Chokri Ben Lamine: Hematology Pearls on Portal Vein Thrombosis
Chokri Ben Lamine, Adult Hematology and SCT Assistant Consultant at Oncology Center of Excellence at King Faisal Specialist Hospital and Research Center, shared a post on X:
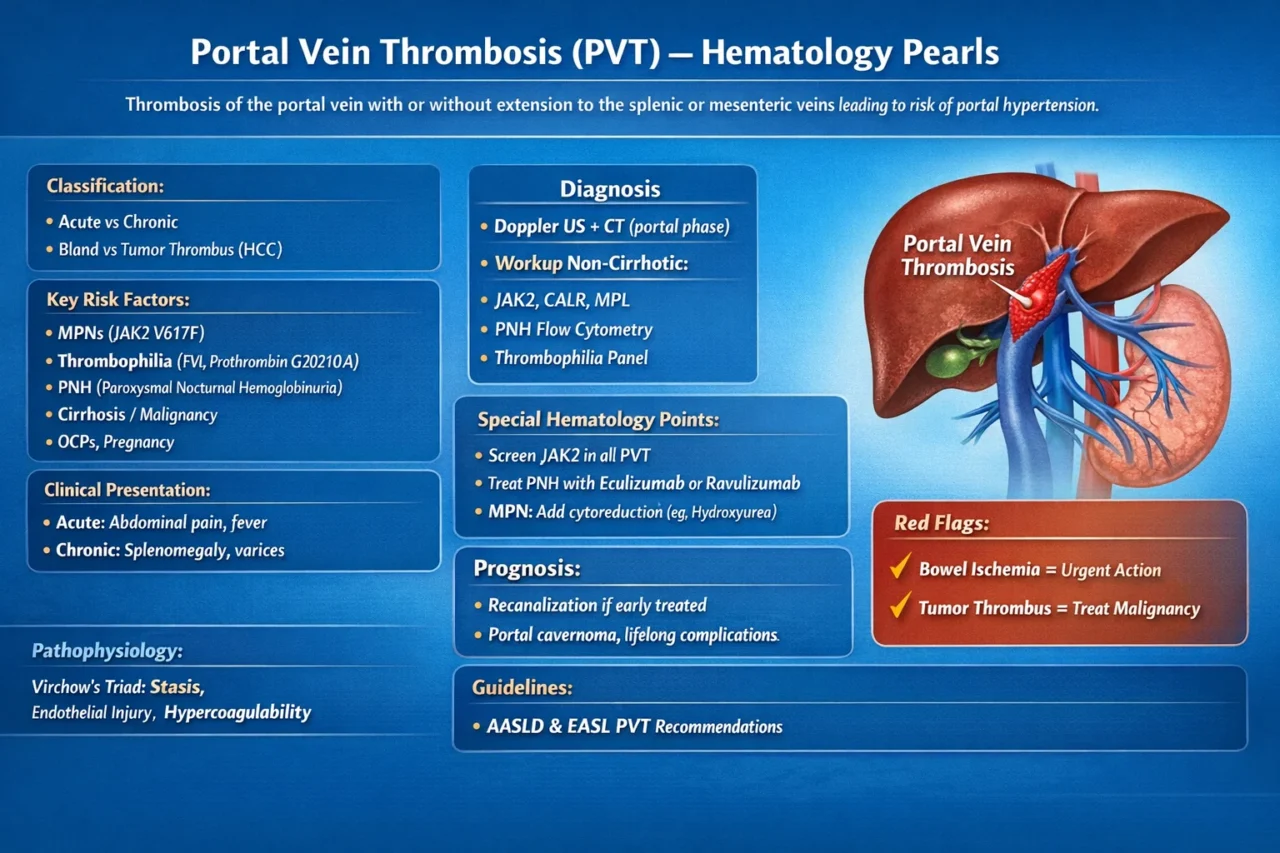
“Portal Vein Thrombosis (PVT) – Hematology Pearls
Thrombosis of the portal vein with or without extension to the splenic vein or superior mesenteric vein leading to risk of portal hypertension
Classification
- Acute vs chronic
- Bland vs tumor thrombus ( HCC)
Key Risk Factors:
- MPNs (especially JAK2 V617F positive) are the most common systemic cause
- Thrombophilia:
- Factor V Leiden
- Prothrombin G20210A mutation
- Decreased Protein C and Protein S
- Decreased Antithrombin
- PNH (always screen in unexplained PVT)
- Intra-abdominal infection/inflammation (appendicitis, pancreatitis)
- Cirrhosis / malignancy
- OCPs, pregnancy
Pathophysiology:
Virchow triad leads to portal flow stasis and endothelial injury, and hypercoagulability
Clinical Presentation:
Acute: abdominal pain, fever, nausea, increased lactate (if bowel ischemia).
Chronic: asymptomatic progressing to splenomegaly, varices, and thrombocytopenia.
Diagnosis:
- Doppler US is first line
- CT in the portal venous phase is the gold standard for assessing the extent of disease and for detecting bowel ischemia.
- Workup ALL non-cirrhotic:
- JAK2 positive or negative, CALR or MPL
- PNH flow cytometry
- Thrombophilia panel (selective, timing matters)
Red Flags
- Bowel ischemia leads to urgent anticoagulation and surgery
- Tumor thrombus leads to no anticoagulation alone (treat malignancy).
Management (Guideline-based):
- Anticoagulation is the cornerstone.
- LMWH changes to DOAC or VKA (individualized).
- Duration is three to six months or more.
- Indefinite if there is MPN or it is unprovoked.
Cirrhosis:
- Anticoag SAFE if no active bleeding (AASLD/EASL)
- Improves recanalization
Interventions:
- TIPS is indicated for refractory portal hypertension or disease progression.
- Thrombolysis is used in selected acute severe cases.
Monitoring:
- Imaging at three months shows recanalization.
- Platelets decreased, consider hypersplenism or MPN evolution.
Special Hematology Points:
- Always screen JAK2 in splanchnic thrombosis EVEN with normal CBC
- PNH clone is treated with Eculizumab or Ravulizumab.
- MPN-associated cases require adding cytoreduction, for example, with hydroxyurea.
Prognosis:
- Recanalization if early anticoag
- Chronic cases lead to portal cavernoma and lifelong complications.
Key Studies:
- AASLD 2020 guidance (vascular liver disorders)
- EASL 2016 PVT guidelines
- DeLeve LD et al., Hepatology.”
Stay updated with Hemostasis Today.
-
May 28, 2026, 09:16Maxime Dely: The Human Connection Behind Stem Cell Donation
-
May 28, 2026, 09:15Heghine Khachatryan: Maternal Health Begins With Recognizing Iron Deficiency Early
-
May 28, 2026, 09:15Alejandro González Veliz: Why Cardiovascular Prevention Matters More Than Intervention
-
May 28, 2026, 05:29Kidist K.: First Balloon Pulmonary Angioplasty Performed as New CTEPH Program Launches
-
May 28, 2026, 04:59Maria Sol Andres: Exploring Lipid Disorders in Modern Cancer Care
-
May 28, 2026, 04:42Francesca Granata: Representing the Porphyria Community at the 79th World Health Assembly
-
May 28, 2026, 04:29Samone Cook: When Collaboration Turns Into Organizational Coagulation
-
May 28, 2026, 03:42Lara Bloom: 15,000 Steps, Countless Conversations – One Unforgettable WHA79
-
May 27, 2026, 23:00Octavio Marques Pontes-Neto: Exchanging Latin American Experiences at the Global Stroke Alliance Meeting in Buenos Aires

