
Timothy Lesaca: How SSRIs Influence Hemostasis Through Platelets
Timothy Lesaca, Child And Adolescent Psychiatrist at Transformations Care Network, shared a post on LinkedIn:
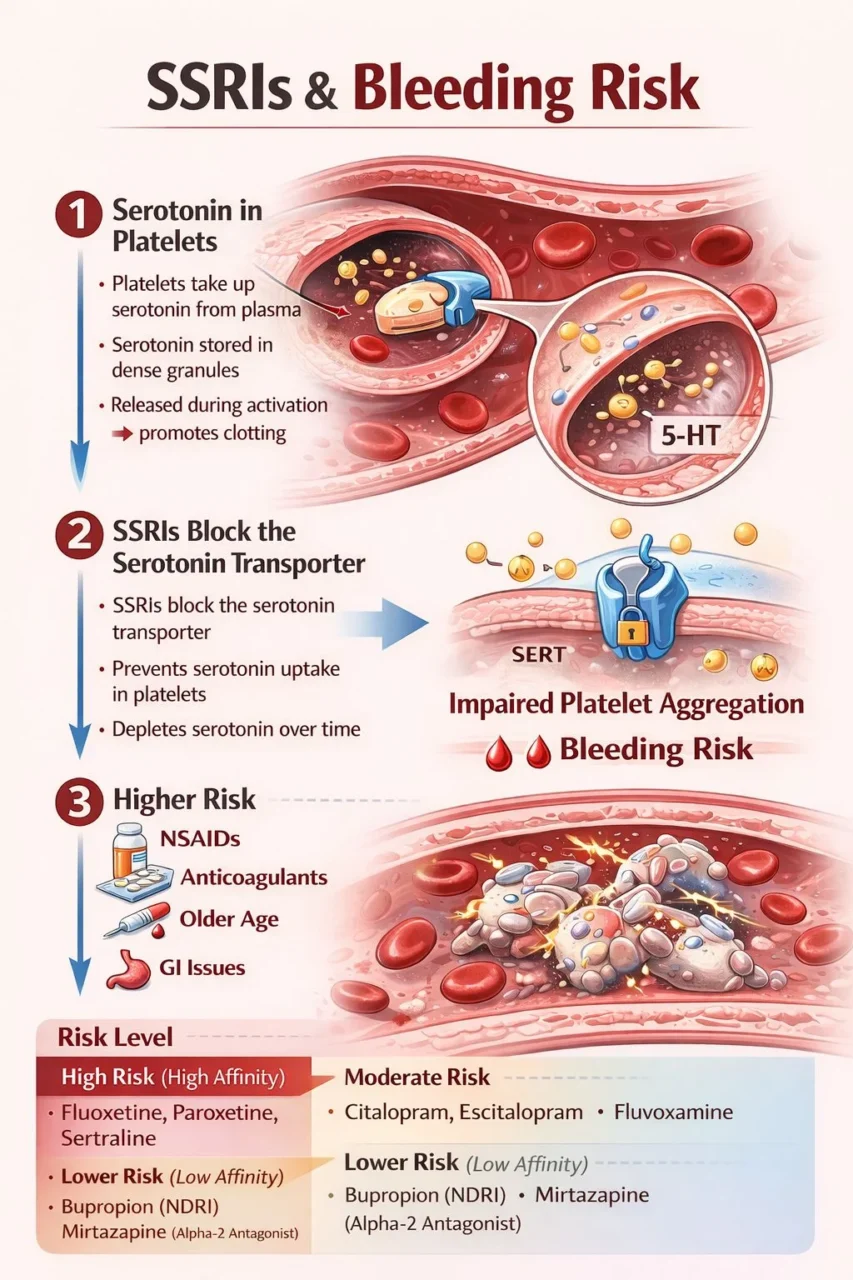
“SSRIs and Bleeding Risk
Selective serotonin reuptake inhibitors’ association with increased bleeding risk reflects an important pharmacological principle: drugs targeting neurotransmitter systems often exert clinically significant effects outside the central nervous system.
This effect is mediated through platelets.
Unlike neurons, platelets lack the ability to synthesize serotonin.
Instead, they depend on uptake from plasma via the serotonin transporter (SERT), the same target inhibited by SSRIs.
Under normal conditions, serotonin is stored in platelet dense granules and released during activation, where it amplifies aggregation and promotes vasoconstriction at sites of vascular injury.
This contributes to primary hemostasis.
SSRIs inhibit SERT on platelets, preventing serotonin uptake.
Over time, this leads to depletion of intraplatelet serotonin stores.
The result is impaired platelet aggregation, particularly in response to weak agonists, and reduced amplification of the hemostatic response.
Importantly, this does not abolish clotting.
Rather, it reduces the efficiency and stability of platelet plug formation.
Clinically, this manifests as an increased tendency toward mucosal and superficial bleeding.
The most consistently observed association is with upper gastrointestinal bleeding.
Several large observational studies and meta-analyses have demonstrated that SSRI use is associated with approximately a 1.5–2-fold increased risk of GI bleeding.
This risk becomes substantially higher when SSRIs are combined with other agents that affect hemostasis.
Nonsteroidal anti-inflammatory drugs (NSAIDs) impair platelet aggregation via cyclooxygenase-1 inhibition and also disrupt gastric mucosal integrity.
When combined with SSRIs, the risk of GI bleeding increases synergistically, with estimates ranging from 3- to 6-fold compared to baseline.
Anticoagulants and antiplatelet agents further amplify this effect.
Not all SSRIs carry equal risk.
Agents with higher affinity for SERT, such as fluoxetine, sertraline, and paroxetine, are more strongly associated with platelet serotonin depletion and may confer a higher bleeding risk compared to agents with lower SERT affinity.
This suggests a dose- and potency-dependent effect.
From a clinical standpoint, risk stratification is essential.
Higher-risk populations include:
- older adults
- patients with prior gastrointestinal bleeding
- those taking NSAIDs, anticoagulants, or dual antiplatelet therapy
- patients with liver disease or coagulopathy
- High Risk: Fluoxetine, Paroxetine, Sertraline
- Moderate Risk: Citalopram, Escitalopram, Fluvoxamine
- Lower Risk: Bupropion, Mirtazapine
This phenomenon highlights a broader concept in psychopharmacology.
Neurotransmitter systems are not confined to the brain.
Peripheral expression of targets such as SERT means that centrally acting drugs can influence systemic physiology in meaningful ways.”
Stay updated with Hemostasis Today.
-
May 23, 2026, 08:15Alexander Krupp: Asundexian Receives Priority Review Designation from China‘s NMPA
-
May 23, 2026, 07:59Toward a Dedicated Framework for MIg-Driven Hemostatic Disorders – JTH
-
May 23, 2026, 07:53Ankit Panthari: Can Haemophilia Serve as A Health System Model for Other Rare Diseases in India?
-
May 23, 2026, 07:43Ted Roh: Indonesia’s Plasma Fractionation Plant Wins Social Infrastructure Deal of the Year at the IJGlobal Awards 2025
-
May 23, 2026, 07:36Angie Read: Stories of Strength and Resilience on The Latest Episode of Stroke Sisters
-
May 23, 2026, 07:30Ozlem Fidanci: Reflections From WHA79 on the Future of Stroke Care
-
May 23, 2026, 07:21Ney Carter Borges: Where the Benefit Appears in Dual Antiplatelet Therapy
-
May 23, 2026, 05:38SIUH Advances Precision Stroke Care with Vena MicroAngioscope – Northwell Health
-
May 23, 2026, 05:31Kalyan Roy: Precision Blood Matching in Transfusion-Dependent Thalassaemia

