
Reza Shojaei: Germany’s Plasma Collection – History, Scale, and Strategic Fault Lines
Reza Shojaei, Chief Operating Officer at Canadian Plasma Resources, shared a post on Linkedln:
”Europe says: ‘donate.’
Others say: ‘compensate.
Germany does both.
Germany has quietly built one of the most scalable plasma collection models in Europe, balancing regulation, private-sector capacity, and donor engagement.
But here’s the real question:
Is this the model the rest of the world will ultimately be forced to adopt?
In this edition of Blood and Plasma Pulse, we break down:
- How Germany built its system
- Why Europe still depends on imported plasma
- What this means for countries aiming for self-sufficiency
Plus: a concise Germany vs EU vs US comparison
Germany has evolved into one of Europe’s most consequential plasma ecosystems, combining high-volume plasmapheresis, permitted donor expense compensation, and major domestic fractionation capacity.
In 2024, Germany reported collecting 3.59 million litres of plasma for fractionation, alongside very large cross-border flows (6.24 million litres imported; 5.03 million litres exported, including intra-EEA transport) (Paul-Ehrlich-Institut, 2025).
This scale sits against a backdrop of demand, with immunoglobulin (Ig) volumes placed on the market in Germany rising by ~87% from 2015 to 2024 (Paul-Ehrlich-Institut, 2025).
In fact, Germany has emerged as one of the most influential plasma collection markets outside the United States, yet its evolution is often underexamined.
Its hybrid model, combining public infrastructure with regulated private sector participation, offers critical lessons for global self-sufficiency strategies.
Historical Evolution
Germany’s plasma collection system traces back to the post-World War II era, when transfusion medicine was primarily hospital-based and publicly administered.
By the 1970s and 1980s, technological advancements in plasmapheresis enabled large-scale plasma collection, gradually shifting the model toward specialized centers (Burnouf, 2007).
A pivotal transformation occurred in the 1990s following contamination crises (e.g., HIV and hepatitis transmission), which triggered sweeping regulatory reforms and modernization of blood safety systems across Europe, including Germany (Kreil, 2015). These reforms laid the groundwork for today’s highly controlled environment.
From the early 2000s onward, Germany began expanding private-sector participation, allowing companies such as Grifols, CSL Plasma, and Octapharma to establish and operate plasma collection centers.
This hybrid model significantly increased collection capacity while maintaining public oversight.
Current Regulatory Framework
Germany’s plasma governance sits at the intersection of national law and guidance and European harmonization.
The TFG provides the legal backbone; technical and clinical guardrails are reinforced by national hemotherapy guidelines developed by the German Medical Association in agreement with the Paul-Ehrlich-Institut, with expert consultation roles assigned to the Arbeitskreis Blut at the Robert Koch Institute (Seitz and Heiden, 2010).
At the European level, Directive 2002/98/EC established quality and safety standards and explicitly promotes voluntary, unpaid donation as a means of ensuring high safety standards (without constituting a categorical ban on compensation).
Looking ahead, the European Union adopted the SoHO Regulation (EU) 2024/1938, repealing the older blood directive framework and introducing a directly applicable regulation following a transition period (widely cited as applying from 2027) (European Parliament and Council of the European Union, 2024).

Every unit of plasma undergoes rigorous processing and verification to ensure safety, traceability, and therapeutic reliability.
Supply vs Demand Reality
Germany’s plasma system is best understood as two coupled engines: collection (donor-facing) and fractionation/PDMP manufacturing (industrial conversion), connected by significant cross-border logistics.
In 2024, Germany reported 3,593,828 litres of plasma collected for fractionation, up by 56,245 litres year over year; 74% (2,642,281 litres) came from plasmapheresis rather than recovered plasma from whole blood.
In 2023, Germany’s collected fractionation plasma accounted for over 38% of the total volume reported across Council of Europe member states, a strong indicator of Germany’s outsized role in Europe (the EU-only share is not explicitly stated in the PEI report and is therefore unspecified) (Paul-Ehrlich-Institut, 2025).
Germany is also a logistics and processing hub, not a closed national loop.
In 2024, plasma for fractionation flows were reported as 6,239,275 litres imported and 5,030,901 litres exported (figures include intra-EEA transport), implying a net import of ~1.21 million litres.
In the same year, Germany reported 5,774,036 litres fractionated (vs 4,802,202 litres available), suggesting substantial processing throughput and inventory dynamics.
Demand pressures are evident in immunoglobulin utilization: the quantity of normal Ig placed on the market rose from 7,720 kg (2015) to 14,407 kg (2024), an 87% increase, and 2024 use (14,653 kg) slightly exceeded the placed-on-market quantity (Paul-Ehrlich-Institut, 2025).
Major PDMP manufacturers/fractionators operating in Germany include:
CSL Behring: opened the ‘Phoenix’ base fractionation facility in Marburg with an investment reported at US$470M and claims of significantly expanded/automated fractionation capability (CSL Behring, 2023).
Biotest: reports manufacturing facilities in Dreieich, with stated plasma processing capacity ramping ‘up to 3 million litres’ by 2026 (Biotest AG, n.d.).
Octapharma: lists manufacturing sites in Germany (e.g., Dessau-Rosslau), supporting the broader PDMP manufacturing footprint (site-specific fractionation roles are not fully detailed in this source and are therefore unspecified) (Octapharma AG, n.d.).
Donor compensation policy (Germany): Germany permits compensation framed as an expense allowance.
Historical and policy documentation emphasize keeping compensation from becoming wage-like: a 1993 expert vote supports generally unpaid donation but allows expense compensation (then capped in Deutsche Mark terms) with guardrails to avoid ‘payment character’ (Arbeitskreis Blut, 1993).
A later European Commission implementation report notes that German law allows an expense allowance and cites an expert resolution stating there is no proven safety detriment; it also references a €25 ceiling for the whole-blood expense allowance and describes policy sensitivities around advertising payments (European Commission, 2006).
A practical contemporary summary of Section 10 TFG describes compensated plasmapheresis in the private sector (e.g., ‘up to 25 euros or gifts’) and donation frequency allowances (e.g., up to 60 times/year with minimum day gaps), but granular national enforcement details are unspecified in public PEI supply tables (Pant et al., 2021).
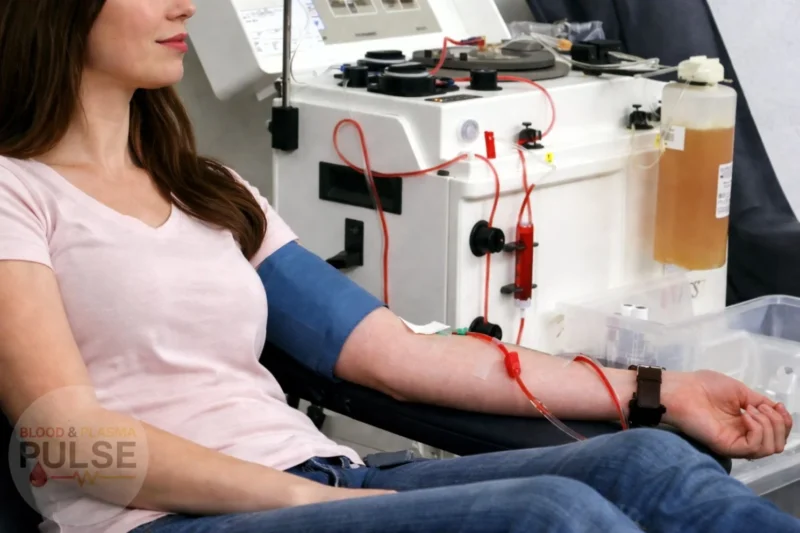
Modern plasmapheresis in action: wehere donor exprience, technology, and effeciency converge to sustain a growing global demand for life-saving therapies.
Donor demographics (Germany): National surveillance publications indicate plasma donor participation is comparatively small but intensive.
In 2006, around 0.3% of eligible Germans donated plasma/platelets repeatedly; repeat plasma donors were younger than repeat whole-blood donors, with an average plasmapheresis donation frequency of around 11.9/year (and higher for some segments) (Ritter et al., 2008).
Updated surveillance for 2010 reported 0.4% repeatedly donating plasma/platelets and an average plasmapheresis frequency of ~12.5/year (Ritter et al., 2012).
More recent, nationally aggregated socio-economic donor profiling for plasmapheresis (e.g., income/occupation mix) is unspecified in the official sources above.
Germany vs EU vs US Snapshot
Donor Compensation (Source Plasma)
- Germany: Permitted as an expense allowance; compensation is common in private plasmapheresis centers
- EU / Europe: Policy preference for voluntary, unpaid donation; practices vary by country; ongoing push to strengthen non-remunerated capacity
- United States: Compensation widely practiced in private-sector plasma collection; regulated donation frequency limits
Share of Global Source Plasma (Illustrative)
- Germany: ~5% of global supply (indicative estimate based on non-aligned data points)
- EU / Europe: ~14% of global supply (pre-pandemic estimate)
- United States: ~65–70% of global supply; dominant exporter
Plasma Self-Sufficiency (Medicinal Production)
- Germany: No single official self-sufficiency ratio; major collector and a key import/export hub within Europe
- EU / Europe: ~40% to ~60% self-sufficient; structurally dependent on imports
- United States: Effectively self-sufficient and a net exporter supporting global supply
Key Controversies
Germany’s controversies cluster into three recurring themes: trust, ethics, and donor protection.
Trust: The early-1990s contaminated blood-product scandals triggered intense scrutiny and long-term reputational damage, widely cited as catalysts for stronger governance (Abbott, 1993)
Ethics of compensation: Germany’s allowance model has been repeatedly framed as ‘expense reimbursement’ rather than payment, with explicit caution that high-frequency plasma donation should not turn compensation into wage-like income (Arbeitskreis Blut, 1993).
This sits awkwardly beside Europe’s normative preference for voluntary, unpaid donation and today’s strategic autonomy goals under the SoHO framework (European Parliament and Council of the European Union, 2003).
Donor protection and safety modernization: Germany’s screening regimes are frequently described as highly mature, with ongoing reassessment of burdensome legacy safeguards.
For example, a large PEI-initiated survey on quarantine plasma release (2015–2019) found extremely low theoretical residual risk under current screening, supporting debate about shortening or discontinuing quarantine storage without measurably reducing safety (Fiedler et al., 2022).
At the same time, Europe-wide initiatives explicitly call for stronger evidence on the health effects of frequent plasmapheresis, highlighting that donor protection is now a strategic supply lever, not only an ethical imperative (Supply Project, n.d.).

From donation to life-saving therapy, plasma collection remains the critical first step in a global healthcare value chain that millions of patients depends on every day.
Global Implications
A German-level view quickly becomes a global story.
The OECD describes PDMP supply chains as vulnerable and notes that global source plasma is dominated by the United States, with 67% of pre-pandemic source plasma, versus 14% from Europe.
Within Europe, the OECD reports that most source plasma comes from a small set of countries, including Germany (Organization for Economic Co-operation and Development, 2024).
This concentration means Germany’s regulatory choices, compensation framing, donor-frequency constraints, and data transparency carry spillovers: Europe’s resilience efforts (e.g., EU4Health-funded work to strengthen voluntary data collection) will succeed or fail in part depending on whether high-volume countries can scale while preserving donor trust (SUPPLY Project, n.d.).
Last Words
Germany’s plasma system is already critical infrastructure.
The opportunity now is to convert scale into strategic resilience, without triggering ethical backlash or donor attrition.
- First, treat donor protection as a measurable, publishable performance domain: align German practice with the emerging European agenda calling for large-scale prospective evidence on frequent donation (including IgG-related metrics and donor outcomes).
- Second, elevate transparency on “self-sufficiency” beyond national pride metrics. Germany’s 2024 data show a sophisticated hub model with large import/export flows; publishing a clear, decision-grade narrative on what Germany aims to be self-sufficient in (plasma litres, fractionation capacity, IVIG access, or critical indications) would improve policy credibility.
- Third, anticipate SoHO implementation friction: the shift to Regulation (EU) 2024/1938 presents an opportunity to harmonize donor vigilance, data interoperability, and shortage planning, areas repeatedly highlighted in European initiatives.
Finally, demand discipline must sit alongside supply growth.
Germany’s sharp increase in Ig use over the last decade underscores the need for evidence-based utilization governance (national registries, indication stewardship, and shortage protocols), so that incremental litres translate into patient outcomes, not just higher baseline consumption.
References
- Abbott, A. (1993). Concern grows over impact of German blood scandal. Nature, 366(6451), 98.
- Arbeitskreis Blut. (1993, December 1). Aufwandsentschädigung für Blut- und Plasmaspender [Report].
- Biotest AG. (n.d.). Biotest at a glance.
- Burnouf, T. (2007). Modern plasma fractionation. Transfusion Medicine Reviews, 21(2), 101–117.
- CSL Behring. (2023, March 23). “Phoenix” is delivering on our promise: The new base fractionation in Marburg starts regular operation with a ceremonial opening.
- European Commission. (2006). Report from the Commission to the Council and the European Parliament on the promotion by Member States of voluntary unpaid blood donations (COM(2006) 217 final).
- European Parliament and Council of the European Union. (2003, January 27). Directive 2002/98/EC setting standards of quality and safety for the collection, testing, processing, storage and distribution of human blood and blood components and amending Directive 2001/83/EC.
- European Parliament and Council of the European Union. (2024, June 13). Regulation (EU) 2024/1938 on standards of quality and safety for substances of human origin intended for human application and repealing Directives 2002/98/EC and 2004/23/EC.
- Fiedler, S. A., Oberle, D., Henseler, O., Heiden, M., and Funk, M. B. (2022). Follow-up of plasma donors after quarantine storage: Results of a 5-year survey in Germany. Transfusion Medicine and Hemotherapy, 50(1), 26–29.
- Octapharma AG. (n.d.). Our locations.
- Organization for Economic Co-operation and Development. (2024). Securing medical supply chains in a post-pandemic world. OECD Publishing.
- Pant, S., Bagha, R., and McGill, S. (2021, December). International plasma collection practices: Project report (CADTH Health Technology Review) [Internet]. Canadian Agency for Drugs and Technologies in Health.
- Paul-Ehrlich-Institut. (2025). Report on the supply of blood and blood products 2024 (pursuant to Section 21 TFG).
- Ritter, S., Willand, L., Reinhard, B., et al. (2008). Demography and donation frequencies of blood and plasma donor populations in Germany. Bundesgesundheitsblatt – Gesundheitsforschung – Gesundheitsschutz, 51, 915–925.
- Ritter, S., Hamouda, O., and Offergeld, R. (2012). Demography and donation frequencies of blood and plasma donor populations in Germany: Update 2010 and 5-year comparison. Bundesgesundheitsblatt – Gesundheitsforschung – Gesundheitsschutz, 55(8), 914–922.
- Seitz R, Heiden M. Quality and Safety in Blood Supply in 2010. Transfus Med Hemother. 2010 Jun;37(3):112-117. doi: 10.1159/000314497. Epub 2010 May 20. PMID: 20577599; PMCID: PMC2889628.
- SUPPLY Project. (n.d.). Strengthening voluntary non-remunerated plasma collection capacity in Europe.”
Stay updated with Hemostasis Today.
-
May 7, 2026, 17:31Talha Badar: New Classical Hematology Chapter on Bleeding and Thrombosis
-
May 7, 2026, 17:26Maria Τektonidou: Gene Network Analysis Identifies STAT1 in Thrombotic APS
-
May 7, 2026, 17:23Sonu Bhaskar: Inflammatory Biomarkers in Acute Cerebral Venous Sinus Thrombosis
-
May 7, 2026, 16:53Patricio S. Espinosa: Anticoagulation Is Not an Absolute Contraindication to Amyloid Therapy
-
May 7, 2026, 16:34Arun V J: Give Blood and Be the Hero You Always Wanted to Be
-
May 7, 2026, 16:15August Bones: When Would You Consider Placing an Inferior Vena Cava Filter After a Pulmonary Embolism?
-
May 7, 2026, 15:58Stop Asking Doctors to Do More – Reimagining the Care Team – The US Oncology
-
May 7, 2026, 15:42Chokri Ben Lamine: CVC-Associated UE-DVT and Catheter Removal
-
May 7, 2026, 15:38Samwel Mikaye: Key Insights on Vitamin B12 Deficiency

