
Jeff June: Building the Biological Map for Stroke Neuroprotection
Jeff June, Innovation and Ecosystem Leader at University Lab Partners, MedTech Innovator, Founding CEO and Board Member at Ischemia Care, shared on LinkedIn:
”Stroke research is full of complex mechanisms and promising molecules.
Neuroprotection in stroke isn’t failing.
It’s often being tested without a biological map — treated as one-size-fits-all rather than aligned to underlying biology.
In the reperfusion era, understanding which patients express which biology may matter more than the next new molecule.
Reperfusion changed stroke care.
Thrombectomy works.
Door-to-needle times matter.
Large vessel occlusions can now be reopened with precision that would have been unimaginable two decades ago.
But reopening an artery is not the same as restoring a brain.
The reperfusion era has made something clear:
We are procedurally advanced. We are still biologically early.
A recent Science Advances paper described nanoparticles that anchor to inflamed cerebral vessels and locally generate hydrogen (H₂), allowing it to diffuse across the blood–brain barrier and modulate post-stroke inflammation.
In murine models, the therapy:
- Reduced infarct size
- Shifted microglia toward a reparative phenotype
- Enhanced angiogenesis and axonal sprouting
- Improved long-term motor recovery
- Outperformed edaravone across several measures
The work is thoughtful. The inflammatory–microglial axis is clearly modifiable.
But the deeper issue isn’t the molecule.
It’s the map.
Many neuroprotective strategies show strong biological effects in preclinical models.
Yet translating those effects into consistent benefit across broad stroke populations has been difficult.
One reason may be how we enroll.
Most stroke trials stratify based on:
- Time from onset
- Imaging findings
- Vessel status
Very few stratify based on:
- Inflammatory burden
- Immune activation gradients
- Oxidative stress dominance
- Reparative pathway suppression
Yet this hydrogen-based strategy works by shifting post-ischemic inflammation and microglial behavior.
If only a subset of patients express that biology at scale, enrolling everyone dilutes measurable effect.
Signal doesn’t vanish. It gets averaged.
Reperfusion fixed the plumbing.
Now we need to understand the tissue.
Not all ischemic strokes share the same downstream biology:
- Some are thrombosis-dominant
- Some are cardioembolic with limited inflammatory amplification
- Some are immune-amplified and repair-suppressed
- Some retain strong endogenous recovery programs
A therapy designed to modulate microglia or oxidative stress is unlikely to be uniformly effective across these contexts.
This is where a biological map becomes essential.
Large multi-center transcriptomic efforts, including clinical trials like BASE (NCT02014896), demonstrate that peripheral immune gene expression differs by stroke subtype and mechanism.
These datasets allow quantification of inflammatory activation and modeling of reparative pathway activity early after stroke.
That changes the framing.
Instead of asking, ‘Does this therapy work in stroke?’
We can ask, ‘In which biological subtype of stroke does this mechanism have leverage?’
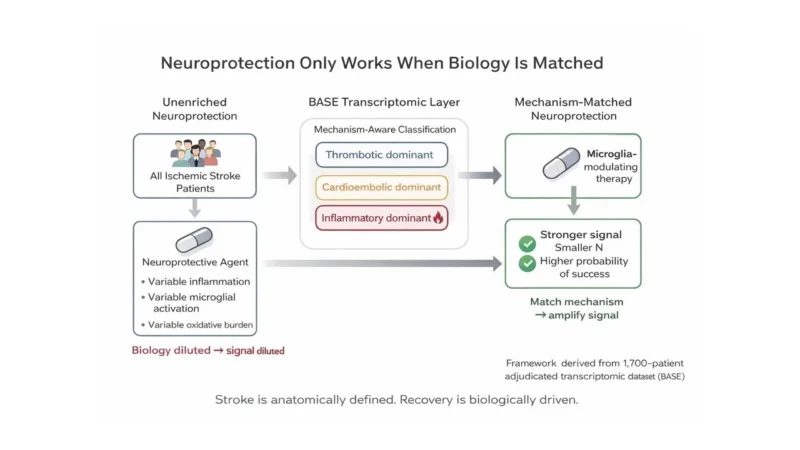
A practical model for the reperfusion era looks like this:
- Start with the full ischemic stroke population
- Apply a biological stratification layer
- Enroll patients whose biology aligns with the therapy’s mechanism
Without that middle layer, trials test molecules against heterogeneity.
With it, trials test mechanisms against biology.
Reperfusion restored blood flow.
The next frontier is biological alignment.
Stroke is anatomically defined. Recovery is biologically driven.
If neuroprotective strategies are to reach their potential in the reperfusion era, the path forward is not simply a new molecule.
It is enrichment.
Build the map. Use it. Then randomize.”
Stay updated with Hemostasis Today.
-
Jun 1, 2026, 13:44Milad Abdalla: Elevating Phlebotomy Standards – Why Order of Draw and Blood Cultures Matter
-
Jun 1, 2026, 13:39Abdul Mannan: The Moral Injury of Practising Haemato-Oncology in a Resource-Limited Setting
-
Jun 1, 2026, 13:34Filza Aslam: What Does a Patient Journey Partner Actually Do in Bleeding Disorders?
-
Jun 1, 2026, 13:33Darine Ghanem: Advancing Health Equity in Care at the LATAM Meeting
-
Jun 1, 2026, 13:23Skye Collado: Miller-Keystone Blood Center Expands Community Impact Through the Addition of New Bloodmobiles
-
Jun 1, 2026, 12:37Rutuja Mahadik: Anemia is More Than Just Feeling Tired
-
Jun 1, 2026, 12:36Ankur Jindal: Large-Vessel Inflammation and Immune Dysregulation in Wiskott–Aldrich Syndrome
-
Jun 1, 2026, 12:35Shadi Almassri: Conditions That Can Cause False High or False Low HbA1c Results
-
Jun 1, 2026, 12:22Ed Davidson: Clot Removing Technology That Can Change the Game

