
Peter Antevy: EMS Rarely Suspects Pediatric Stroke And It’s Costing Kids Time
Peter Antevy, Founder and Chief Medical Officer at Handtevy, President of C3MD, EMS Medical Director at Davie Fire Rescue, shared on LinkedIn:
”When an adult stroke alert is called, the system mobilizes. The team assembles. Imaging is expedited.
Treatment protocols activate. There is a chain of survival, and everyone knows their role.
For most children, that chain dos not exist.
Most hospitals do not have a regimented process for a pediatric stroke alert.
No automatic assembly of the right team.
No standardized pathway to get the right imaging done and the right treatment started without delay.
We built that process at Joe DiMaggio Children’s Hospital over a decade ago, and it’s had a huge impact on how quickly these kids get diagnosed and treated.
Now the State of Florida Department of Health is working to make that the standard.
Add to that the work that the Florida Stroke Registry, Florida EMSC, and the Prehospital Pediatric Readiness Recognition Program are contributing, and you have a state that is building the infrastructure so that pediatric stroke readiness is not the exception but the expectation.
The chain of survival matters just as much for a seven-year-old as it does for a seventy-year-old. Lives depend on it.
For more detail please read my latest blog post on pediatric stroke recognition and the data behind why this work is so urgent.
Pediatric stroke is rare. But delayed diagnosis is common.
A seven-year-old collapses at school. The teacher calls 911. Paramedics arrive within minutes.
The child is postictal, confused, not following commands.
The EMS crew documents a seizure, starts an IV, and transports to the nearest pediatric emergency department.
Nobody considers stroke.
Twelve hours later, an MRI reveals an acute ischemic infarct in the left middle cerebral artery territory.
The child has a dense right hemiparesis. The window for intervention has closed.
This scenario is not hypothetical. It is the norm.
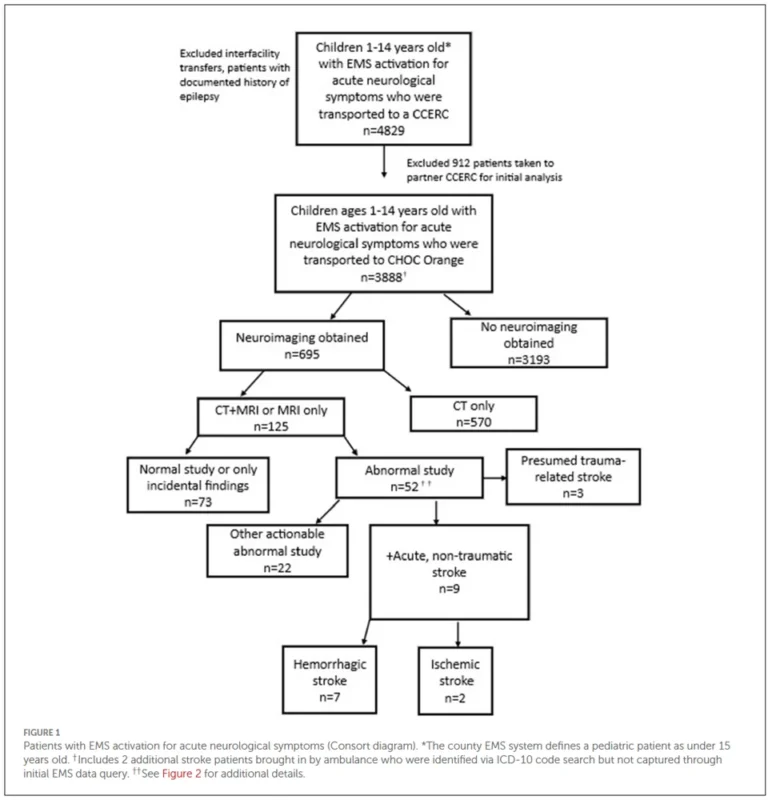
A new study from the University of California system analyzed 3,888 children transported by EMS for acute neurological symptoms over four years.
The findings put numbers behind something many of us have suspected: EMS almost never considers stroke in kids. Among nearly 4,000 activations for pediatric neurological emergencies, only 13 patients (0.3%) had an EMS primary impression of ‘stroke.’
And none of those 13 actually had one.
But here’s what caught my attention.
When EMS documented ‘stroke’ as the primary impression, 100% of those patients received neuroimaging in the ED. All 13 had CT scans.
Eleven had MRIs. In other words, when EMS framed the case as a potential stroke, the emergency department responded accordingly.
The EMS impression shaped the ED’s diagnostic approach, even when the suspicion was ultimately incorrect.
This is anchoring bias working in our favor.
For the 695 children who received neuroimaging, the median time from EMS activation to CT was 2.3 hours.
The median time to MRI was 26.8 hours.
That delay to MRI is the critical finding.
Unlike adults, where CT suffices to rule out hemorrhage and guide thrombolytic therapy, MRI is essential for diagnosing pediatric ischemic stroke.
CT misses most acute ischemic strokes in children. Among the 125 patients who received MRI, 9 had acute strokes.
Another 31 had actionable findings: CNS infections, tumors, vascular malformations.
These children needed MRI to establish the diagnosis and guide treatment.
The study also found disparities in imaging decisions.
Children under 5 were less likely to receive neuroimaging, despite being at higher stroke risk than older children.
Hispanic children were significantly less likely to be imaged compared to other races and ethnicities (15.5% vs. 20.8%). And most pediatric stroke patients didn’t arrive by EMS at all.
During the study period, 43 children were admitted with out-of-hospital stroke. Only 21% arrived by ambulance.
A third were walk-ins brought by family. Nearly half were transfers from other facilities.
None of this is surprising when you think about it.
Pediatric stroke doesn’t look like adult stroke.
Kids present with seizures, altered mental status, severe headache with vomiting, loss of consciousness.
The classic adult stroke tools we rely on, CPSS, FAST, RACE, were designed for focal deficits and aphasia, symptoms that are often subtle or absent in children.
Layer in a much higher rate of stroke mimics (migraine, seizure, trauma), and it becomes clear why EMS rarely puts stroke on the differential for a pediatric patient.
That may be starting to change.
The 2026 AHA/ASA Acute Ischemic Stroke Guidelines now include the first-ever pediatric-specific stroke screening tools, and one in particular deserves attention: the PedRACE.
The Pediatric Rapid Arterial Occlusion Evaluation scale was adapted from the validated adult RACE scale by the Catalan Stroke Network.
It is a simple 5-item assessment: facial palsy, arm motor function, leg motor function, head and gaze deviation, and aphasia or agnosia. It can be administered in about two minutes.
In a prospective study of 50 children evaluated through the Catalan Pediatric Stroke Code, prehospital and emergency staff scored the PedRACE comparably to child neurologists, with 82% full agreement across all items and a weighted kappa of 0.920.
The scale correlated strongly with the PedNIHSS for both child neurologists (Spearman ρ 0.852) and prehospital/ED staff (Spearman ρ 0.781).
A PedRACE score of 5 or higher was significantly associated with large vessel occlusion, the subset of pediatric strokes most likely to benefit from thrombectomy.”
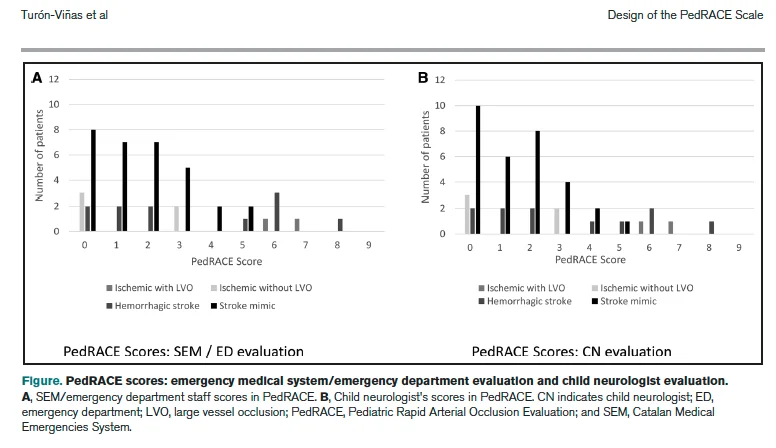
This is a tool designed for non-neurologists. It does not require advanced training.
And it gives EMS and ED clinicians a structured way to quantify what they are seeing in a child with acute neurological symptoms.
We recently added the PedRACE to our platform’s Clinical Scores library so that clinicians can access it at the point of care, right alongside the tools they already use every day.
The sample size is small. The sensitivity and specificity for pediatric stroke screening have not yet been established.
But this is the first prehospital tool specifically designed to detect large vessel occlusion in children. Its inclusion in the 2026 AHA/ASA guidelines signals that the field is ready to move beyond awareness and toward action.
And we already have proof that action matters. This study shows that EMS documentation influences ED decision-making.
When EMS raises the possibility of stroke, hospitals respond.
Clear documentation in the EMS report, direct verbal handoff highlighting stroke concern, prehospital notification for suspected large vessel occlusion when protocols support it.
These are not expensive interventions. They are communication. And they change the trajectory of care.
One more finding worth highlighting. Adult stroke care uses ‘door-to-needle’ and ‘door-to-puncture’ times as quality metrics.
Those don’t work for pediatric stroke.
The authors propose ‘door-to-diagnosis’ as the key metric for children: time from ED arrival to CT for suspected hemorrhagic stroke, and time from ED arrival to MRI for suspected ischemic stroke.
This accounts for the reality that MRI is essential for pediatric stroke diagnosis, while CT suffices for adults. If we are going to improve outcomes, we need a way to measure progress.
This is a good start.
EMS clinicians almost never suspect stroke in kids. But when they do, it changes everything that happens next.
The opportunity here is not perfect stroke recognition in the field.
That is unrealistic given how rare pediatric stroke is and how often it mimics other conditions.
The opportunity is making sure stroke stays on the differential when a child presents with acute neurological symptoms.
A structured tool like the PedRACE. A clear EMS impression. A verbal handoff that names the concern.
In pediatric stroke, where median time to diagnosis is still approximately 24 hours from symptom onset, even small improvements save brain.
Sources:
- Pearson R, et al. Striving toward quality metrics for pediatric stroke: time from door to diagnosis. Front. Stroke. 2025.
- Turón-Viñas E, et al. Design and interrater reliability of the pediatric version of the RACE scale: PedRACE. Stroke. 2024;55:2240–2246.”
Title 1: Striving toward quality metrics for pediatric stroke: time from door to diagnosis
Authors: Rachel Pearson, Nancy K. Hills, Kellie Bacon, Shelby K. Shelton, Rowena Roque, Tatiana Moreno, Maria Kuchherzki, Carl Schultz, Theodore W. Heyming, Christine K. Fox, Heather J. Fullerton
Read the Full Article on Frontiers

Title 2: Design and interrater reliability of the pediatric version of the RACE scale: PedRACE
Authors: Eulàlia Turón-Viñas, Susana Boronat, Ignasi Gich, Verónica González Álvarez, Montserrat García-Puig, Maria Camós Carreras, Agustí Rodriguez-Palmero, Ana Felipe-Rucián, Gemma Aznar-Laín, Xavier Jiménez-Fàbrega, Natalia Pérez de la Ossa, Catalan Pediatric Stroke Study Group
Read the Full Article on Stroke

Stay updated on all scientific advances with Hemostasis Today.
-
Apr 29, 2026, 17:25Robert Brodsky: Ravulizumab Appears To Be Safe And Effective In Pregnancy
-
Apr 29, 2026, 16:53Chokri Ben Lamine: IV Iron Showdown – FCM vs Ferric Derisomaltose vs Iron Dextran
-
Apr 29, 2026, 16:46Deep Vein Thrombosis Risk in Jobs with Prolonged Sitting – NBCA
-
Apr 29, 2026, 16:41Vikramaditya Gangakar: Essential Pharmacy Facts You Should Know About Aspirin
-
Apr 29, 2026, 16:17W. Alberto Sifuentes Giraldo: Non-Criteria Manifestations of Antiphospholipid Syndrome
-
Apr 29, 2026, 16:12Mavis Agnes Kisakye: Concluding a Successful Entrepreneurs Training for Empowering Ptients’ Mothers
-
Apr 29, 2026, 15:48Kriti Batni: Happy to Share Current Use and Future Directions of Monoclonal Antibodies in Medicine Update 2026
-
Apr 29, 2026, 15:46Dima Shulkin: Comparing HALP and PIV for Mortality Prediction in ACS
-
Apr 29, 2026, 15:44Sonal Sonu: Securing First Prize in Research Oral Presentation at the CME

