
Heghine Khachatryan: Why PNH Is More Than a Hemolytic Disease
Heghine Khachatryan, Editor-in-Chief of Hemostasis Today, Head of Hemophilia and Thrombosis Center at Yeolyan Hematology and Oncology Center, shared a post on LinkedIn:
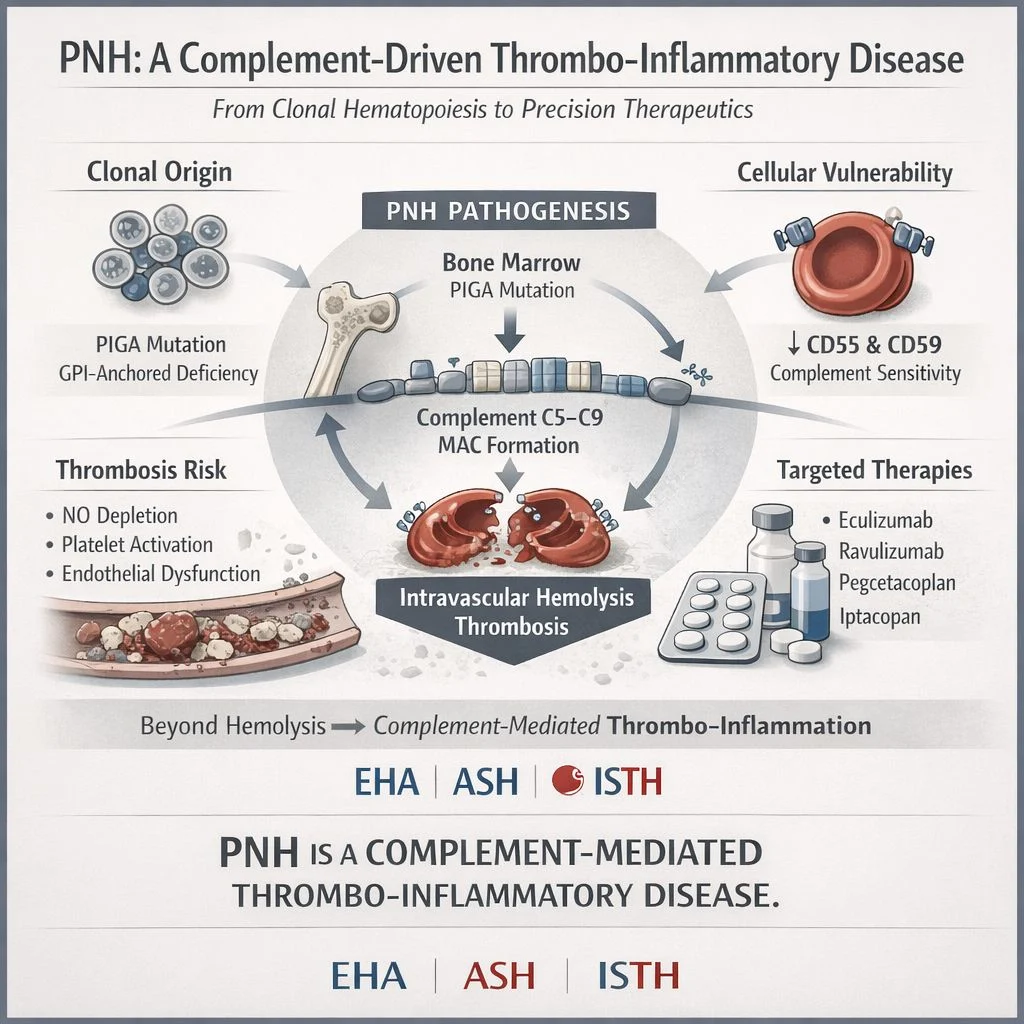
“Paroxysmal Nocturnal Hemoglobinuria (PNH): A Complement-Driven Thrombo-Inflammatory Disease
From Clonal Hematopoiesis to Precision Therapeutics
Paroxysmal nocturnal hemoglobinuria (PNH) is no longer adequately defined as a rare hemolytic anemia.
It is a clonal hematopoietic stem cell disorder characterized by complement-mediated intravascular hemolysis, systemic thromboinflammation, and variable bone marrow failure.
Mechanistic Framework (Systems-Level Perspective)
1. Clonal Origin (Bone Marrow Level)
An acquired mutation in the PIGA gene leads to defective biosynthesis of glycosylphosphatidylinositol (GPI) anchors, resulting in expansion of a pathological hematopoietic clone.
2. Cellular Vulnerability
Deficiency of GPI-anchored complement regulatory proteins:
- CD55 (decay-accelerating factor)
- CD59 (membrane attack complex inhibitor)
Erythrocytes become highly susceptible to complement-mediated injury.
3. Complement Activation (Effector Phase)
Uncontrolled activation of the terminal complement pathway (C5–C9) results in formation of the membrane attack complex (MAC) and intravascular hemolysis.
Thrombosis: The Central Determinant of Prognosis
Beyond hemolysis, PNH is one of the most prothrombotic conditions in hematology.
Data from International Society on Thrombosis and Haemostasis and European Hematology Association highlight a multifactorial pathogenesis:
- Nitric oxide depletion due to free hemoglobin
- Complement-mediated platelet activation
- Endothelial dysfunction and procoagulant shift
Resulting in high-risk thrombosis, frequently at atypical sites (hepatic, portal, cerebral veins)
Therapeutic Transformation: Complement Inhibition
Terminal Complement Inhibitors:
- Eculizumab
- Ravulizumab
- Effective control of intravascular hemolysis
- Significant reduction in thrombotic risk
- Survival approaching that of the general population
Next-Generation Strategies: Proximal Complement Targeting
- Pegcetacoplan
- Iptacopan
These agents address key limitations of C5 blockade by targeting upstream complement activation:
- Control of extravascular hemolysis
- Improved hemoglobin stabilization
- Reduced transfusion dependence
Guideline-Oriented Clinical Strategy
According to American Society of Hematology and European Hematology Association:
Initiate complement inhibition in patients with:
- Clinically significant hemolysis
- Elevated LDH (more than 1.5× ULN)
- History of thrombosis
- Selected high-risk scenarios (including pregnancy in expert centers)
Key Conceptual Insight
PNH is not merely a hemolytic disorder.
It is a complement-mediated, systemic thrombo-inflammatory disease requiring mechanism-driven intervention.”
Other posts featuring Heghine Khachatryan on Hemostasis Today.
-
May 29, 2026, 17:23Rita Schwab: Current Clinical Management of Trauma without the Use of Allogenic Blood Products
-
May 29, 2026, 17:22Brian Schiro: Excited to Provide Guideline Based Care at the Aortic Center
-
May 29, 2026, 17:20Martin Widschwendter: How Molecular Detection Tests Could Transform Endometrial Cancer Care
-
May 29, 2026, 17:18Nina Lansbury: Supporting a Period Friendly World With Menstrual Health Research and Education
-
May 29, 2026, 17:16Ipsita Chatterjee: Red is Not Shame, Red is Power, Red is a Woman
-
May 29, 2026, 16:49Abdulrahman Nasiri: The Evolving Role of Romiplostim in SAA
-
May 29, 2026, 16:46Soumen Bhattacharya: UC-II and Immune Modulation in Osteoarthritis
-
May 29, 2026, 16:38Ana Pedrero Gil: Red Blood Cell Transfusion Practice in Spain – High Inappropriateness Despite Low Overall Use
-
May 29, 2026, 15:40Lena Volland: Expanding Holistic Care in Bleeding Disorders Through Pelvic Health Physical Therapy at WFH Congress

