
Haichang Wang: The Nightmare Case on Recurrent Subacute LAD Ostial Stent Thrombosis
Haichang Wang, Hospital Director of Xi’an International Medical Center Hospital, shared a post on LinkedIn:
“Daily Cardiology Challenge 115 – Recurrent Subacute LAD Ostial Stent Thrombosis: The Nightmare Case
Case Presentation:
Patient: Male, 59 years old, emergency admission due to intermittent chest pain for 1 month, worsening over the past 3 hours.
History:
- One month ago: Started experiencing exertional, squeezing precordial chest pain. Local hospital treatment was unsatisfactory, leading to transfer. On 07-21, underwent coronary angiography and stent implantation (details unknown).
- During that hospitalization: Developed acute in-stent thrombosis 4 days later, requiring emergency coronary angiography and drug-coated balloon (DCB) angioplasty (details unknown). Symptoms resolved, and he was discharged. Outpatient regimen included Aspirin Enteric-Coated Tablets, Ticagrelor Tablets, Atorvastatin Calcium Tablets, and Ezetimibe Tablets.
- 3 hours ago: Recurrence of severe chest pain with sweating. Emergency ECG at local hospital indicated extensive anterior wall myocardial infarction.
Past Medical History:
- Hypertension: more than 8 years, highest BP 190/100 mmHg. Regular oral Nifedipine Sustained-Release Tablet 10 mg daily, BP controlled at (100-120)/(60-80) mmHg.
- Diabetes Mellitus: more than 3 months, highest blood glucose 18 mmol/L. Regular oral Metformin Hydrochloride Tablets 0.25 g twice daily and Glipizide Tablets 5 mg daily. Self-reported fasting blood glucose controlled at 6-9 mmol/L.
- Hyperlipidemia: more than 3 months. Current regimen: Atorvastatin Calcium Tablets 20 mg nightly and Ezetimibe Tablets 10 mg.
Personal History:
Smoked for more than 30 years, approximately 60 cigarettes/day. Quit smoking 8 years ago.
Examination on Admission:
Heart rate: 98 bpm, Blood pressure: 128/77 mmHg. Remainder unremarkable.
Emergency Investigations:
ECG:
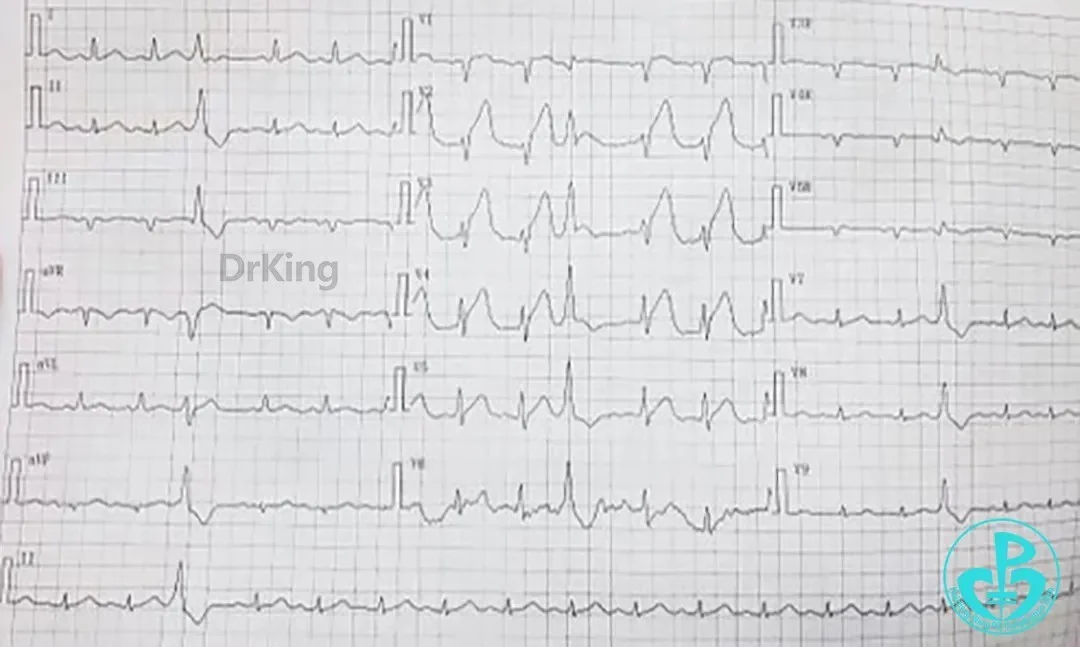
Markedly Elevated Cardiac Biomarkers:
- cTnI: 2.8 ng/ml
- Myoglobin: >900 ng/ml
- CK-MB: 72 ng/ml
- NT-proBNP: 739 ng/L
- PCT: <0.072 ng/ml
Cardiac Enzymes:
- LDH: 319 U/L
- HBDH: 267 U/L
- CK: 56 U/L
- CK-MB mass: 27 ng/ml
Coronary Angiography (Emergency, 8 days after last procedure):
Right coronary artery (RCA): Severe proximal tortuosity, mid-segment occlusion. No collateral flow to the left coronary system.
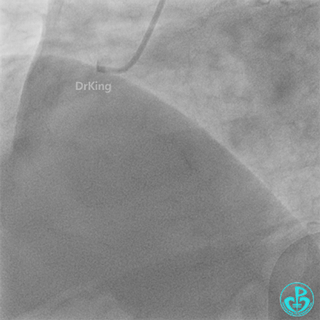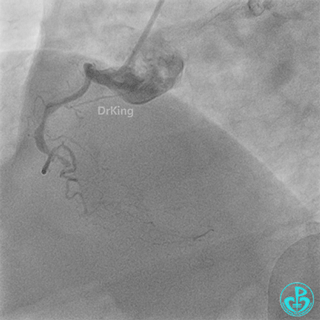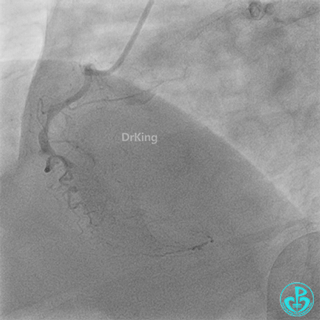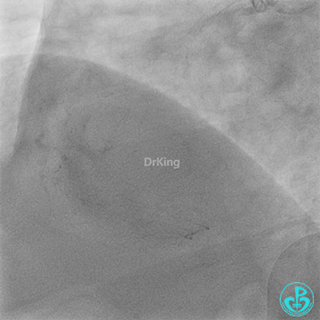
Left anterior descending artery (LAD): Stent visible from the ostium to proximal segment. In-stent occlusion at the LAD ostium.
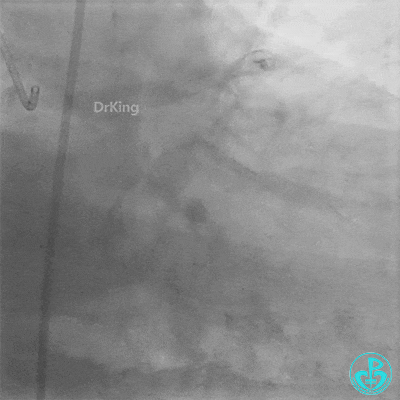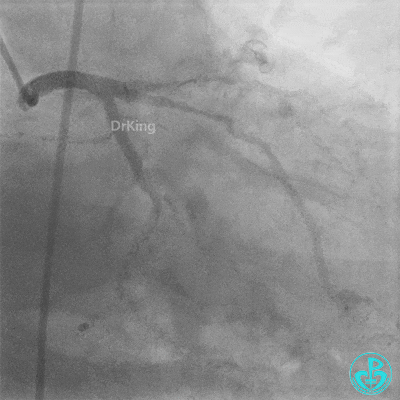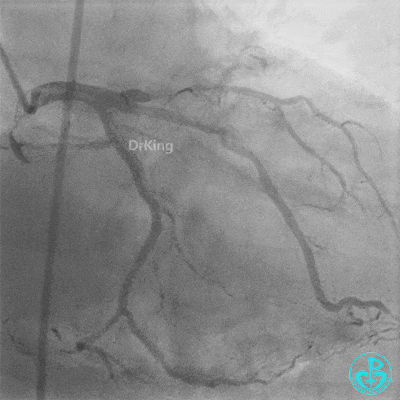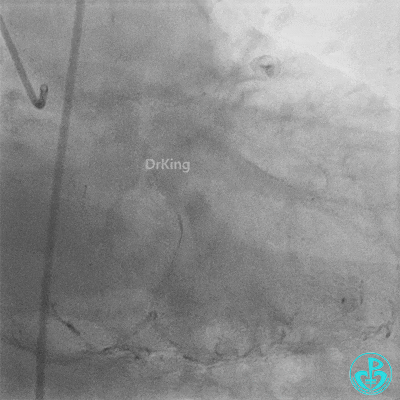
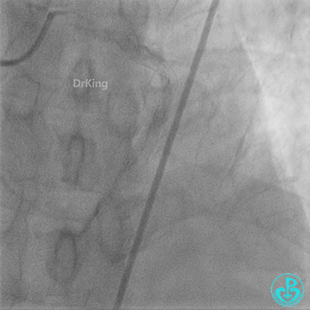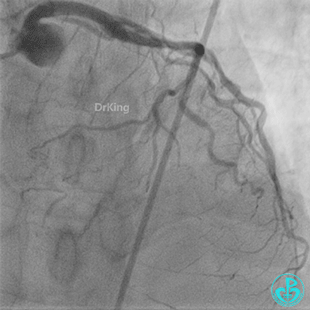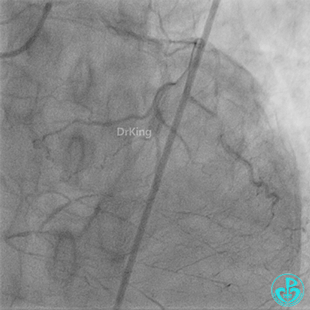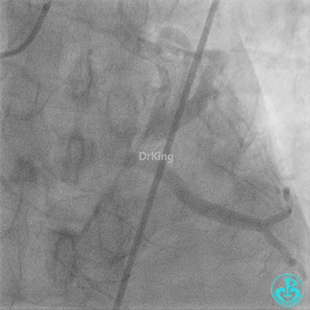
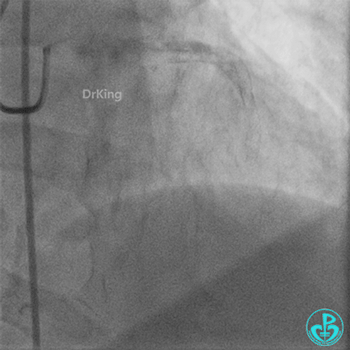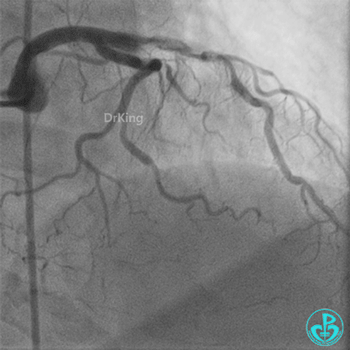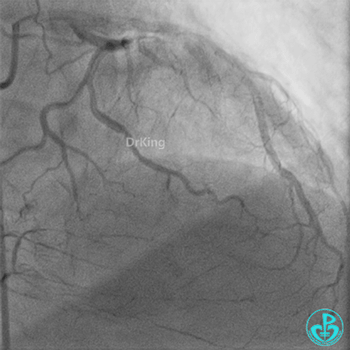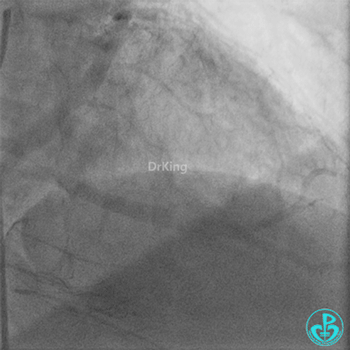
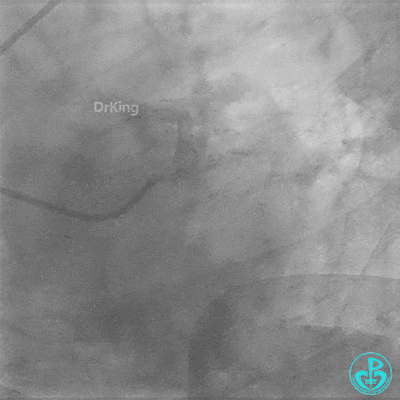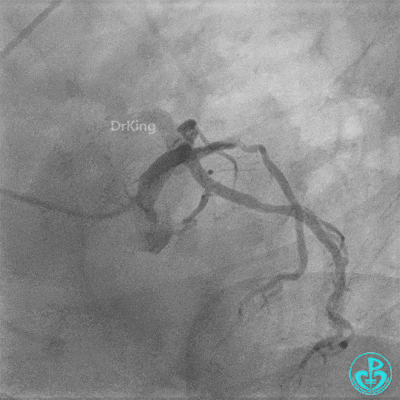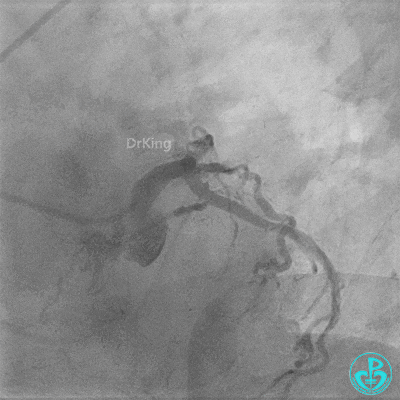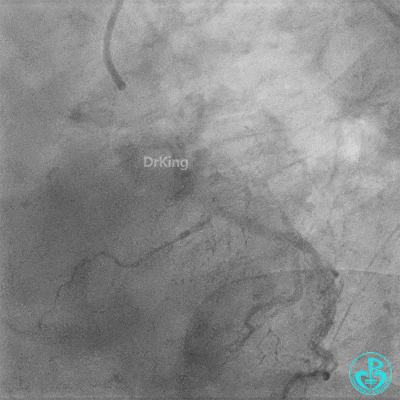
Procedure Details (First re-intervention at our center):
- Sion wire failed to cross. Fielder XT-R wire passed through the occlusion with Finecross microcatheter support, then exchanged for a Sion wire.
- Multiple dilations (5 times) performed with a 2.0×20 mm balloon and a 2.75×15 mm non-compliant balloon (14-18 atm, 5 sec each).
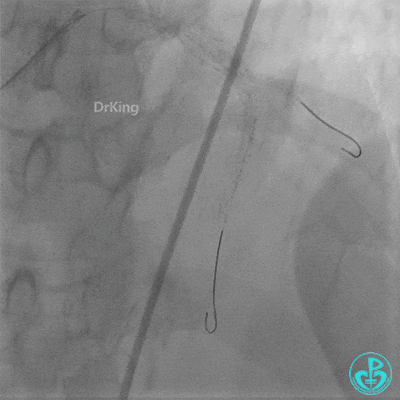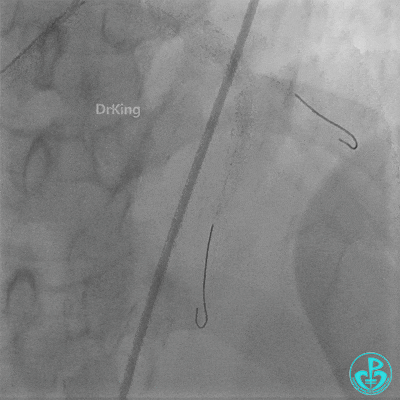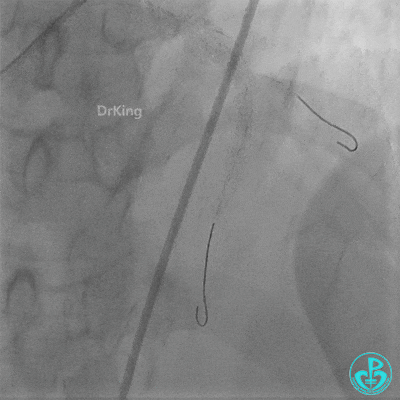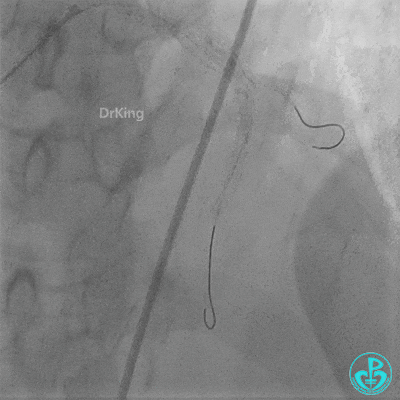
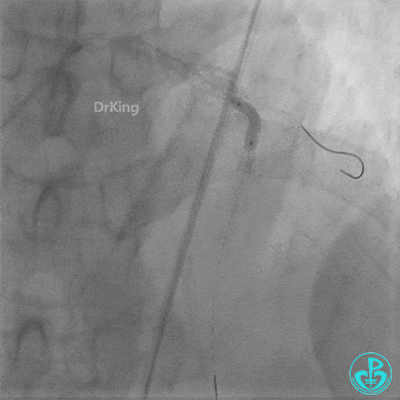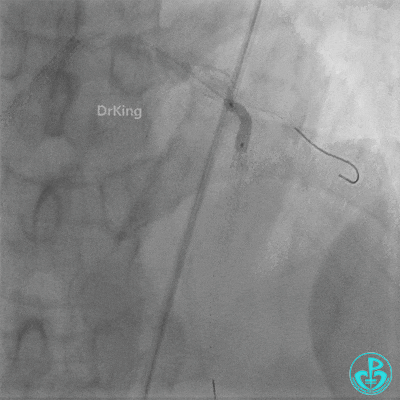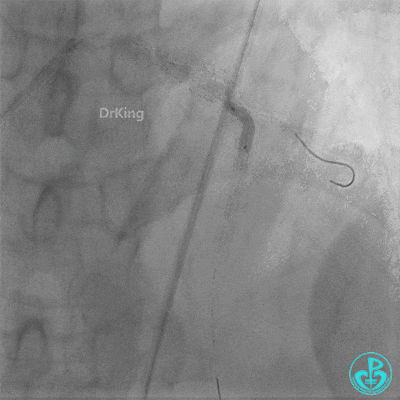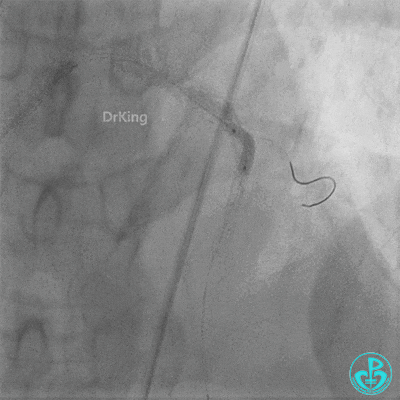
- TIMI 3 flow restored in the LAD. Residual thrombus visible within the stent.
- Thrombus aspiration catheter retrieved red thrombus.
- Intracoronary injection of 4 mg Tenecteplase (TNK).
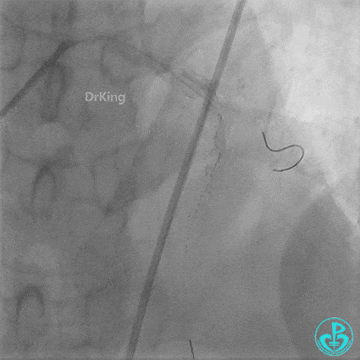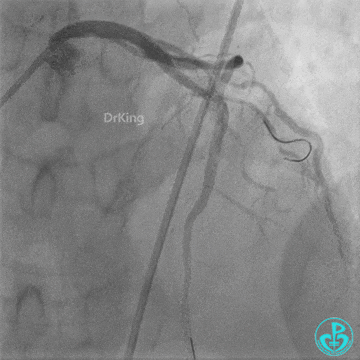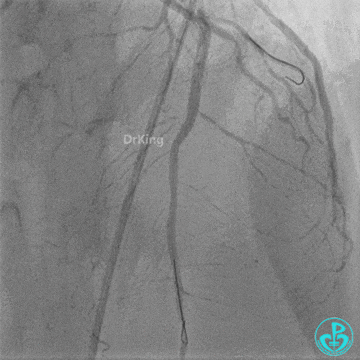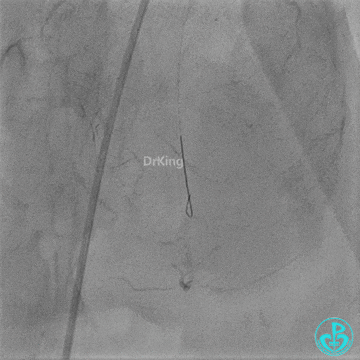
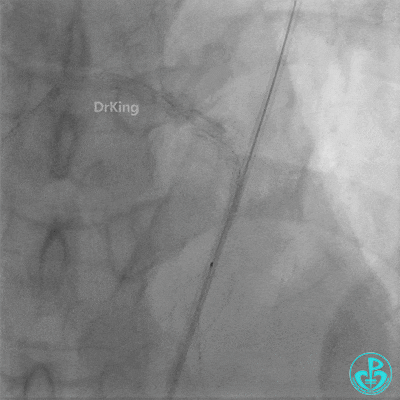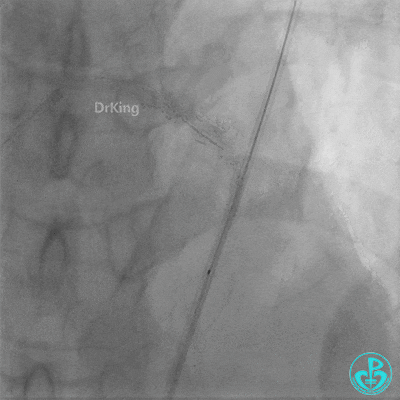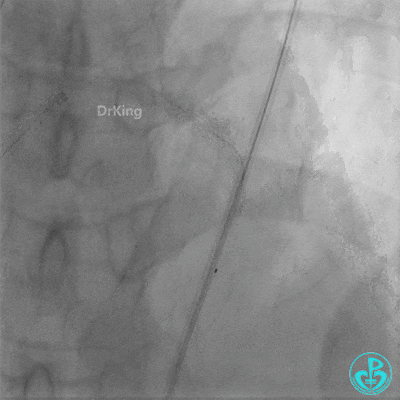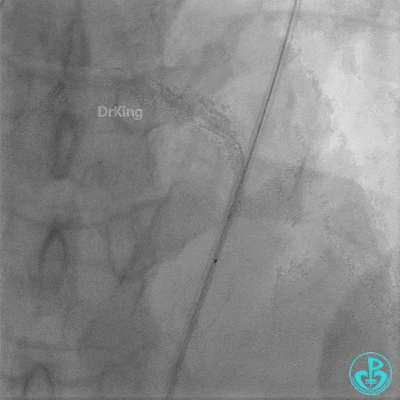
- LAD flow: TIMI 3.
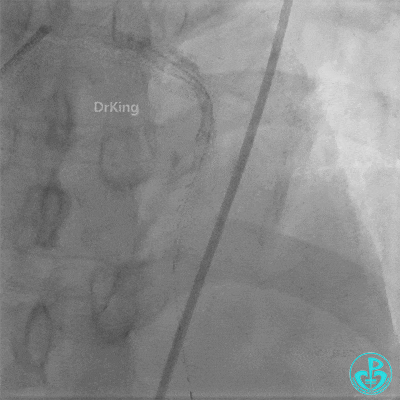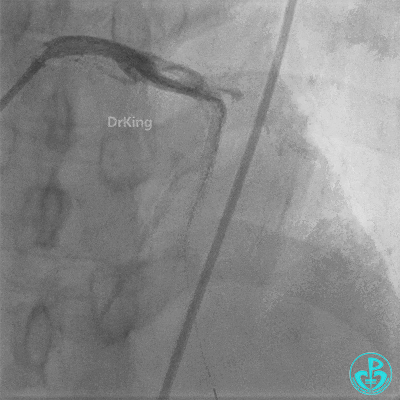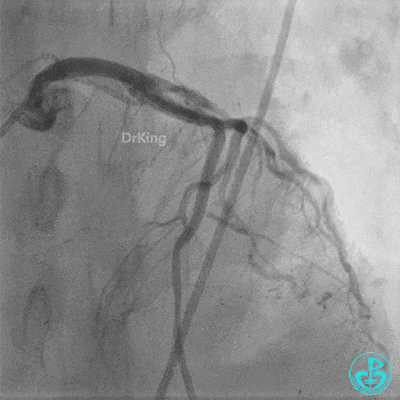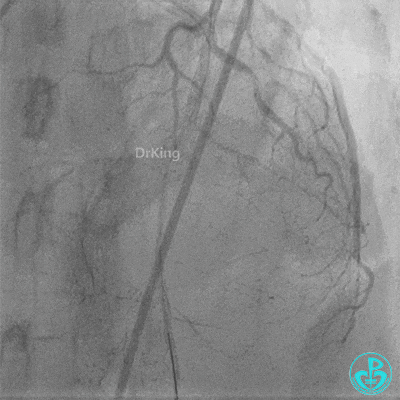
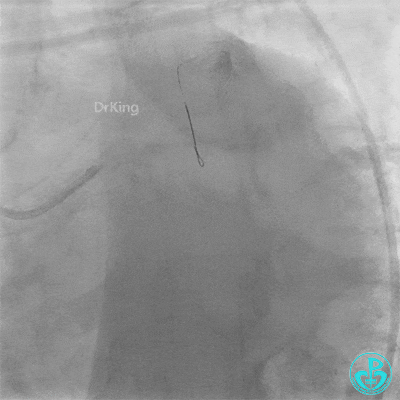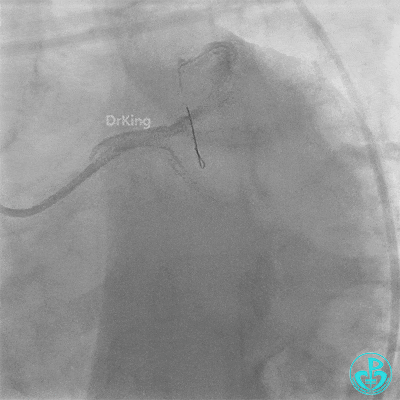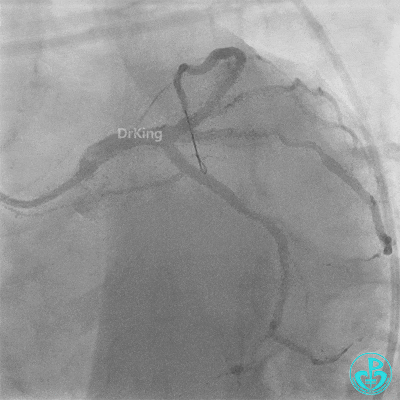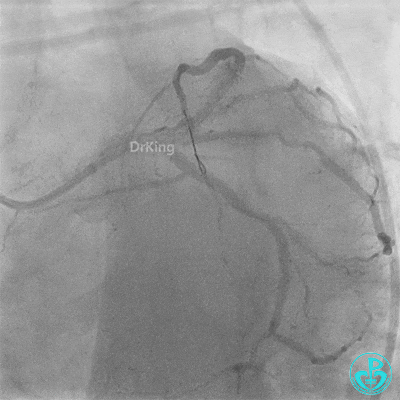
- Post-procedure: Transferred to CCU for close monitoring. Continuous Tirofiban infusion at 6 mg/hour initiated.
Post-Procedure Investigations:
- Cardiac Enzymes, Complete Blood Count:
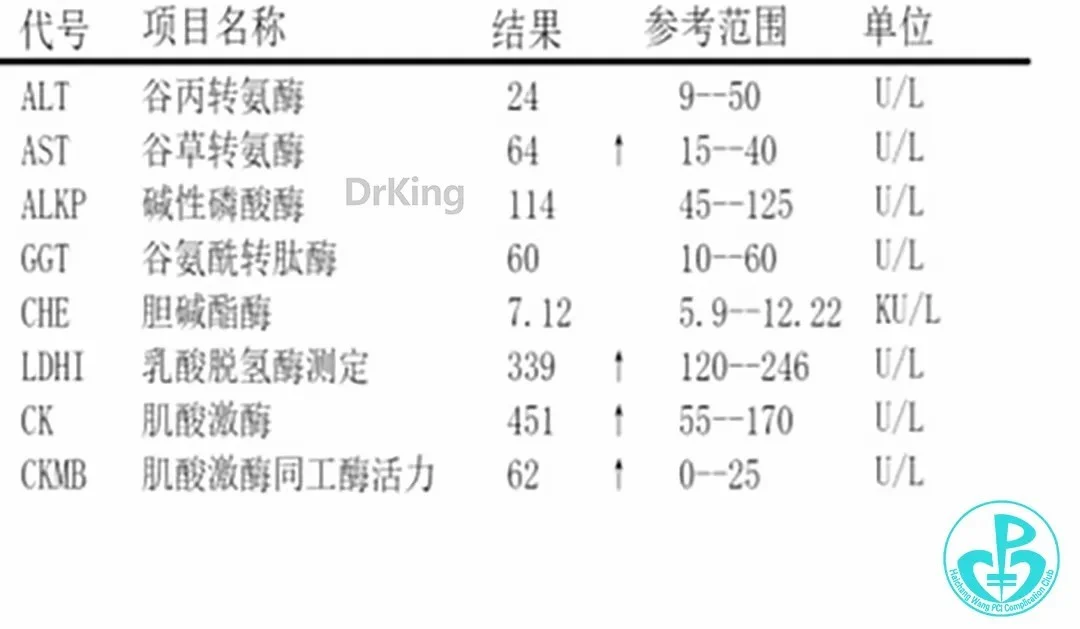
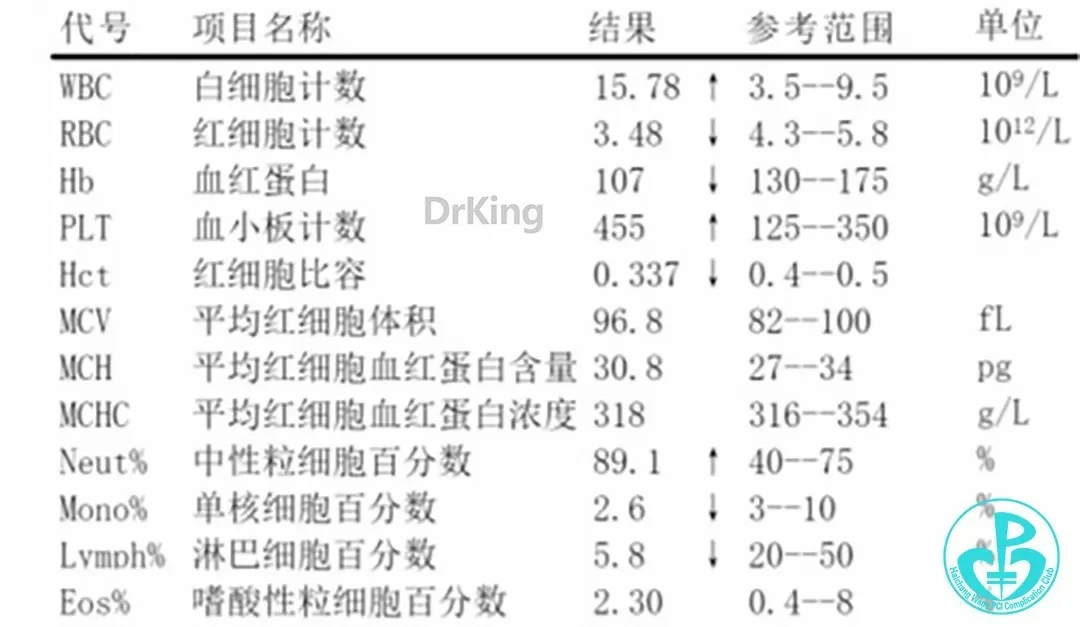

- Coagulation and Platelet Function Tests:
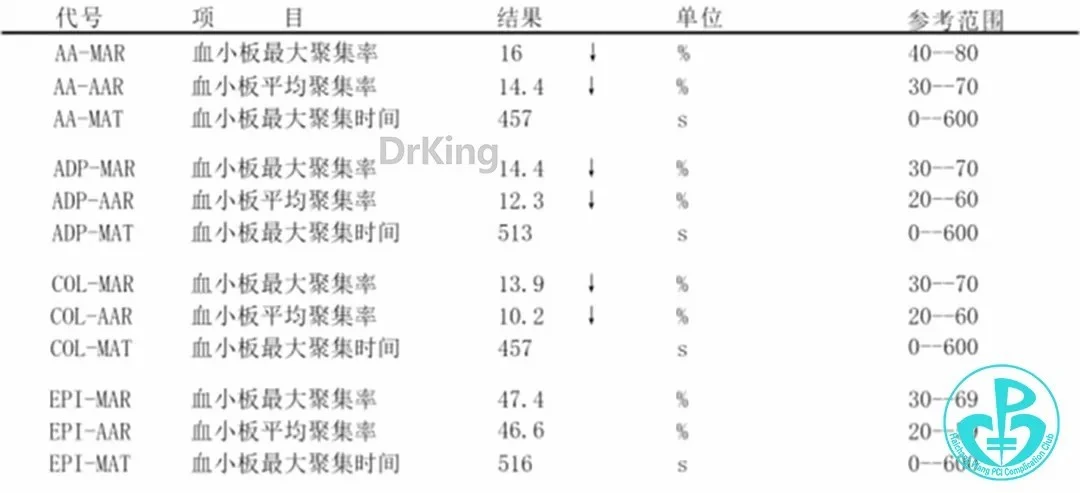
- MAR more than 55% indicates minimal drug effect; MAR less than30% indicates significant drug efficacy.
- If two or more parameters are <20%, indicates bleeding risk requiring close observation, potentially drug discontinuation or dose reduction, with repeat testing in 3-5 days.
- For drug resistance, consider dose increase and repeat test in 3-5 days.
- Note: AA: Arachidonic Acid, ADP: Adenosine Diphosphate, COL: Collagen, EPI: Epinephrine
Genotype Testing for Aspirin and Atorvastatin Metabolism:

According to the principle of assessing risk first, then efficacy, comprehensive evaluation suggests the patient can use Atorvastatin or Simvastatin for lipid-lowering therapy.
Post-Procedure Echocardiography:

ECG Post-Procedure Day 2:
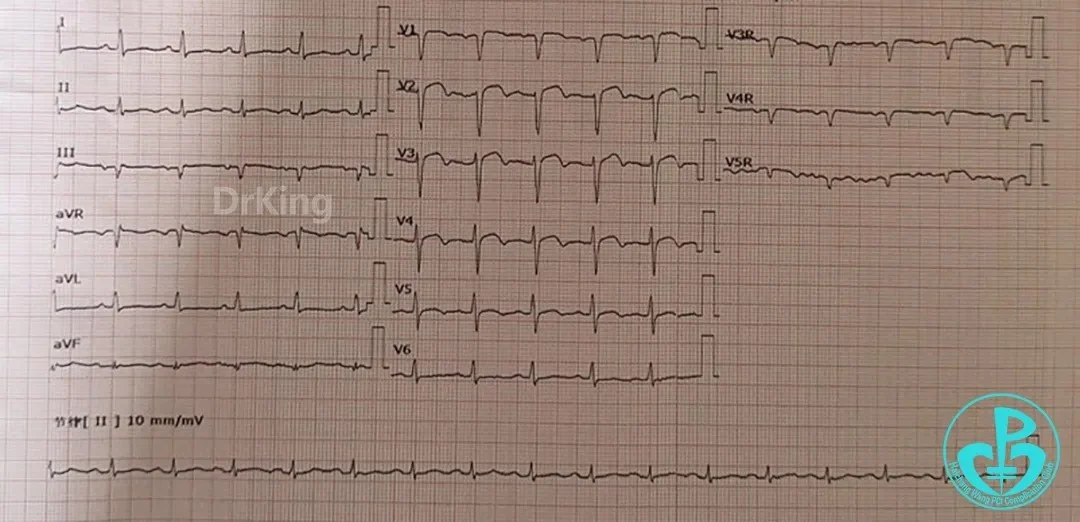
Post-Procedure Medications:
- Aspirin 100 mg once daily
- Ticagrelor Tablet 90 mg twice daily
- Atorvastatin Calcium Tablet 20 mg nightly
- Pantoprazole Sodium 40 mg once daily
- Metoprolol Sustained-Release Tablet 23.75 mg once daily
- Tirofiban 5% continuous infusion at 6 ml/hour
- Isosorbide Mononitrate Injection 20 mg once daily, diluted for IV infusion
- Symptomatic and supportive therapy
Second Re-intervention:
3 days after the last procedure, at 07:30, patient developed severe postprandial chest pain with sweating, persistent and unrelieved. ECG showed ST elevation in anterior leads.
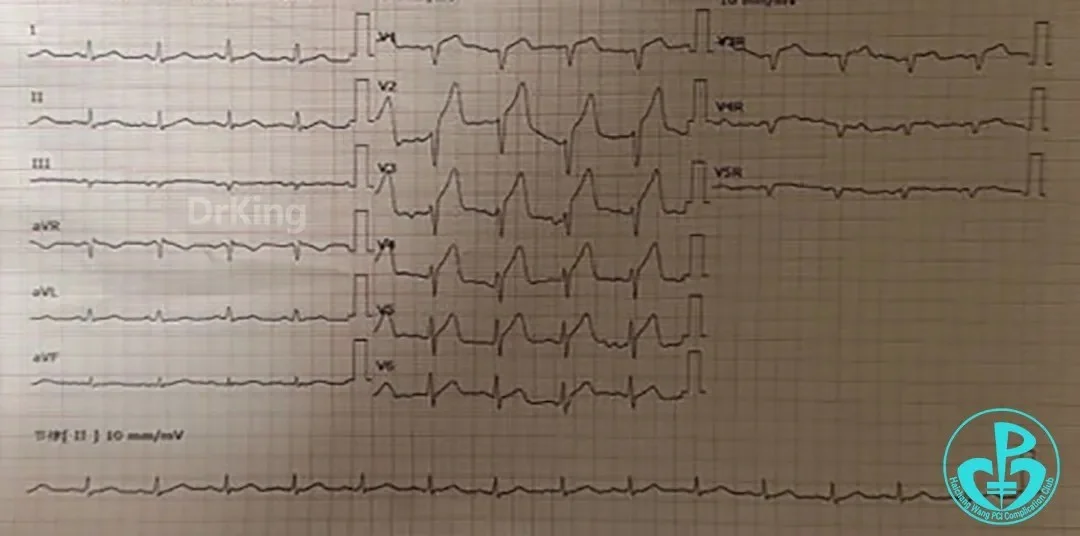
Markedly elevated troponin. Repeat ECG:
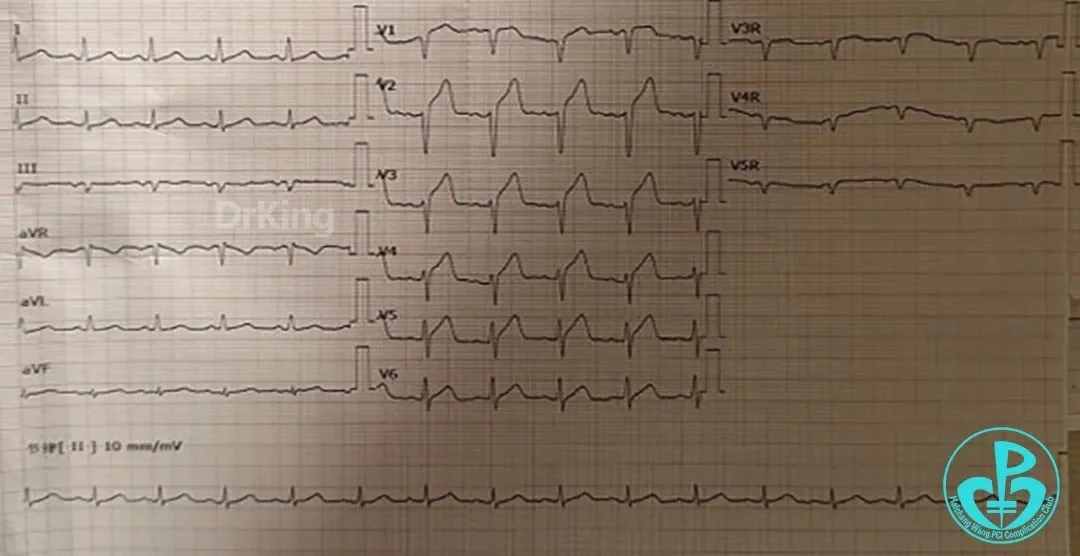
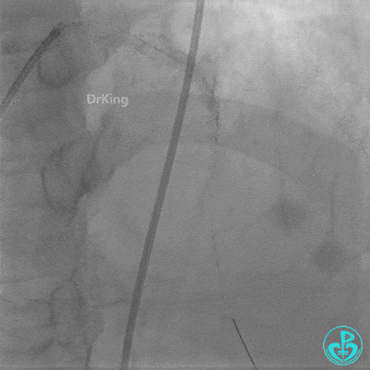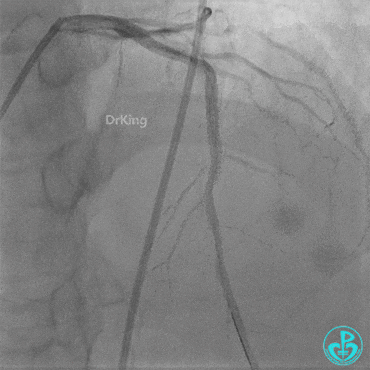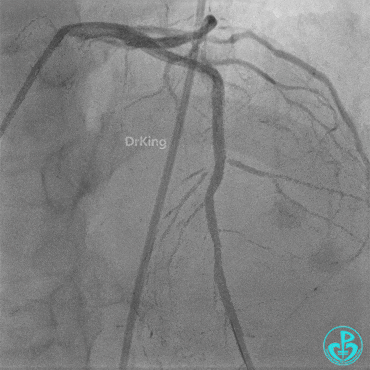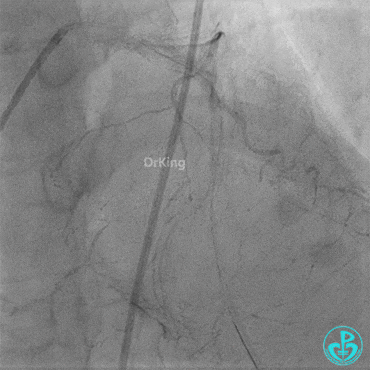
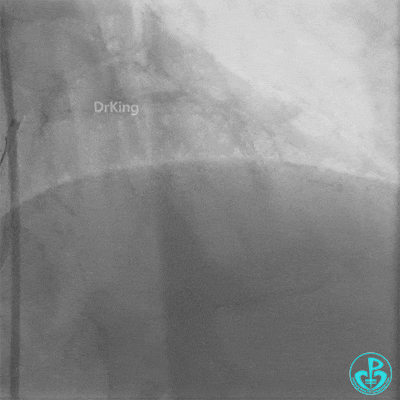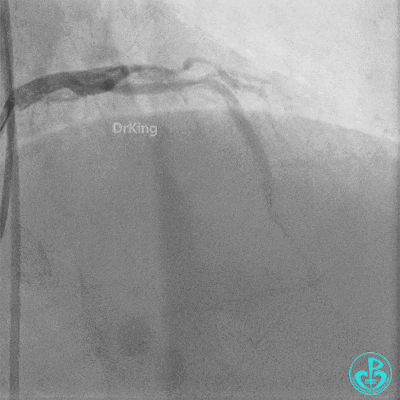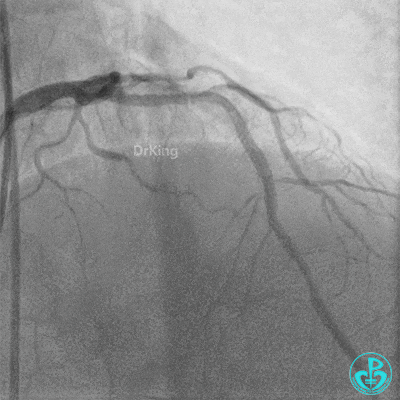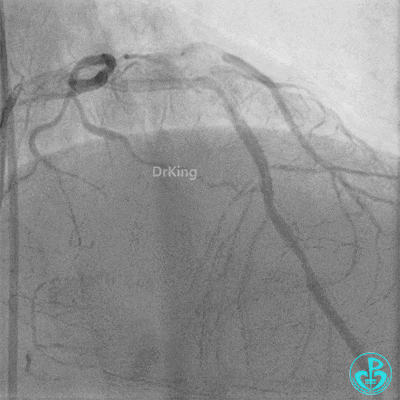
Second Emergency Coronary Angiography:
In-stent occlusion at the LAD ostium.
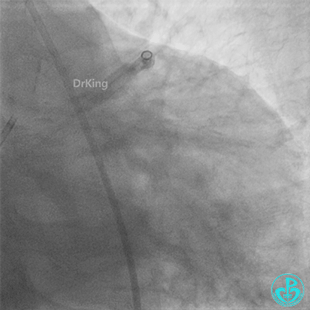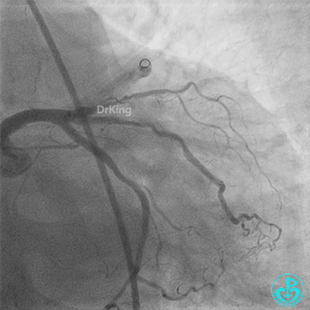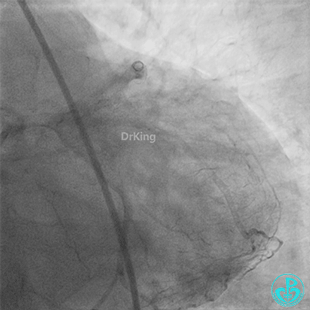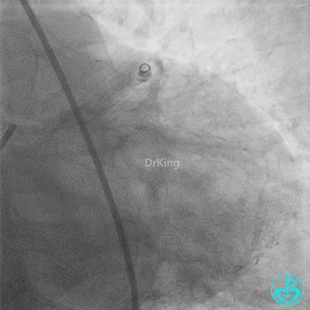
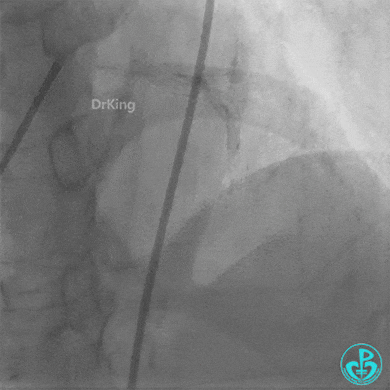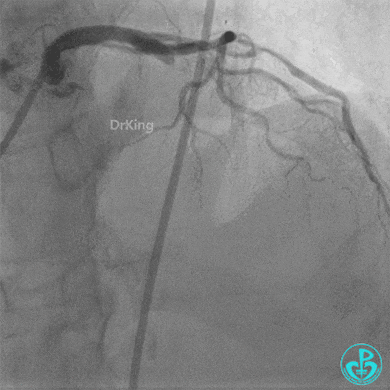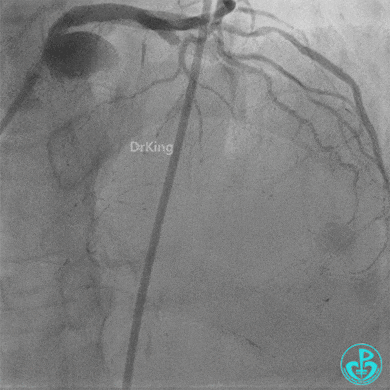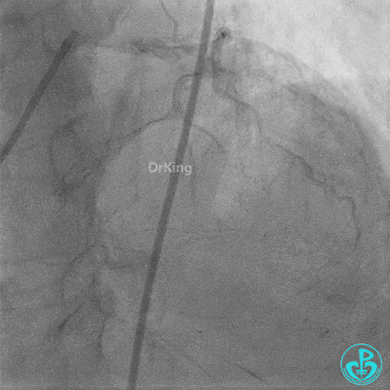
Procedure:
- 6F XB 3.0 guiding catheter engaged. Sion guidewire crossed the occlusion.
- Multiple dilations: 2.5×20 mm balloon inflated 3 times; 3.5×15 mm non-compliant balloon inflated 8 times at 14-18 atm.
- LAD flow restored to TIMI 2. Large amount of thrombus visible within the lumen.
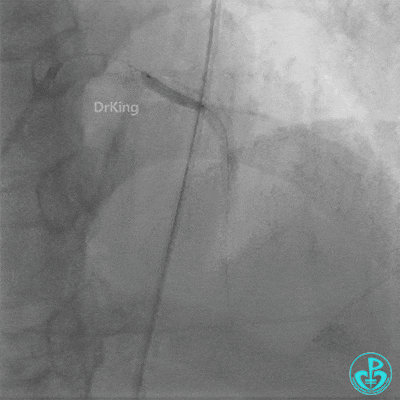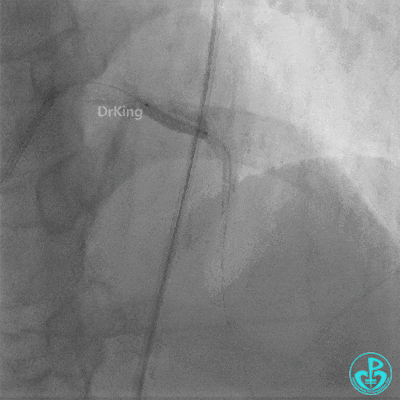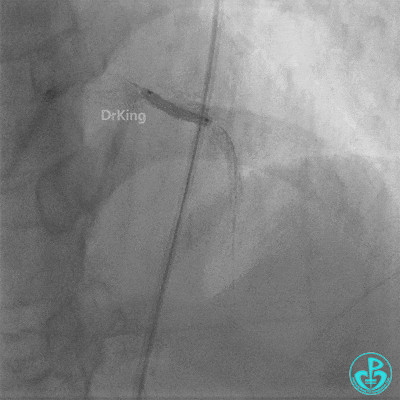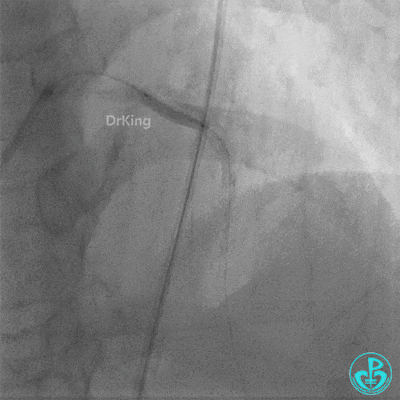
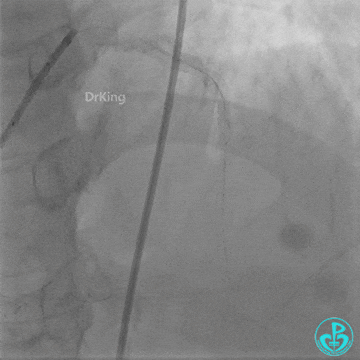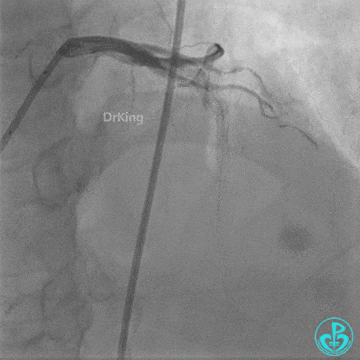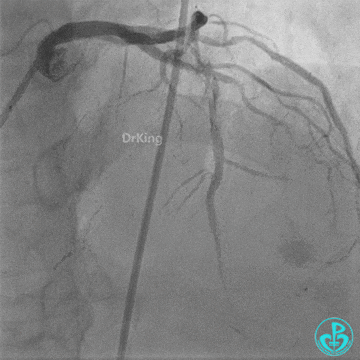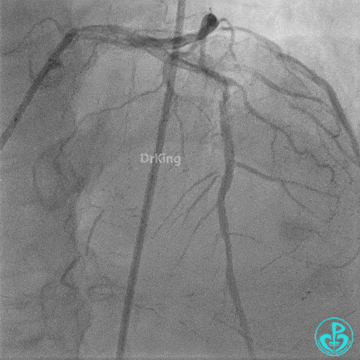
Further dilation with a 3.0 mm non-compliant balloon at 20 atm, 3 times.
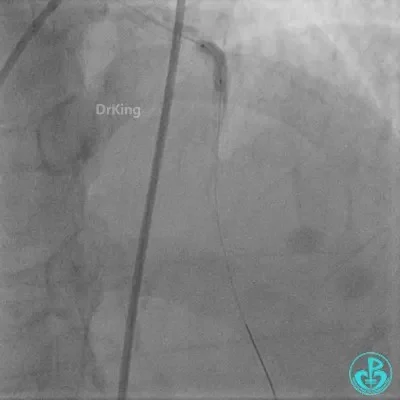
Final LAD flow: TIMI 3.
Post-Procedure Management:
Continued triple antiplatelet therapy. Tirofiban discontinued after 72 hours, switched to low molecular weight heparin for 3 days. Cardiothoracic surgery consultation obtained. Patient transferred to cardiac surgery for further management, with elective CABG planned.
Discussion Points:
- What are the possible reasons for repeated in-stent thrombosis in this patient?Stent underexpansion?Autoimmune disease?
- Was the use of a drug-coated balloon (DCB) strategy appropriate given the high thrombus burden in the initial in-stent thrombosis at the outside hospital?
- If thrombosis recurs, how should it be managed?
Follow me for more cardiology cases!”
Stay updated with Hemostasis Today.
-
May 13, 2026, 15:19Papa Heme։ Causes of Isolated Prolonged aPTT Without Bleeding
-
May 13, 2026, 15:10Wolfgang Miesbach: Rethinking Bleeding Risk in Anticoagulation
-
May 13, 2026, 15:09Veronica Sanchez: Better Cardiovascular Health Helps Lower Heart Attack Risk
-
May 13, 2026, 15:07Tung Nguyen Thanh: New Perspective on Thrombosis in Hematological Malignancies in Vietnam
-
May 13, 2026, 15:03Haji Siyamuddin Ansari: The Key Difference Between Plasma and Serum
-
May 13, 2026, 14:45Masoabi Sefojane: The Cost of a 35-Year Diagnosis Delay
-
May 13, 2026, 14:39Ahmed Mohsen: Managing DVT During Pregnancy and Lactation
-
May 13, 2026, 14:38The Coffee Shop Origins of Factor V Leiden – ISTH
-
May 13, 2026, 14:33Moustafa Abdou: Could a Commonly Prescribed Drug Trigger Life-Threatening Hemolysis?

