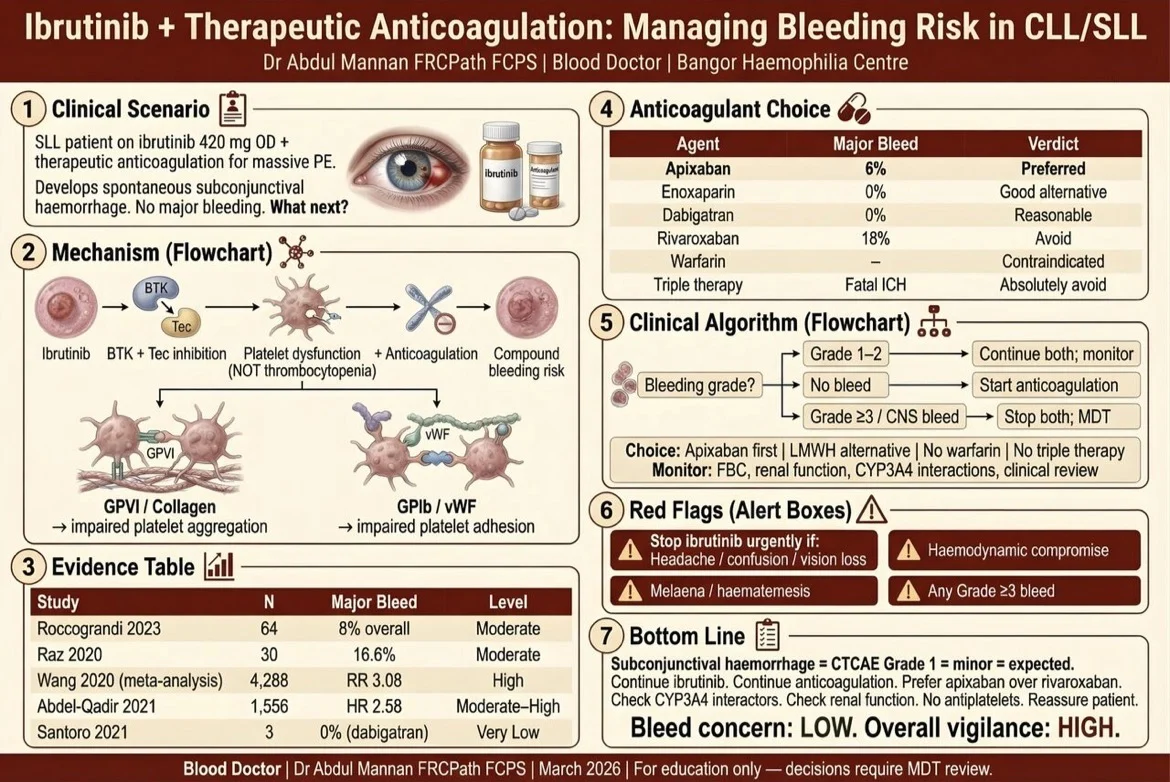
The red eye is Grade 1. It is minor. It is expected. Ibrutinib knocks out BTK and Tec kinase together, crippling platelet adhesion via GPVI/collagen and GPIb/vWF pathways.
The result is platelet dysfunction, not thrombocytopenia. Mucocutaneous bleeding happens in up to 67% of patients on ibrutinib. A subconjunctival bleed is part of that story.
But stacking anticoagulation on top? That is where the real risk lives.
What the numbers tell us (Roccograndi et al., Leukemia & Lymphoma 2023, n=64 CLL/SLL patients):
- Apixaban used with ibrutinib: 6% major bleeding
- Rivaroxaban used with ibrutinib: 18% major bleeding
- Enoxaparin used with ibrutinib: 0% (small numbers, but reassuring)
Warfarin: contraindicated, full stop
Ibrutinib combined with DOAC and clopidogrel:
one fatal intracranial haemorrhage
Wang et al. meta-analysis (Frontiers in Pharmacology 2020, 11 RCTs, 4,288 patients) showed ibrutinib triples overall bleeding risk in CLL patients.
So what did I do?
Continued ibrutinib. Continued anticoagulation. The PE does not forgive you for stopping. Checked she was on apixaban not rivaroxaban. Checked renal function. Removed every antiplatelet from her list. Educated her on CNS and GI red flag symptoms.
The infographic below tells the whole story in one page. Save it. Share it with your trainees.
- Bleed concern: LOW.
- Overall vigilance: HIGH.
Have you faced this combination in practice? What anticoagulant did you go with?”
Other posts featuring Abdul Mannan on Hemostasis Today.
-
Apr 23, 2026, 12:18Mona Ranade: A Contemporary Framework for Managing Right Heart Thrombus in PE
-
Apr 23, 2026, 11:59Strengthening Hemophilia Care Through Collaboration and Commitment in India at IHC X 2026 – Hemophilia Federation India
-
Apr 23, 2026, 08:16David Ferreira: Identifying the True Drivers of Recurrent Thrombosis
-
Apr 23, 2026, 08:05Hugo Antonio Romo Rubio: Biology, Function, and Updated Classification of von Willebrand Disease
-
Apr 23, 2026, 07:50Hassan Raza: A Smarter Risk Prediction in MPNs Using AI
-
Apr 23, 2026, 05:32Why TXA and rFVIIa Are Not Equivalent in Trauma Bleeding Control – RPTH Journal
-
Apr 23, 2026, 04:08Suraj Mali: Pune Team Initiative for World Hemophilia Day 2026 Advances Early Diagnosis in Hemophilia
-
Apr 23, 2026, 03:58Adam Ho: What Does It Actually Mean to ”Prevent” a Stroke?
-
Apr 23, 2026, 03:49Jakob Krebs Christensen: Mobile Stroke Units Bring Imaging and Treatment Directly to the Patient

