
8 Posts Not to Miss From the ASH 2025 – Marc Carrier
The American Society of Hematology Congress 2025 (ASH25) is officially underway in Orlando, Florida, from December 6 to 9.
It aims to bring together hematology professionals from across the globe.
Throughout the meeting, experts presented new research, clinical breakthroughs, and innovations that are defining the future of hematologic care.
Marc Carrier, Professor at Ottawa Hospital Research Institute, shared following posts from ASH 2025 on LinkedIn and X:
1.”New Insights on Bleeding Risk During Extended Anticoagulation in Cancer-Associated VTE
Presented at ASH25 and published in Lancet Haematology, this post-hoc analysis of the API-CAT trial, led by Prof. Isabelle Mahé identifies key predictors of clinically relevant bleeding during extended apixaban therapy in patients with active cancer.
Key Predictors of Higher Bleeding Risk
• Anemia and/or thrombocytopenia (HR 1.93)
• Age ≥75 years (HR 1.51)
• Index pulmonary embolism (HR 1.47)
• Male sex (HR 1.38)
These predictors were consistent across cancer types and also aligned with predictors of major bleeding.
See manuscript.
 ”
”
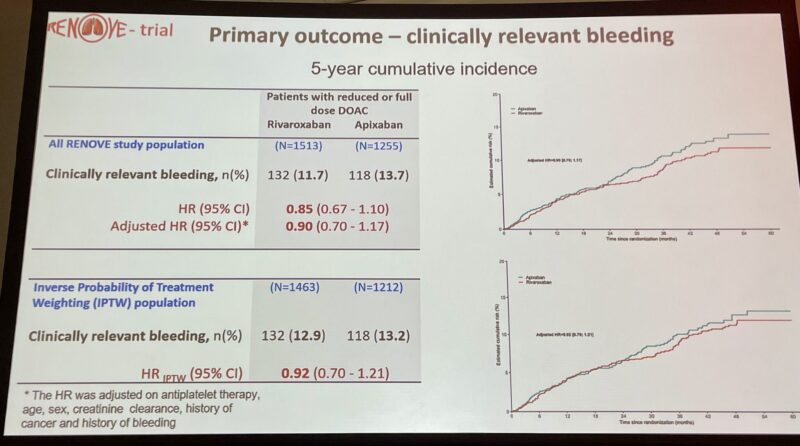
2.”ASH25 Highlight – Extended Anticoagulation in VTE: Apixaban vs Rivaroxaban
Important new insights from a post-hoc analysis of the RENOVE randomized trial, evaluating safety during extended treatment (after ≥6 months of full-dose therapy) with apixaban or rivaroxaban by Prof Francis Couturaud
Key Findings (5-year outcomes):
• Clinically relevant bleeding (CRB): Similar between drugs at both full and reduced doses.
• Major bleeding: No significant differences across subgroups.
• Recurrent VTE: Low and comparable with both agents.
• Dose reduction: Consistently lowered CRB risk for both apixaban and rivaroxaban.
Takeaway:
Unlike early-treatment data where rivaroxaban shows higher bleeding risk, during extended therapy the safety profiles of apixaban and rivaroxaban appear equivalent.
More trials are needed.
Read the full article here.
 ”
”
3.”Congratulations to Dr. Mysa Saad on her first oral presentation at ASH25!
Does concurrent antiplatelet or NSAID use increase bleeding risk in cancer patients receiving apixaban thromboprophylaxis?
Key Findings:
• Among patients receiving prophylactic apixaban, concurrent antiplatelet/NSAID use significantly increased clinically relevant bleeding (HR 1.78) and CRNMB (HR 1.98).
• No reduction in VTE was observed (HR 0.60).
• In subgroup analyses:
– Antiplatelet agents were the main driver of increased bleeding (CRNMB HR 2.59).
– NSAIDs did not show a significant impact on bleeding or VTE.
• Mortality outcomes were unaffected.
Implications:
These results highlight the need to carefully reassess antiplatelet/NSAID indications and conduct individualized bleeding risk evaluations when considering apixaban prophylaxis in cancer outpatients.
Read the full article here.

 ”
”
4.”Huge congratulations to Dr. Abdulrahman Al Raizah on delivering his first ASH presentation!
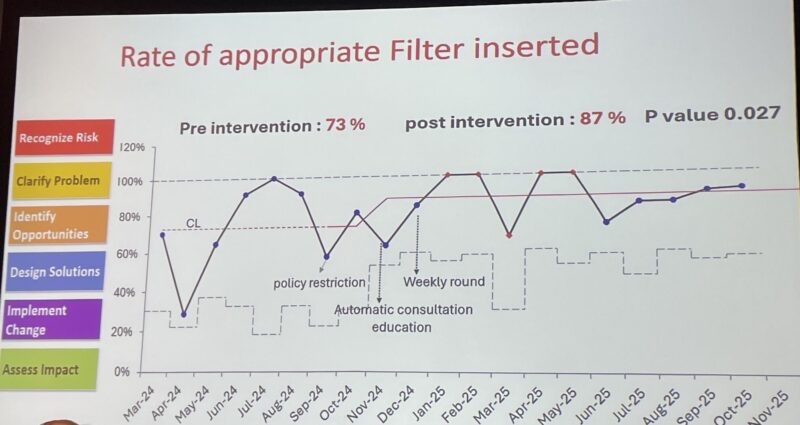
His team’s quality-improvement project tackled two major challenges in IVC filter use: insertion without proper indication and delayed retrieval.
Through a coordinated, system-level strategy, they achieved:
• Appropriate filter use: 72.7% → 91.4%
• Retrieval among eligible patients: 76% → 92.3%
• Median retrieval time: reduced from 35 to 22 days
A fantastic example of how evidence-based policy, education, and workflow redesign can meaningfully improve thrombosis care.
Read the full article here.
 ”
”
5.”Congratulations to Dr. Elena Butera on her first poster presentation at ASH!
An important contribution to the limited evidence base on cancer-associated ovarian and renal vein thrombosis (OVT/RVT).
Study highlights (n = 82):
• 98% of OVT/RVT events were incidental
• 82% received anticoagulation (64% LMWH, 31% DOAC)
• Recurrent VTE: 3.8% at 6 and 12 months
↳ 1.5% with AC vs. 14.3% without
• Major bleeding: 2.5%, all on therapeutic LMWH
• 12-month mortality: 25%
Takeaway: Anticoagulation appears effective with modest bleeding risk, providing valuable real-world data for these rare and understudied unusual-site VTEs.
Read the full article here.”
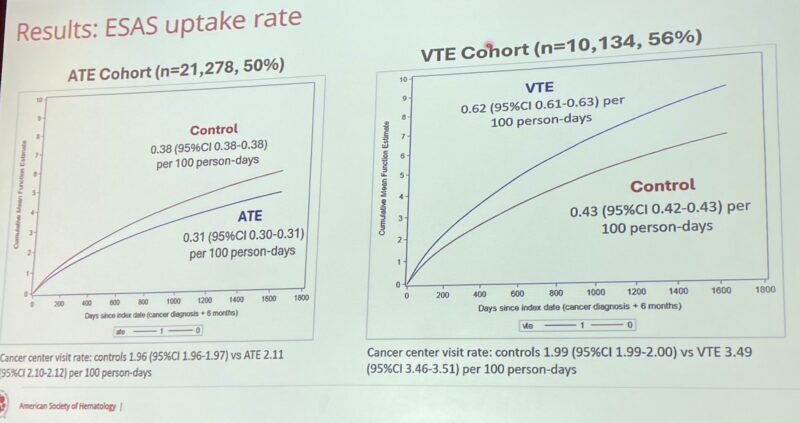
6.”ATE and VTE worsen symptom burden in cancer
In a population study (n≈59K), ATE lowers ESAS uptake, despite high clinic visits, while VTE increases ESAS use.
Both ATE and VTE led to higher odds of worsening pain, anxiety, depression, SOB and wellbeing.
Supports better monitoring + thromboprophylaxis.
Read the full article by Deborah Siegal and Colleagues here.
 ”
”
7.”Cancer-associated bleeding in the US: new data from >1.6M patients ASH25
• 12-mo bleeding: 3.9% overall; 4.5% with systemic therapy
• GI bleeds 2.1% most common; ICH 0.5% but deadly
• High-risk: leukemia, HCC, upper GI, brain mets
• ICH (HR 5.5) and GI bleed (HR 3.5) ↑ mortality
Read the full article by Ang Li and Colleagues here.
 ”
”
8.”Pregnancy-associated VTE and racial disparities at ASH25
In a population study of 442,816 pregnancies, 1,793 VTEs occurred (4.0/1,000).
Asian and Black individuals had lower VTE incidence (aRR 0.48 and 0.73) but more diagnostic delays plus higher acute-care use after VTE.
17-fold increase in ED visits in week pre-diagnosis
Read the full article by Yan Xu and Colleagues here.
 ”
”
All from ASH25 featured in Hemostasis Today.
-
Apr 30, 2026, 18:19Deva Nanda TK: A Practical Overview of Dural Sinuses and The Venous Drainage of the Brain
-
Apr 30, 2026, 18:08Amrit Kaur Kaler: The Hidden Genetic Drivers of Thrombosis
-
Apr 30, 2026, 18:06Alejandro González Veliz: The Most Dangerous Mistake After Getting a Stent
-
Apr 30, 2026, 18:03Carmen Ruiz: First Arterial Mechanical Thrombectomy in New Zealand Using the ARTIX System
-
Apr 30, 2026, 17:52Simon Senanu: von Willebrand Disease May Be Missed Despite Normal Tests
-
Apr 30, 2026, 17:20José Antonio García Erce: Why Healthy Older Adults Should Keep Donating Blood?
-
Apr 30, 2026, 17:13Paul Logan: Decoding the Words ‘He’s on blood thinners’
-
Apr 30, 2026, 17:01Jason Andrade: A Decade-Long Quest Proves Early Ablation Halves Persistent AF Burden
-
Apr 30, 2026, 16:56Oliver Maracic: Could Co-Targeting ALK with FAK/PYK2 Help Mitigate the High VTE Burden Seen in ALK with NSCLC

