
Simon Senanu: Rouleaux Formation – When Red Cells Stack Like Coins
Simon Senanu, Medical Laboratory Scientist at Perkins Medical Centre, shared a post on LinkedIn:
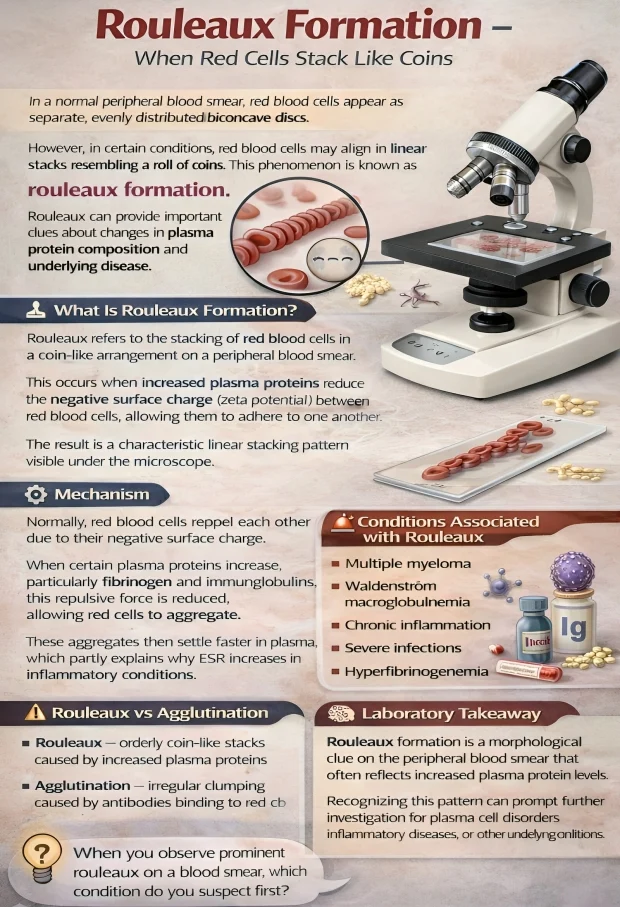
”Rouleaux Formation – When Red Cells Stack Like Coins
In a normal peripheral blood smear, red blood cells appear as separate, evenly distributed biconcave discs.
However, in certain conditions, red blood cells may align in linear stacks resembling a roll of coins. This phenomenon is known as rouleaux formation.
Rouleaux can provide important clues about changes in plasma protein composition and underlying disease.
What Is Rouleaux Formation?
Rouleaux refers to the stacking of red blood cells in a coin-like arrangement on a peripheral blood smear.
This occurs when increased plasma proteins reduce the negative surface charge (zeta potential) between red blood cells, allowing them to adhere to one another.
The result is a characteristic linear stacking pattern visible under the microscope.
Mechanism
- Normally, red blood cells repel each other due to their negative surface charge.
- When certain plasma proteins increase, particularly fibrinogen and immunoglobulins, this repulsive force is reduced, allowing red cells to aggregate.
- These aggregates then settle faster in plasma, which partly explains why ESR increases in inflammatory conditions.
Conditions Associated with Rouleaux
Rouleaux formation may be seen in several clinical conditions, including:
- Multiple myeloma
- Waldenström macroglobulinemia
- Chronic inflammation
- Severe infections
- Hyperfibrinogenemia
These conditions often involve elevated plasma proteins, which promote red cell aggregation.
Rouleaux vs Agglutination
It is important to distinguish rouleaux from red cell agglutination.
- Rouleaux – orderly coin-like stacks caused by increased plasma proteins
- Agglutination – irregular clumping caused by antibodies binding to red blood cells
Agglutination is typically associated with immune-mediated processes, such as cold agglutinin disease.
Laboratory Takeaway
Rouleaux formation is a morphological clue on the peripheral blood smear that often reflects increased plasma protein levels.
Recognizing this pattern can prompt further investigation for plasma cell disorders, inflammatory diseases, or other underlying conditions.”
Other posts featuring Simon Senanu on Hemostasis Today.
-
Apr 22, 2026, 06:01Kathaleen Schnur: Global Perspectives on Psychosocial Support in Hemophilia Care
-
Apr 22, 2026, 05:43Maia Meier: A Journey to Raise Awareness for Women with Bleeding Disorders
-
Apr 22, 2026, 05:41Moustafa Abdou: Diagnostic Challenges in Pediatric Hematology
-
Apr 22, 2026, 04:43Ifeanyichukwu Ifechidere: The Critical Role of Calibrator Specificity in Anticoagulation Monitoring
-
Apr 22, 2026, 04:13Ilenia Calcaterra: Clinical Relevance of Persistent Pain in Emicizumab-Treated Haemophilia A
-
Apr 22, 2026, 03:56Annette Bowyer: Reflecting on Progress and Leadership in Laboratory Sciences
-
Apr 21, 2026, 21:07Tareq Abadl: Not Every Low Platelet Count Is True – Check the Smear First
-
Apr 21, 2026, 21:05Beverley Hunt: Honored to Receive the Lifetime Achievement Award at BSH 2026
-
Apr 21, 2026, 21:03Toong Youttananukorn: Proud to Support Data That Drives Action at WFH 2026

