Sumyea Kabir: The Hidden Risk of Bombay Blood Group
Sumyea Kabir, Assistant Professor at Zainul Haque Sikder Women’s Medical College and Hospital, shared a post on LinkedIn:
”Bombay Blood Group (Oh): When ‘O’ Is Not O
A rare phenotype. A common mistake. A potentially fatal outcome.
During my residency at Bangladesh Medical University, I encountered 5 confirmed cases of Bombay blood group (Oh)—a powerful reminder that assumptions in blood grouping can cost lives.
The Dangerous Assumption:
- Appears as O group on forward typing
- considered universally compatible
O blood transfusion can cause acute hemolytic reaction
Apparent O is not equal to Safe O
Why named as ‘Bombay’ Blood Group?:
- First reported in 1952 in Bombay (Mumbai), India
- Discovery led to identification of absence of H antigen
- A landmark chapter in immunohematology—still clinically relevant today
What the Textbooks and Guidelines Say (Very Clearly):
Mollison’s Blood Transfusion:
- Forward grouping alone is dangerous
- Reverse grouping discrepancy is the key diagnostic clue
- Anti-H must be considered in apparent O groups
Denise Harmening:
- Bombay phenotype produces strong anti-H
- Incompatible with all ABO groups, including O
AABB Technical Manual:
- Both forward and reverse grouping are mandatory
- ABO discrepancies must be resolved before issue
- Rare blood groups must be documented and traceable
WHO Blood Safety Guidance:
- Emphasizes accurate grouping and antibody detection
- Strongly supports rare donor identification and registries
Classic Diagnostic Pattern (Do Not Miss!):
- Forward: anti-A negative | anti-B negative
- Reverse: A, B and O cells all positive
- Anti-H lectin: negative
- Diagnosis: Bombay blood group
Clinical Reality:
- Cannot receive A, B, AB or O blood
- Requires Bombay phenotype donor only
- Missed diagnosis leads to life-threatening reaction
What We MUST Build (System Responsibility):
- Permanent flagging of rare phenotypes
- Counseling and retention of rare donors
- 24/7 emergency donor contact lists
- Inter-hospital and regional networking
- National rare blood donor registry
Final Take-Home Message:
- No reverse grouping means no safe transfusion
- Bombay blood group is rare—but errors should never be
From MBBS textbooks to tertiary hospitals, the message is the same:
Details save lives in transfusion medicine.
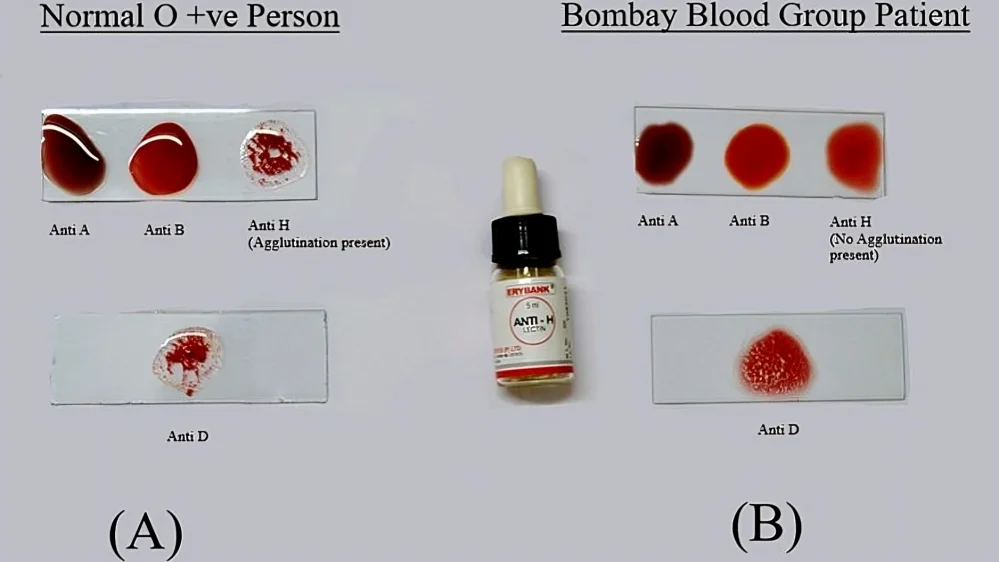
Reference Figure (A)Shows agglutination reaction of the blood sample taken from an individual with an O-positive blood group, showing agglutination with anti-A and anti-B antisera, but no agglutination with anti-D and anti-H antisera.
(B) Represents the patient’s blood sample with an O-positive Bombay blood group which shows agglutination with anti-A, anti-B, and anti-H antisera, but no agglutination with anti-D antisera.”
Stay updated with Hemostasis Today.
-
May 29, 2026, 17:23Rita Schwab: Current Clinical Management of Trauma without the Use of Allogenic Blood Products
-
May 29, 2026, 17:22Brian Schiro: Excited to Provide Guideline Based Care at the Aortic Center
-
May 29, 2026, 17:20Martin Widschwendter: How Molecular Detection Tests Could Transform Endometrial Cancer Care
-
May 29, 2026, 17:18Nina Lansbury: Supporting a Period Friendly World With Menstrual Health Research and Education
-
May 29, 2026, 17:16Ipsita Chatterjee: Red is Not Shame, Red is Power, Red is a Woman
-
May 29, 2026, 16:49Abdulrahman Nasiri: The Evolving Role of Romiplostim in SAA
-
May 29, 2026, 16:46Soumen Bhattacharya: UC-II and Immune Modulation in Osteoarthritis
-
May 29, 2026, 16:38Ana Pedrero Gil: Red Blood Cell Transfusion Practice in Spain – High Inappropriateness Despite Low Overall Use
-
May 29, 2026, 15:40Lena Volland: Expanding Holistic Care in Bleeding Disorders Through Pelvic Health Physical Therapy at WFH Congress

