
Benedikt Lorenz on Liver Failure and Coagulation – Myths, Traps, and Bad Habits
Benedikt Lorenz, Senior Physician, Interdisciplinary Surgical Intensive Care Medicine at Schleswig-Holstein University Hospital, shared on LinkedIn:
”Liver failure and coagulation – myths, traps, and bad habits.
Liver failure and hepatic insufficiency cause profound changes in standard lab tests — and anyone treating these patients must know the pitfalls.
A colleague asks whether to give PCC before inserting a Shaldon catheter for ADVOS therapy in a patient with right heart failure and liver failure.
“We never give PCC blindly – except
A) if a patient is on warfarin and bleeding, or
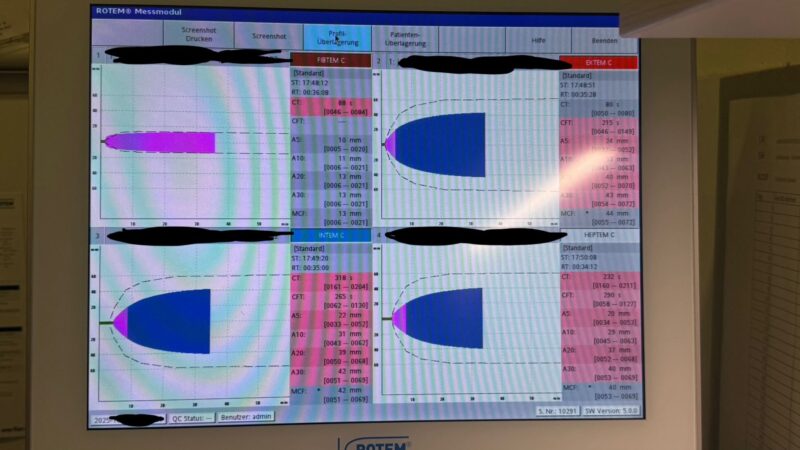
B) if the ROTEM shows a prolonged CT in the EXTEM after (!) correction of hypofibrinogenemia and/or thrombocytopenia!”
This patient with a Quick of 26% and INR 2.46 must not receive PCC — the clotting time is perfectly normal.
If this patient bleeds, he needs fibrinogen concentrate (never plasma or whole blood – hypervolemia only makes things worse! [portal hypertension]).
Even platelet transfusion must be considered carefully: in thrombocytopenic liver failure, VWF levels rise and ADAMTS13 activity falls, creating a prothrombotic state despite low platelet counts.
It becomes tricky, as here, after cardiac surgery, when platelet function is already impaired.
Treat first what kills first!
Coagulation therapy must be individualized – there is no one-size-fits-all recipe.
Giving PCC in this context means risking thromboembolic events, jeopardizing vascular anastomoses after liver transplantation or generally in surgery, and clogging oxygenators in ECMO or other extracorporal therapies like ADVOS oder hemodialysis circuits.
Everyone who has ever transplanted a liver knows: there is no correlation between Quick/INR and bleeding – but a very real one between PCC and thrombosis while it is super effective in patients who really need it.
And one day, even our friends in trauma surgery across the Atlantic will understand:
A low Quick is not a coagulopathy to be fixed with PCC (that’s why it doesn’t work in your studies)– it’s the footprint of hypofibrinogenemia or thrombocytopenia.
The only reliable guide in these patients? Thromboelastography.
The only reliable therapy in these patients? Pure factor concentrate.”
Stay updated with Hemostasis Today.
-
Apr 28, 2026, 16:26Andrew Zapfel: The ASH’s Consortium on Newborn Screening in Africa Brought Together Over 40 People From 10 Countries
-
Apr 28, 2026, 16:22Beth Fernandes: Bringing Alaska’s First Civilian Medevac Whole Blood Program To Life
-
Apr 28, 2026, 15:47Dianne E. van der Wal: How Rat and Human Platelet Vesicles Are Different
-
Apr 28, 2026, 15:14Elaheh Mansouri: Platelet Clumping Is a Common Pre-Analytical and Analytical Challenge in Haematology
-
Apr 28, 2026, 15:11Hans Vrielink: Honoured to Receive the Cohn the Laval Award at the ASFA/WAA
-
Apr 28, 2026, 15:07Stan Van Boeckel: Pitfalls in Early Drug Discovery
-
Apr 28, 2026, 15:02Stephani Carolina Salvatierra Moreno: Our Study on Microneedling and PRP Has Been Published
-
Apr 28, 2026, 14:57Steven Heylen: Hydrolyzed Collagen Injections for Knee Osteoarthritis as a New Treatment Option
-
Apr 28, 2026, 14:22Heghine Khachatryan: Regarding Coagulation Factor Dynamics During Pregnancy in Hemophilia B Carriers

