
Soroush Sohrabi: The Hidden Biology of Sclerotherapy and Mechanisms Beyond Endothelial Injury
Soroush Sohrabi, Consultant vascular and ednovascular surgeon at NMC Healthcare, shared a post on LinkedIn:
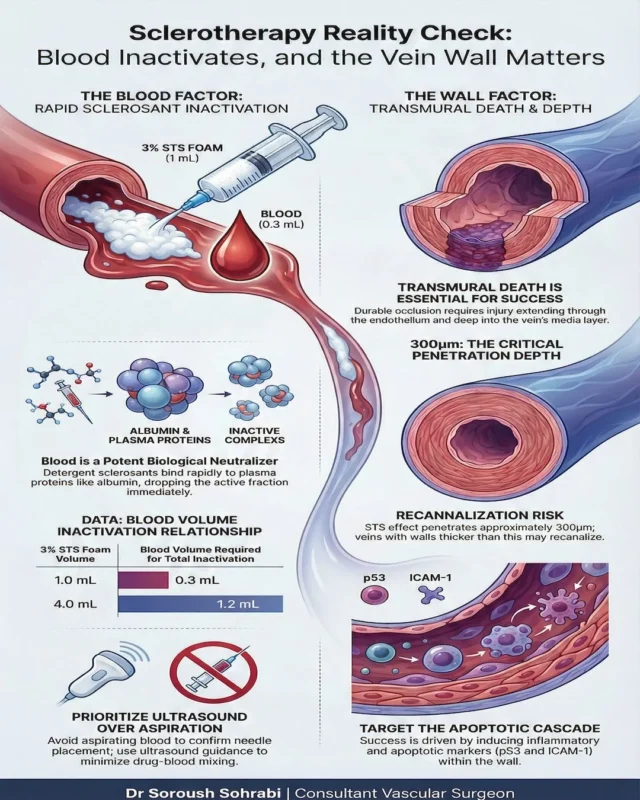
“Sclerotherapy Reality Check: Blood Inactivates — and the Vein Wall Matters
We often describe sclerotherapy in simple terms: inject the sclerosant, damage the endothelium, the vein closes.
The biology is more complex.
Two important experimental studies help clarify what is really happening:
‘Implication of foam sclerosant inactivation by human whole blood in a laboratory setting’
and
‘Media Damage Following Detergent Sclerotherapy Appears to be Secondary to the Induction of Inflammation and Apoptosis: An Immunohistochemical Study Elucidating Previous Histological Observations.’
These papers demonstrate two critical realities.
- First, blood is not passive. It actively reduces sclerosant activity. Detergent agents rapidly bind to plasma proteins such as albumin, forming inactive complexes. Even small volumes of blood can significantly decrease the active fraction available to act on the vein wall.
- Second, durable vein closure depends on more than superficial endothelial injury. Successful treatment requires deeper medial damage driven by inflammatory and apoptotic pathways. If injury remains too superficial relative to wall thickness, recanalisation becomes more likely.
In simple terms:
- Blood reduces effective drug activity
- The vein wall response determines durability
- Endothelial irritation alone is not enough
Why this matters clinically ?
These mechanistic insights help explain why outcomes vary:
- Larger veins behave differently from smaller veins
- Technique influences drug–wall contact time
- Mixing with blood reduces effective concentration
- Wall thickness influences long-term closure
- Sclerotherapy is not just a chemical injection. It is a biological interaction between sclerosant, blood, and vessel wall.
Understanding that interaction helps us refine technique, counsel patients more accurately, and improve durability of results.
What changes, if any, have these mechanisms prompted in your own approach to sclerotherapy?”
Stay updated with Hemostasis Today.
-
May 25, 2026, 10:30Rob Mac Sweeney: Prevention and Treatment of Thrombosis in Patients With Decompensated Cirrhosis
-
May 25, 2026, 07:34Wolfgang Miesbach: The Maastricht Bleeding Cohort and The High Prevalence of BDUC in Women
-
May 25, 2026, 07:31Maya Brown-Zimmerman: Bridging Patient Experience and Genetic Counseling in Marfan Syndrome
-
May 25, 2026, 05:25Abdullah Mohsin: Automated Detection of DVT Using Deep Learning and Doppler Ultrasound
-
May 25, 2026, 05:07The Dual Role of PAI-1 Mutations in Bleeding and Thrombotic Disorders – ICHCC
-
May 25, 2026, 05:04Fibrinogen αC Domain Lysines Drive Plasminogen Binding and Plasmin Generation – JTH
-
May 25, 2026, 04:50Gülşah Türkoğlu: An Encouraging Momentum Around the Adoption of Resolutions on Stroke Care at WHA79
-
May 25, 2026, 04:47Krishnakant Prasad: A Quick Clinical Review of Renal Papillary Necrosis
-
May 25, 2026, 04:40Rajiv Kumar Jain: World Health Assembly Adopts First-Ever Global Resolution on Stroke Prevention and Care

