
Haris Mohamed: Esophageal Injury Following Capsule Manipulation in a Young Patient Receiving Dabigatran
Haris Mohamed, Inpatient Pharmacist at Abu Dhabi Stem Cells Center, shared a post on LinkedIn:
“She opened her capsule.
Mixed it with honey.
Swallowed it.
She was trying to help herself.
Three days later, she was vomiting blood.
A 19-year-old with Cerebral Venous Sinus Thrombosis – prescribed with dabigatran 150 mg twice daily.
Good diagnosis.
Correct drug.
Right dose.
But nobody told her the capsule could never be opened.
Here is what happened:
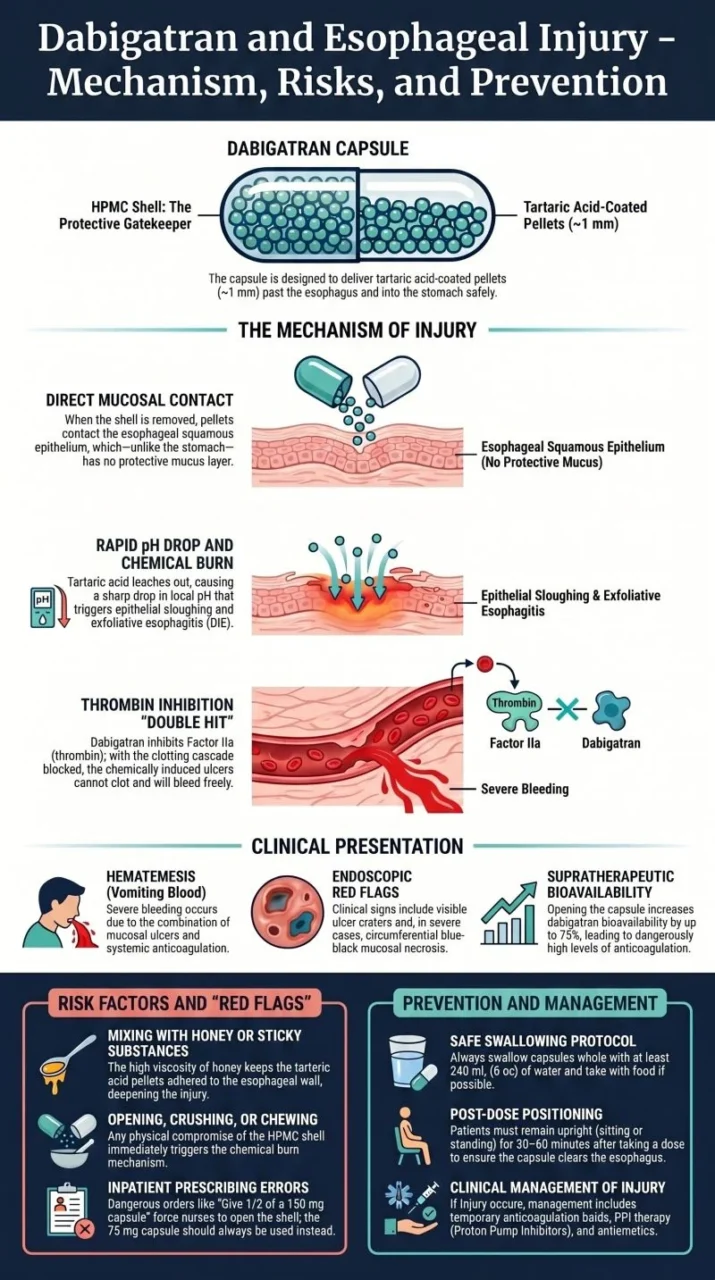
Dabigatran capsules contain tartaric acid-coated pellets.
That acid is not a filler — it creates the right environment for absorption.
The capsule shell carries those pellets safely past the Esophagus.
When she opened it, the pellets hit her Esophageal lining directly.
The pH dropped. The tissue burned.
Ulcers formed.
Then dabigatran made sure they bled freely.
Her body also absorbed 75% more drug than intended.
Maximum anticoagulation. Active bleeding.
No clotting protection.
Honey made it worse — it kept the pellets against the Esophageal wall longer.
She recovered.
But here is what stays with me:
Nobody failed dramatically.
A young woman didn’t know one rule.
And no one made sure she did.
This doesn’t only happen at home.
Pharmacists — check your inpatient orders.
Because these two orders exist in hospitals right now:
‘Dabigatran 75 mg — give ½ of a 150 mg capsule’
The 75 mg capsule is approved and available. If it is on your formulary, there is never a reason to split a 150 mg capsule.
Same order — when 75 mg is not on formulary
If the 75 mg capsule is not stocked, splitting the 150 mg is still not the answer.
Escalate to procurement, consult the prescriber — opening that capsule is never an acceptable workaround.
Both orders look like a dose adjustment.
Neither is safe.
Pellets don’t distribute evenly — ‘half’ is not half.
And a nurse handed either order will open the capsule, meaning well, causing harm.
When you see that order:
Do not dispense it
- Call the prescriber. Clarify the dose.
- 75 mg on formulary — switch to it. Document the intervention.
- 75 mg not on formulary — escalate to procurement. Never split.
- Inform nursing — this capsule is never opened
The villain is not the drug.
It is the gap between ‘prescribed correctly’ and ‘taken correctly.’
That gap lives in the skipped discharge conversation.
In the unreviewed inpatient order.
In the assumption that a young patient will figure it out.
Pharmacists sit right in that gap.
Use the position.
Never open, crush, split, or chew – ever
- Full glass of water. Every dose. With food.
- Upright for 30–60 minutes after
- Swallowing difficulty: flag it, don’t improvise
- Need 75 mg? Prescribe it — or escalate if not on formulary.
One conversation.
One intercepted order.
That is the difference.
Case details anonymized for educational purposes.”
Stay updated with Hemostasis Today.
-
May 11, 2026, 16:52Luke McLaughlin: Raising Awareness on Haemophilia Issues at ENIL Lead On
-
May 11, 2026, 16:49Jeff Sternlicht: Normal LDL Does Not Always Mean Low Risk
-
May 11, 2026, 16:42Archil Jaliashvili: From Managing Blood to Managing Oxygen Metabolism
-
May 11, 2026, 16:42Heghine Khachatryan: Celebrating One Hundred Years of von Willebrand Disease with EHC
-
May 11, 2026, 16:34Jane Hankins: Excited to Have Been a Part of the Faculty of ASH CRTI LA
-
May 11, 2026, 16:28Conan McIlwrath at the Rare Bleeding Disorders Conference Representing The Haemophilia Society as Chair
-
May 11, 2026, 16:24Anna A. Avagyan: Presenting Armenia’s Experience at SIOP Europe 2026
-
May 11, 2026, 16:18Mohamed Elkhider: Raising Awareness on Aortic Dissection
-
May 11, 2026, 16:11David McIntosh: A Pensioner’s Reflections on Blood Donation

