
Ney Carter Borges: Triple Low-Dose Antihypertensive Therapy After Intracerebral Hemorrhage – A Pragmatic and Effective Strategy
Ney Carter Borges, Member Cardiologist of Global Physician Association at Cleveland Clinic Florida, shared a post on LinkedIn:
“Triple Low-Dose Antihypertensive Therapy After Intracerebral Hemorrhage: A Pragmatic and Effective Strategy
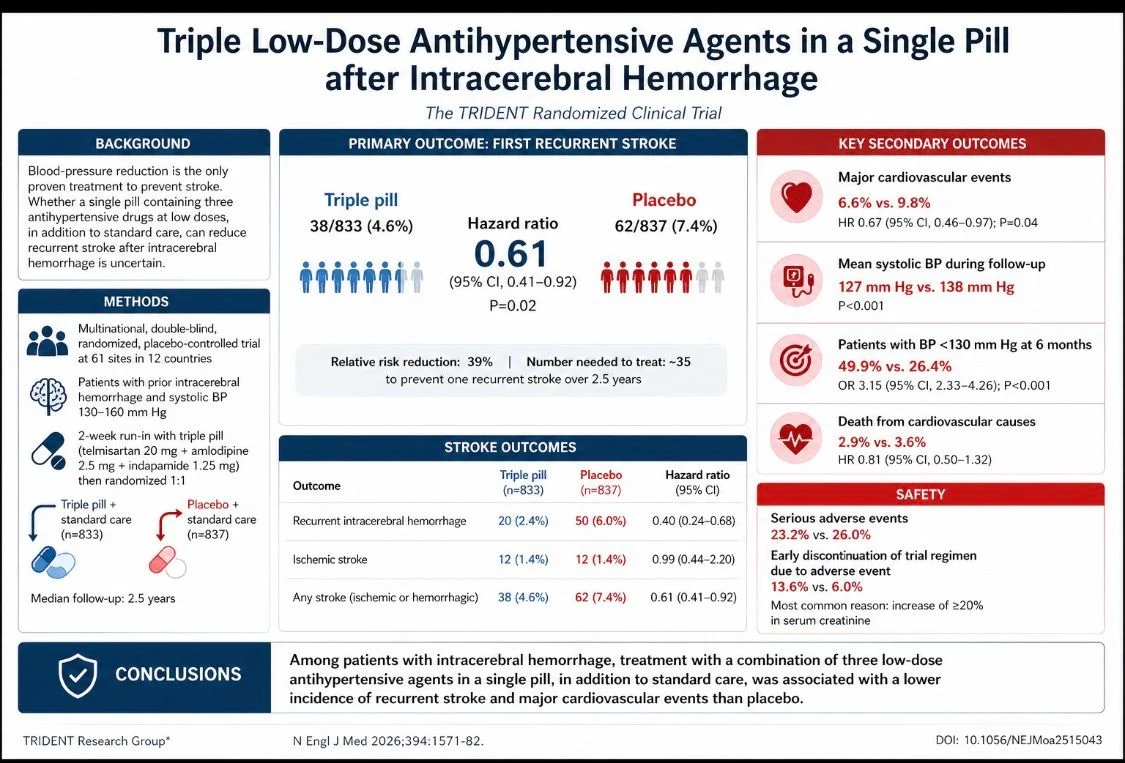
This multicenter, randomized, double-blind, placebo-controlled trial (TRIDENT) evaluated whether a fixed-dose combination of three low-dose antihypertensive agents could improve outcomes in patients with prior intracerebral hemorrhage (ICH). The study enrolled 1,670 patients with baseline systolic blood pressure between 130–160 mmHg, randomized to receive either a once-daily triple pill (telmisartan 20 mg, amlodipine 2.5 mg, indapamide 1.25 mg) or placebo, in addition to standard care.
Over a median follow-up of 2.5 years, the intervention demonstrated a clinically meaningful reduction in recurrent stroke.
The primary endpoint occurred in 4.6% of the triple-pill group versus 7.4% in the placebo group (hazard ratio [HR] 0.61; 95% CI 0.41–0.92; P=0.02), corresponding to a relative risk reduction of approximately 39%. This benefit was primarily driven by a substantial decrease in recurrent intracerebral hemorrhage (HR 0.40).
Importantly, the triple therapy achieved superior blood pressure control, with a mean systolic blood pressure of 127 mmHg vs. 138 mmHg in the placebo group, and significantly higher rates of target BP attainment (<130 mmHg) at 6 months (49.9% vs. 26.4%; OR 3.15; P<0.001).
In addition to stroke prevention, the intervention reduced major cardiovascular events (6.6% vs. 9.8%; HR 0.67; P:0.04), although no statistically significant reduction in cardiovascular mortality was observed.
Safety outcomes were broadly comparable between groups, though treatment discontinuation was more frequent in the triple-pill arm (13.6% vs. 6.0%), largely driven by increases in serum creatinine.
From a clinical perspective, the findings support a simplified, fixed-dose combination strategy to enhance adherence and intensify blood pressure control—two critical gaps in post-ICH management. The estimated number needed to treat (NNT) of ~35 underscores meaningful real-world applicability.
In summary, this study provides robust evidence that early initiation of low-dose combination antihypertensive therapy in a single pill significantly reduces recurrent stroke and improves blood pressure control after intracerebral hemorrhage, reinforcing aggressive BP management as the cornerstone of secondary prevention in this high-risk population.”
Find more posts featuring Ney Carter Borges on Hemostasis Today.
-
Apr 27, 2026, 23:24Leonardo Roever: The Emerging Role of the TyHGB Index in Predicting New-Onset Stroke
-
Apr 27, 2026, 20:25Shek Sady Khan: Addressing the Silent Burden of Venous Thromboembolism in Bangladesh
-
Apr 27, 2026, 16:04Heghine Khachatryan: Intracranial Hemorrhage in Leukemia – Beyond Thrombocytopenia
-
Apr 27, 2026, 15:56Marc Carrier: Supporting Thrombosis Canada in My Final Year as President
-
Apr 27, 2026, 15:52Tagreed Alkaltham։ You Think Eligibility Is About You… It’s Not
-
Apr 27, 2026, 15:52Emma Gasson: Top Abstract Oral Presentation at BSH 2026 on Cancer-Associated Thrombosis Microfluidics
-
Apr 27, 2026, 15:48Elliot Tapper: Continuing Anticoagulation Improves PVT Outcomes During Banding
-
Apr 27, 2026, 15:44Crisanto Torres: Early Plasma Administration Maximizes Survival in Traumatic Intracranial Hemorrhage
-
Apr 27, 2026, 15:38Key Insights from ESHMPN 26 on Advances in MPN Management – ESH

