
Sumedha Dash: Why Whole Blood is Rarely the Answer Anymore?
Sumedha Dash, Transfusion Medicine specialist at Institute of Medical Sciences and Sum Hospital, shared a post on LinkedIn:
“Why Whole Blood Is Rarely the Answer Anymore?!
For decades, whole blood was the default response to anemia and blood loss. Today, transfusion medicine has moved far beyond this one size fits all approach.
Modern transfusion practice is built on component therapy. Instead of transfusing whole blood, we transfuse only what the patient actually needs.
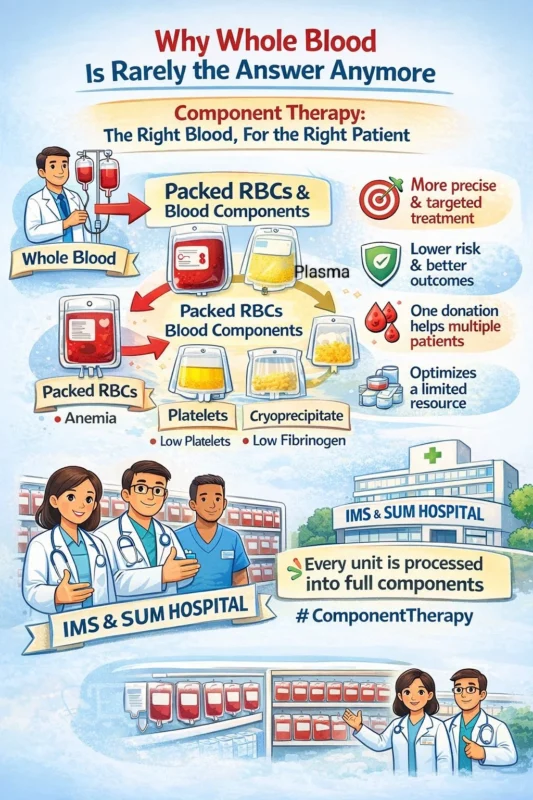
Why component therapy makes more clinical sense:
- Packed Red Blood Cells (PRBCs) – Improve oxygen-carrying capacity in anemia
- Platelet concentrates – Prevent or control bleeding in thrombocytopenia
- Plasma – Correct coagulation factor deficiencies
- Cryoprecipitate – Target fibrinogen deficiency
Each component addresses a specific physiological problem, avoiding unnecessary volume overload and reducing transfusion-related risks.
The clinical impact:
- Better patient outcomes
- Lower risk of transfusion reactions and circulatory overload
- More rational and ethical use of a limited resource
- One donation benefits multiple patients, not just one
Good clinical practice and patient blood management (PBM)
At IMS and SUM Hospital, Bhubaneswar, Odisha, every unit collected is processed into full blood components, ensuring optimal utilization of each donation and delivering targeted, evidence-based transfusion support across all clinical specialties.
Whole blood still has select indications—such as massive hemorrhage protocols or specific trauma settings, but it is no longer the routine answer.
Despite the shift toward component therapy, whole blood still has a role in carefully selected clinical situations.
In cases of massive hemorrhage, particularly in severe trauma, battlefield injuries and uncontrolled acute blood loss, low-titer group O whole blood can provide rapid volume replacement along with red cells, plasma and platelets in a single product.
When time is critical and component therapy may delay resuscitation, whole blood can support early hemostasis and improve survival.
However, its use requires strict protocols, appropriate donor selection, and robust transfusion services and it is best viewed as a targeted tool for specific emergencies rather than routine transfusion practice.
However, these advanced component separation and transfusion facilities are still not universally available across many blood centers, particularly in resource-limited and peripheral settings.
As a result, patients may continue to receive whole blood by default rather than targeted components, not because it is ideal, but because it is the only option available.
Bridging this gap requires investment in infrastructure, trained manpower, quality systems, and policy support to ensure equitable access to safe and evidence-based transfusion care.
Transfusion medicine today is not about giving more blood, it’s about giving the right blood.”
Stay updated with Hemostasis Today.
-
May 30, 2026, 18:12Khokon Miah Akanda: FDA Approves a First-in-Class Hypertension Drug
-
May 30, 2026, 18:11Alessandro Perrella: It is Not Only about “How High the CRP is”, but “in Which Patient” We are Measuring That Value
-
May 30, 2026, 18:11Jasper van Grunsven: Grateful for Our Rare Disease Team and the Commitment That Drives Our Mission
-
May 30, 2026, 18:10Open Registration for the 2026 Thrombosis Canada Annual Education Conference – Thrombosis Canada
-
May 30, 2026, 18:09Peter Zdziarski: Approval Does Not Mean NovoSeven is 100% Effective or Risk-Free in GT
-
May 30, 2026, 17:07Deepak Yadav: A Privilege to Talk on ESUS at CREST Stroke Conclave 2026
-
May 30, 2026, 16:59Syed A Rizvi: Medical Scoring Systems – Small Numbers, Big Clinical Decisions
-
May 30, 2026, 16:53Timothy “Tim” Sheehan: BNY Wealth Joins the Fight Against Blood Disorders In Support of Hemophilia of Georgia
-
May 30, 2026, 16:51Nouf Bahri: Anticoagulation Initiation for New-Onset Atrial Fibrillation in Critical Illness

