
Dr Abdul Mannan: What’s Your Approach to Diagnosing Iron Deficiency in Tricky Cases?
Dr Abdul Mannan, Consultant Haematologist at Betsi Cadwaladr University Health Board, posted on LinkedIn:
“After years of managing anaemia across different patient populations, I’ve learned one thing: that single ferritin number on your screen? It’s not telling you the whole truth.
Let me explain with three patients I see regularly.
Patient 1: The “Normal” Pregnant WomanHer ferritin comes back at 20 µg/L.
“Normal range,” says the lab slip.
But here’s what the lab doesn’t know: she’s growing a human being. That baby needs iron. Her expanding blood volume needs iron. We’re talking about 1 gram of additional iron over 9 months.
A ferritin of 20 in pregnancy? That’s not normal. That’s a deficiency waiting to cause problems.
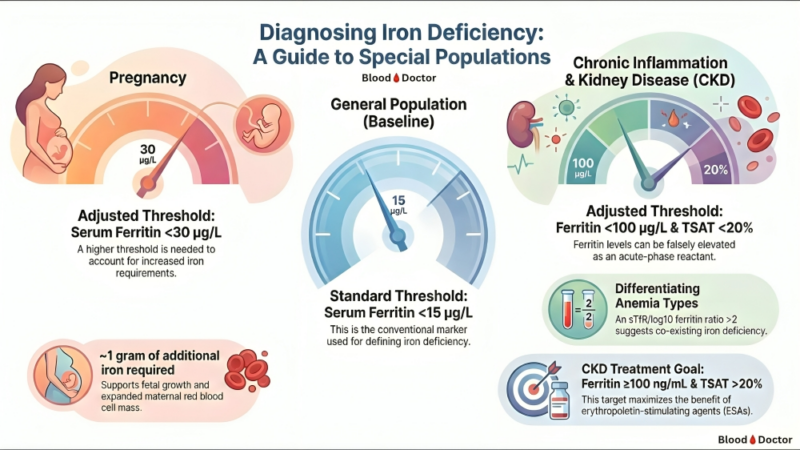
The fix: In pregnancy, think <30 µg/L as your red flag.
Patient 2: The CKD Patient with “Adequate” Iron
Ferritin: 85 µg/L.
Looks fine, right?
Wrong.
This patient has chronic kidney disease. Inflammation. Ferritin is an acute phase reactant — it rises when the body is inflamed, regardless of actual iron stores.
I’ve seen CKD patients with ferritin of 200 who were profoundly iron deficient.
The fix: In CKD and inflammation, you need TWO numbers: → Ferritin <100 µg/L AND → Transferrin saturation <20%
Both. Not one. Both.
And when you’re really stuck? The sTfR/log10 ferritin ratio >2 points toward true iron deficiency hiding behind inflammation.
Patient 3: The Textbook Case
Healthy adult. No inflammation. No pregnancy.
Ferritin <15 µg/L = iron deficiency.
Simple. Clean. The one time ferritin actually behaves.
The Bottom Line:
One number. Three completely different interpretations depending on who’s sitting in front of you.
Medicine isn’t about memorizing reference ranges. It’s about knowing when those ranges don’t apply.
The best doctors I know don’t just read results. They read context.
Quick Reference:
General population: Ferritin <15 µg/L
Pregnancy: Ferritin <30 µg/L
CKD/Inflammation: Ferritin <100 µg/L + TSAT <20%
Save this. Share it. Your patients will thank you.
What’s your approach to diagnosing iron deficiency in tricky cases?”
Follow the latest with Hemostasis Today.
-
May 8, 2026, 09:25Athma Dias: Limitations of PT and APTT in Predicting Thrombotic Risk
-
May 8, 2026, 09:12Abhishek Kumar: New Horizons in Hemophilia B Treatment and Prevention
-
May 8, 2026, 08:19Augustina Isioma Ikusemoro: Thalassaemia is not Just a Blood Disorder – It is a Public Health Priority
-
May 8, 2026, 06:24Transforming Thrombosis Management With Antithrombotic Stewardship – Anticoagulation Forum
-
May 8, 2026, 06:03Risk-Stratified HRT Use Following VTE – NBCA
-
May 7, 2026, 17:56The Latest Clinical Data Shaping The Evolving Landscape of Hemophilia Treatment – EAHAD
-
May 7, 2026, 17:31Talha Badar: New Classical Hematology Chapter on Bleeding and Thrombosis
-
May 7, 2026, 17:26Maria Τektonidou: Gene Network Analysis Identifies STAT1 in Thrombotic APS
-
May 7, 2026, 17:23Sonu Bhaskar: Inflammatory Biomarkers in Acute Cerebral Venous Sinus Thrombosis

