
Reza Shojaei: EU’s Critical Medicines Act and Plasma Resilience
Reza Shojaei, Chief Operating Officer at Canadian Plasma Resources, shared a post on Linkedln:
”Medicine shortages are no longer viewed as isolated disruptions; they are now treated as structural vulnerabilities.
With the EU’s Critical Medicines Act (CMA) advancing, the policy conversation has shifted from reactive shortage management to strategic resilience.
But what does this mean for plasma-derived therapies, one of the most supply-sensitive and globally integrated categories of essential medicines?
For plasma leaders, this is not just regulatory reform.
It touches on manufacturing sovereignty, coordinated stockpiling, cross-border dependency, and long-term supply stability.
Poorly aligned national stockpiling could distort markets and intensify shortages.
Well-harmonized frameworks could strengthen continental resilience and encourage investment in fractionation.
In this edition of Blood and Plasma Pulse, we examine how the CMA may reshape plasma supply dynamics and why inventory policy must reflect the biological and operational realities of plasma-derived medicines.
I invite healthcare leaders, regulators, and plasma professionals to read and share your perspective:
How should Europe balance sovereignty with system optimization in plasma supply?
Introduction: From Collection to Strategic Sovereignty
The Critical Medicines Act (CMA) is a legislative initiative proposed by the European Commission as part of its broader Pharmaceutical Strategy for Europe.
Emerging from lessons learned during the COVID-19 pandemic and repeated medicine shortages across Member States, the CMA aims to strengthen the security of supply for medicines considered vital to public health and health system resilience.
The Act builds on earlier EU regulatory coordination mechanisms and seeks to introduce structured tools such as coordinated stockpiling, strategic investment in manufacturing capacity, and improved cross-border monitoring of supply risks (European Commission, 2023a; European Commission, 2023b).
Its development reflects a shift from reactive shortage management toward proactive system-level resilience planning.
In the plasma community, ‘self-sufficiency’ has traditionally focused on donor recruitment and plasma collection volumes.
Today, the conversation is broader and more structured.
In the European Union, the proposed Critical Medicines Act (CMA) signals a shift toward policy mechanisms that extend beyond collection to include manufacturing sovereignty, coordinated stockpiling, and mitigation of cross-border supply dependencies.
Plasma-derived medicinal products (PDMPs), including immunoglobulins, albumin, and coagulation factors, are widely recognized as life-sustaining therapies for patients with primary immunodeficiencies, autoimmune diseases, trauma, and rare bleeding disorders (European Medicines Agency [EMA], 2023).
Their biological complexity, long manufacturing timelines, and reliance on global plasma supply chains position them squarely within the ‘critical medicines’ category.
As Europe advances CMA implementation, stockpiling frameworks and regulatory harmonization will materially influence Europe’s resilience of plasma protein supply.
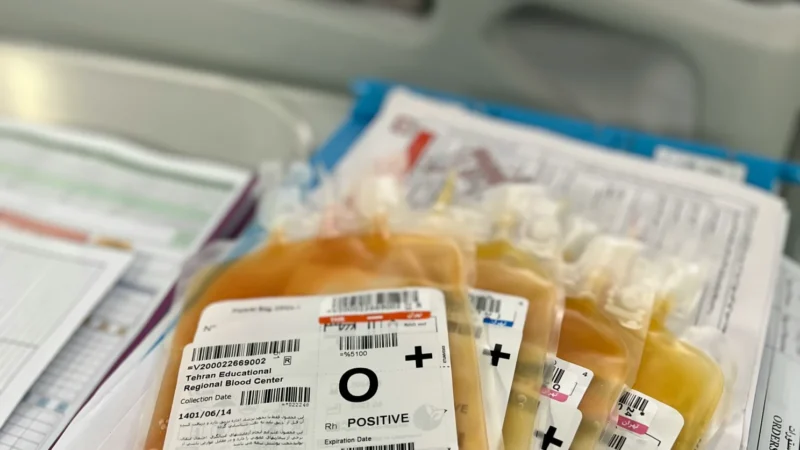
For plasma-derived therapies, resilience is not only about donor collection but also about manufacturing capacity, inventory governance, and cross-border supply optimization to prevent shortages and protect patients.
Why Plasma-Derived Therapies Are Systemically Sensitive
Plasma fractionation is inherently global. P
lasma collected in one country is often processed in another, with PDMPs then redistributed across multiple jurisdictions.
This cross-border integration has historically improved efficiency and optimized capacity.
However, it also introduces structural interdependence.
The COVID-19 pandemic exposed vulnerabilities in the plasma supply. Lockdowns and reduced donor attendance led to substantial declines in global plasma collection, particularly in the United States, which supplies a majority of the world’s plasma for fractionation (PPTA, 2022).
The downstream effect was prolonged immunoglobulin shortages across parts of Europe and other regions, illustrating how geographically concentrated collection can reverberate across borders.
The European Commission has acknowledged these vulnerabilities in its broader pharmaceutical reform agenda, emphasizing the need to secure supply chains for critical medicines (European Commission, 2023a).
PDMPs, given their manufacturing lead times (6–12 months or longer), are particularly sensitive to upstream disruption.
Stockpiling: Risk Mitigation or Market Distortion?
Stockpiling is frequently positioned as a resilience strategy.
Yet its impact depends entirely on design and coordination.
Fragmented National Stockpiling
If implemented independently by individual Member States, national stockpiling programs can have unintended consequences:
- Market distortion: Sudden national procurement surges may concentrate supply in certain regions.
- Internal shortages: Smaller countries with lower purchasing power may experience constrained access.
- Inefficient inventory rotation: Given PDMP shelf-life limitations, buffer stock duplication can reduce overall system efficiency.
The EMA has previously highlighted how supply disruptions in critical medicines often stem not from single-point failures, but from system-level imbalances exacerbated by parallel demand spikes (EMA, 2023).
In plasma markets, where ramp-up capacity cannot be rapidly expanded, poorly coordinated stockpiling could intensify volatility rather than alleviate it.
Harmonized and Coordinated Approaches
Conversely, stockpiling frameworks aligned at the EU level could strengthen resilience.
A harmonized CMA-driven mechanism may:
- Align buffer volumes with actual epidemiological demand modelling
- Reduce redundant procurement competition
- Maintain transparent visibility across Member States
The European Commission’s communication on strengthening pharmaceutical supply chains stresses coordinated EU-level action over unilateral national measures (European Commission, 2023b).
For plasma-derived medicines, such coordination is essential given constraints on fractionation capacity and the long plasma-to-product cycle.
Manufacturing Sovereignty and Fractionation Capacity
Self-sufficiency is increasingly framed not merely as collection self-reliance but as manufacturing sovereignty.
Europe historically imports significant quantities of source plasma for fractionation and finished PDMPs derived from U.S. collections (PPTA, 2022).
Expanding European fractionation capacity and encouraging domestic plasma collection could reduce dependence on geopolitical risk or trade policy shifts.
However, manufacturing sovereignty must balance economic realities.
Fractionation facilities require multiyear capital investment, robust regulatory oversight, and a sustained supply of plasma input.
The CMA’s investment-aligned incentives, if designed with plasma in scope, could catalyze strategic infrastructure expansion while preserving global supply integration.
The key is proportionality: ensuring resilience without fragmenting a highly optimized international system.

Hospital pharmacy shelves stocked with critical medications highlighting why coordinated stockpiling under the EU Critical Medicinces Act must balance resilience with market stability.
Cross-Border Dependency: Inevitable but Manageable
Plasma is a quintessential example of beneficial interdependence. Global pooling enhances epidemiological diversity and mitigates risk concentration.
Absolute autarky is neither feasible nor economically rational.
Therefore, the policy challenge under the CMA is not to eliminate cross-border dependency but to manage it transparently and strategically.
The European Commission has emphasized early notification of shortages and coordinated procurement planning as tools to enhance resilience (European Commission, 2023a).
For PDMPs, such transparency could prevent demand-driven shocks and optimize fractionation scheduling.
If CMA implementation integrates plasma-specific realities, including yield constraints, demand growth trajectories, and fractionation lead times, it can reinforce continental security rather than inadvertently constrain supply flexibility.
What This Means for Plasma Leaders
For professionals operating within plasma collection, fractionation, or policy, the CMA represents more than legislative reform.
It is a structural shift in how ‘criticality’ is defined and operationalized.
Three strategic considerations emerge:
- Engagement in Policy Development: Plasma stakeholders must ensure that stockpiling models reflect PDMP production cycles and therapeutic substitution limitations.
- Investment in Data Transparency: Accurate demand forecasting and capacity visibility will be central to effective continental coordination.
- Balanced Advocacy: Support resilience-building without endorsing fragmentation that could destabilize protein markets.
Plasma-derived therapies already function as critical infrastructure in healthcare systems.
The next phase is aligning regulatory frameworks to safeguard that infrastructure.
Critical medications under the EU framework, where policy meets patient care. As the Critical Medications Act (CMA) advances, harmonized stockpiling and coordinated manufacturing strategies will be essential to safeguard plasma-derived therapies.
A Defining Moment for System-Level Resilience
The EU Critical Medicines Act (CMA) has the potential to strengthen Europe’s therapeutic sovereignty, but only if implemented with a nuanced understanding of biologics, such as plasma-derived medicines.
Self-sufficiency today is multidimensional: collection capacity, manufacturing strength, coordinated inventory, and regulatory cohesion.
Fragmented stockpiling could distort markets and undermine continental optimization.
Harmonized frameworks, however, could attract investment, stabilize supply, and protect patients during geopolitical or epidemiological shocks.
For leaders across the plasma ecosystem, the message is clear: resilience is no longer just operational, it is strategic.
References
- European Commission. (2023a). Proposal for a regulation laying down measures to strengthen security of supply of critical medicines in the European Union.
- European Commission. (2023b). A pharmaceutical strategy for Europe – Ensuring access to affordable medicines and supporting innovation.
- European Medicines Agency. (2023). Medicine shortages in the EU – root causes and mitigation strategies.
- Plasma Protein Therapeutics Association. (2022). Plasma supply and demand overview.”
Stay updated with Hemostasis Today.
-
May 28, 2026, 05:29Kidist K.: First Balloon Pulmonary Angioplasty Performed as New CTEPH Program Launches
-
May 28, 2026, 04:59Maria Sol Andres: Exploring Lipid Disorders in Modern Cancer Care
-
May 28, 2026, 04:42Francesca Granata: Representing the Porphyria Community at the 79th World Health Assembly
-
May 28, 2026, 04:29Samone Cook: When Collaboration Turns Into Organizational Coagulation
-
May 28, 2026, 03:42Lara Bloom: 15,000 Steps, Countless Conversations – One Unforgettable WHA79
-
May 27, 2026, 23:00Octavio Marques Pontes-Neto: Exchanging Latin American Experiences at the Global Stroke Alliance Meeting in Buenos Aires
-
May 27, 2026, 17:51Nita Radhakrishnan: Post Graduate Institute of Child Health Receives WFH Data Quality Certification for Excellence
-
May 27, 2026, 17:51Fiona Robinson: What exactly Are Rebalancing Agents for Bleeding Aisorders?
-
May 27, 2026, 17:14Khurram Nasir: Can Earlier LDL-C Lowering Change the Trajectory of Cardiovascular Disease?

