
Khaled Kandil: A Rare Case of Recurrent Thromboembolism with Pulmonary Artery Aneurysms
Khaled Kandil, Professor of Internal Medicine at Faculty of Medicine Azhar University, shared on LinkedIn:
”Case Presentation :
A 36 – year- old man with medical history of inferior vena cava thrombus and recurrent pulmonary embolism (PE) presented to ER with fever , malaise, and night sweats for 3 days and hemoptysis (approximately half a tablespoon) in the last 24 hours.
He reports the first diagnosis of inferior vena cava thrombus in December 2022, when he presented with similar symptoms and was started on apixaban.
Since then , he had 3 additional episodes in the following 6 months in which he was found to have a recurrent PEs despite compliance and changes in regimen (warfarin then enxoparin).
However, this first episode of hemoptysis.
Patient has never smoked, abd denies personal and family history of coagulopathy or cancer.
Physical Examination Findings
- The patient was febrile ( 39.6 C ).
- Heart rate 108 beats/min.
- Respiratory rate 16 breaths/ min.
- He appeared already and without any signs of stress.
- No rashes, or oral or genital ulcers, eye pain or redness, visual disturbances.
- No lack of strength in extremities, or joint pain/ stiffness.
- All other aspects if Physical examination were within normal limits.
Diagnostic Studies:
- Initial laboratory work up, including: CBC , comprehensive metabolic panel, and CXR were unremarkable.
- Inflammatory markers were elevated (C- reactive protein CRP 160mg/dl and ESR 144 mm/h.
- Urine analysis showed microscopic Hematuria with 3- 10 RBCs per field.
- Doppler ultrasound of both legs was negative for clots.
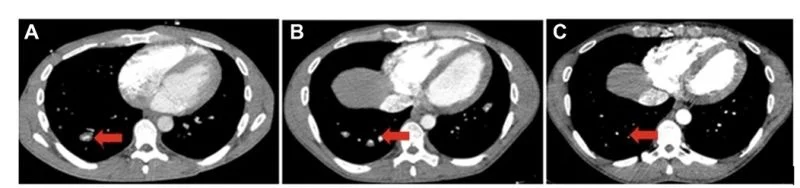
- CT scan of the chest with contrast revealed new, multiple dilated and aneurysmal pulmonary arteries and veins with in situ thrombosis A .
- Additional evaluation took place to elucidate the cause of recurrent thromboembolism and systemic inflammation.
Hypercoagulable work-up was negative, including IgG/IgM, anticardiolipin and IgG/IgM anti- B2GPI and inherited thrombophilia markers
- Autoimmune serologies including anti nuclear antigen and antinuclear cytoplasmic antibodies were negative.
- Blood Culture and all microbiologic work-ups were negative as well.
Organ- specific evaluations included a kidney biopsy showing mild glomerular microangiopathy and acute tubular injury but without evidence of vasculitis.
BM biopsy which was normocellular with trilineage hematopoiesis and no dysplasia of blast proliferation.
Flow Cytometry revealed no abnormal blast cells.
What is your diagnosis?”
Stay updated with Hemostasis Today.
-
Jun 1, 2026, 11:16Ocima Richard Draza: Postpartum Hemorrhage – A Practical Step-by-Step Management Guide
-
Jun 1, 2026, 10:57Kyungjun Lim: How Will Future Mars Colonies Manage Their Supply Chains?
-
May 31, 2026, 16:29José Antonio García Erce: Collaborative PBM Implementation in Transfusion Centers and Services
-
May 31, 2026, 16:22Vera Ignjatović: How Do We Rigorously Study These Drugs in Children to Understand Their True Benefits and Risks?
-
May 31, 2026, 16:21Ksenija Stach: Is This The Future of Lipid-Lowering Lherapy?
-
May 31, 2026, 15:42Antonio Greco: Balancing Bleeding and Thrombotic Risk After PCI
-
May 31, 2026, 15:41Eric Topol: Replication of Plasma p-tau217 Blood Test for Predicting Alzheimer’s Disease
-
May 31, 2026, 15:32ASH Invites Dynamic Members to Apply for 2027 Leadership and Committee Roles
-
May 31, 2026, 14:39Monique Gore-Massy: Redefining Lupus Innovation Through Patient Partnership

