
Alisha Tuck: Ultrasound and Anticoagulation Management in Pregnancy – Why Anticoagulation Matters?
Alisha Tuck, Obstetrics and Gynecology Sonographer at Sonopartners, LLC, shared a post on LinkedIn:
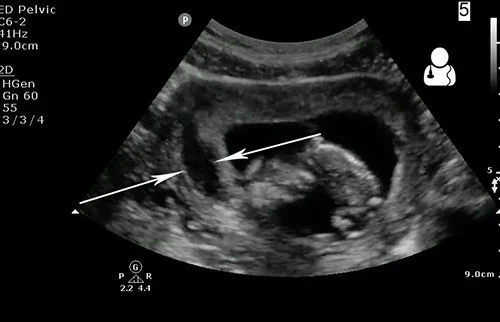
“Navigating the First Trimester: Ultrasound and Anticoagulation Management
The Physiological Context: Why Anticoagulation Matters
Pregnancy increases the risk of Venous Thromboembolism (VTE) by 4-5x .
For patients with conditions like Factor V Leiden, Protein C or S deficiency, or Antiphospholipid Syndrome (APS), the risk of pregnancy loss, placental abruption, and preeclampsia is significantly elevated.
Commonly prescribed anticoagulants in the first trimester include:
- Low-Molecular-Weight Heparin (LMWH): The gold standard (e.g., Enoxaparin) because it does not cross the placenta.
- Low-Dose Aspirin (LDA):Often used in conjunction with LMWH for APS.
- Warfarin: Generally avoided due to ‘Warfarin Embryopathy,’ though occasionally managed in patients with mechanical heart valves under strict supervision.
Key Sonographic Objectives in the First Trimester
When scanning a patient on anticoagulation, our focus shifts toward identifying early signs of pregnancy failure or maternal complications.
1. Confirming Viability and Dating
Accurate dating is paramount.
In patients with clotting disorders, placental insufficiency can manifest later; having a rock – solid CRL from the first trimester ensures that later growth restrictions are identified promptly.
2. Identifying Subchorionic Hemorrhages (SCH)
Anticoagulation therapy can increase the incidence or size of subchorionic bleeds.
- Documentation: Measure the hematoma in three planes.
- Assessment: Note the volume relative to the gestational sac. A hematoma surrounding more than 50% of the sac carries a higher risk of pregnancy loss.
- Clinical Impact: Your report may lead the physician to ‘hold’ or adjust the dosage of anticoagulants.
3. Corpus Luteum and Adnexal Evaluation
Check for large corpus luteum cysts or evidence of internal hemorrhage.
While common, anticoagulated patients are at a slightly higher risk for hemorrhagic cysts, which can mimic ectopic pregnancy symptoms (pelvic pain).
Summary Checklist for the Sonographer
- Gestational Sac – Location, Shape, Mean Sac Diameter. Rule out ectopic; assess for ‘low implantation’
- Yolk Sac – Presence and Diameter. Early indicator of pregnancy health
- CRL – Best measurement of 3 | Critical for future growth monitoring
- Hematoma – Size (cm), Location, % of sac perimeter. Guides anticoagulant dosing adjustments
- Adnexa – Ovaries, free fluid, or masses. Rule out hemorrhage or secondary complications
Conclusion
Sonographers play a pivotal role in the multidisciplinary care of the high – risk obstetric patient.
By providing meticulous documentation of the early pregnancy and any associated perigestational bleeding, we allow the clinical team to tailor anticoagulation therapy – optimizing the safety of both the mother and the developing embryo.”
Stay updated with Hemostasis Today.
-
May 31, 2026, 09:49Ermias Solomon Yalew: New Insights Into Multimorbidity and Disability After Stroke from Ethiopia
-
May 31, 2026, 07:02Raising Awareness of Cerebral Venous Sinus Thrombosis in Women – NBCA
-
May 31, 2026, 07:00Ceri Roberts: How to Reduce Your Risk of a Blood Clot
-
May 31, 2026, 05:28Nikolaos Androulakis: Inflammatory Burden and Antiphospholipid Antibodies in Lupus Anticoagulant Testing
-
May 31, 2026, 05:28Alysha Arif: Understanding a Complex Case of Postpartum Seizures
-
May 31, 2026, 05:27Chiara Novelli: Are We Validating Laboratory Algorithms as Rigorously as We Validate Laboratory Tests?
-
May 31, 2026, 02:42Katja van den Hurk: Optimizing Iron Management in Blood Donors
-
May 31, 2026, 02:36The New JPAC Website Has Been Live for Nearly a Week – SHOT
-
May 31, 2026, 02:33Jecko Thachil: Is It Possible to Use Machine Learning for Differentiating Inherited Thrombocytopenia from Other Causes?

