
Tareq Abadl: Irradiated Blood – Safer, Not More Dangerous
Tareq Abadl, Medical Laboratory Specialist and Director of the Blood Bank at Dr. Abdelkader Al-Mutawakkil Hospital, shared a post on LinkedIn:
“Irradiated Blood – Safer, Not More Dangerous.
Did you know that some blood units are actually irradiated before transfusion… not to harm, but to protect the patient?
What Does ‘Irradiated Blood’ Mean?
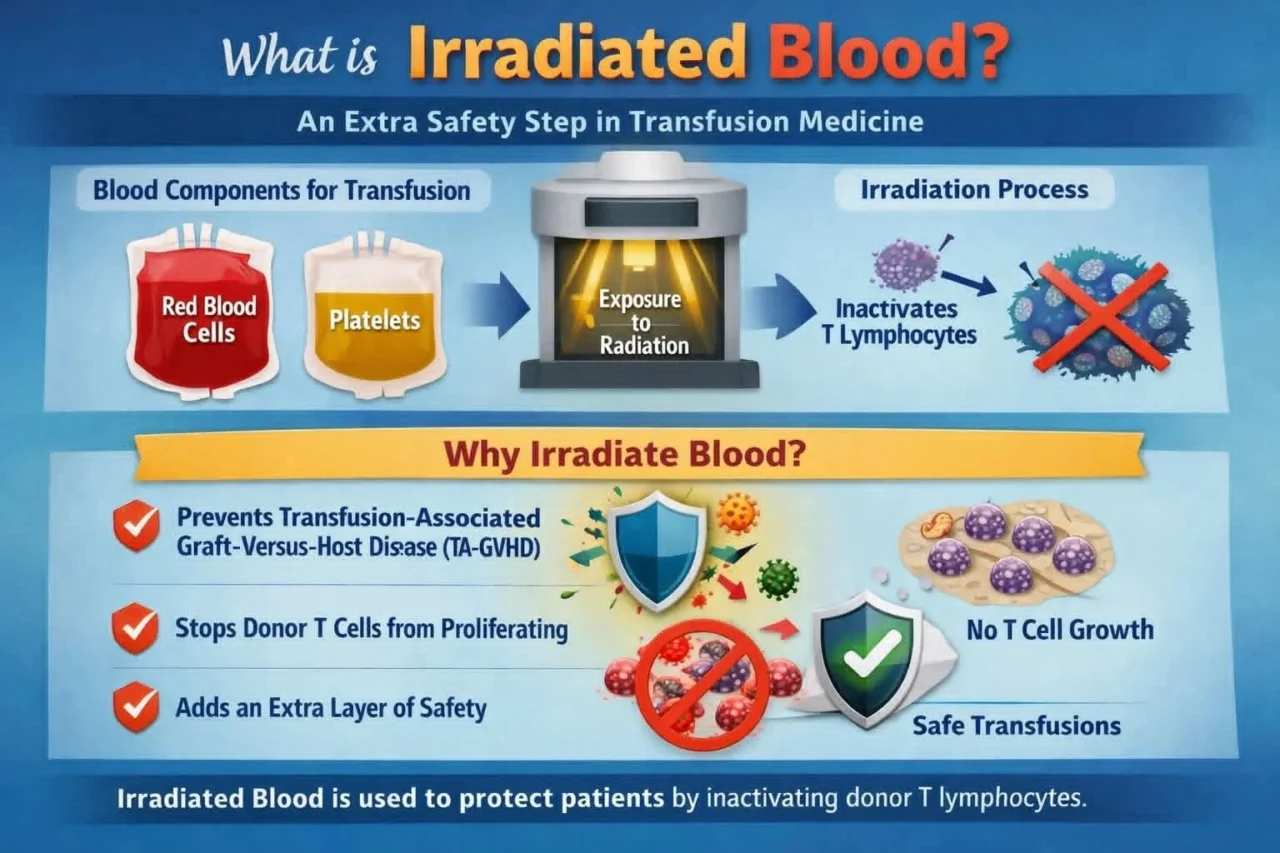
When we say a blood unit is irradiated, it means it has been exposed to controlled radiation to inactivate donor T lymphocytes.
Important:
Nothing ‘toxic’ is added to the blood — this is purely a safety modification.
Why Is Irradiation Needed?
The goal is to prevent a rare but serious complication:
Transfusion-Associated Graft-Versus-Host Disease (TA-GVHD)
This happens when:
- Viable donor T cells attack the recipient’s tissues
- Leading to severe, often fatal immune reactions
According to the AABB, irradiation is used to stop donor T cells from proliferating, eliminating this risk.
Which Blood Components Are Irradiated?
Irradiation is mainly used for cellular components, such as:
- Red Blood Cells (RBCs)
- Platelets
Plasma is not irradiated (it doesn’t contain viable lymphocytes).
Beyond ABO and Rh – Smarter Blood Banking
Modern transfusion medicine is not just about matching blood groups:
Blood banks also select specialized products based on patient needs, including:
- Irradiated components
- Washed red cells
- CMV-seronegative units
As highlighted by Canadian Blood Services, these modifications help reduce transfusion-related risks in specific clinical situations.
Does Irradiation Affect the Blood Itself?
Yes – and this is clinically important:
- Reduced shelf life
- Increased potassium levels
- Structural/biochemical changes in cells
Recent updates from AABB emphasize that irradiated products are used only when clearly indicated because of these effects.
Bottom Line
Irradiated blood is not ‘dangerous blood’ – it’s safer blood for the right patient.
In transfusion medicine:
It’s not just about giving blood…
It’s about giving the right product, to the right patient, at the right time.”
Other posts featuring Tareq Abadl on Hemostasis Today.
-
May 29, 2026, 17:23Rita Schwab: Current Clinical Management of Trauma without the Use of Allogenic Blood Products
-
May 29, 2026, 17:22Brian Schiro: Excited to Provide Guideline Based Care at the Aortic Center
-
May 29, 2026, 17:20Martin Widschwendter: How Molecular Detection Tests Could Transform Endometrial Cancer Care
-
May 29, 2026, 17:18Nina Lansbury: Supporting a Period Friendly World With Menstrual Health Research and Education
-
May 29, 2026, 17:16Ipsita Chatterjee: Red is Not Shame, Red is Power, Red is a Woman
-
May 29, 2026, 16:49Abdulrahman Nasiri: The Evolving Role of Romiplostim in SAA
-
May 29, 2026, 16:46Soumen Bhattacharya: UC-II and Immune Modulation in Osteoarthritis
-
May 29, 2026, 16:38Ana Pedrero Gil: Red Blood Cell Transfusion Practice in Spain – High Inappropriateness Despite Low Overall Use
-
May 29, 2026, 15:40Lena Volland: Expanding Holistic Care in Bleeding Disorders Through Pelvic Health Physical Therapy at WFH Congress

