
Mohamed Magdy Badr: Post-Thrombotic Limb and Venous Ulcer Healing
Mohamed Magdy Badr, Wound Care Consultant at Armed Force Rehabilitation Center, posted on LinkedIn:
”Post-Thrombotic Limb and Venous Ulcer Healing: Why These Wounds Are So Difficult – and How We Can Improve Outcomes
Post-Thrombotic Syndrome (PTS) remains one of the most challenging etiologies behind chronic venous ulcers.
After a DVT, many patients develop residual venous obstruction, valvular incompetence, venous hypertension, edema, skin changes, and microcirculatory failure — all of which create a hostile environment for wound healing.
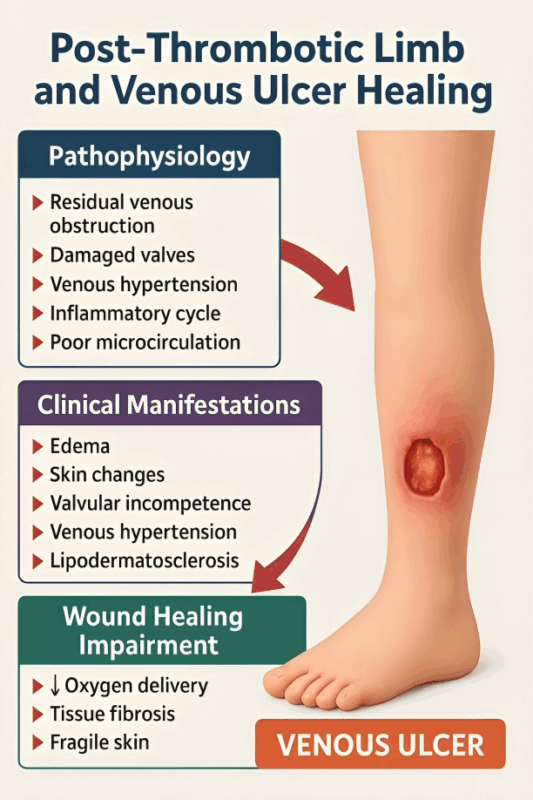
1. Pathophysiology: Why PTS Delays Healing
- Residual venous obstruction → impaired blood return
- Damaged valves → severe reflux
- Venous hypertension → capillary leakage, edema
- Inflammatory cycle → leukocyte trapping, tissue fibrosis
- Poor microcirculation → ↓ oxygen delivery and nutrient supply
- Lipodermatosclerosis → chronic skin fibrosis and fragility
Together, these factors make PTS-related venous ulcers slower to heal and more prone to recurrence.
2. Clinical Challenges in Healing
- Hard, brawny edema resistant to basic compression
- Fibrotic skin with poor elasticity
- Recurrent cellulitis
- Mixed etiology (venous + lymphedema, obesity, CKD, heart failure)
- Poor adherence to long-term compression
- Delayed diagnosis of iliac obstruction (common in PTS)
3. Principles of Effective Management
A. Venous Outflow Restoration (When Needed)
- Consider iliac vein duplex / IVUS in non-healing or recurrent ulcers
- Address residual iliac/femoral obstruction
- Stenting when indicated improves healing and reduces recurrence
B. Compression Therapy (The Cornerstone)
- Multilayer bandaging (40–60 mmHg at ankle)
- Short-stretch or zinc paste boots in severe edema
- Velcro wraps for obese or non-compliant patients
- Long-term maintenance stockings after closure
C. Edema and Inflammation Control
- Limb elevation
- Manual lymphatic drainage when mixed disease
- Anti-inflammatory compression (Unna boot) in lipodermatosclerosis
D. Wound Bed Optimization
- Aggressive debridement of fibrin/tissue necrosis
- Moisture-balanced dressings
- Address biofilm (regular sharp debridement + HOCl)
- Consider advanced therapies: NPWT, biological dressings, PRP
E. Risk Factor Modification
- Weight reduction
- Glycemic control
- Treat heart/renal dysfunction
- Encourage mobility and calf pump activity
4. The Reality: Healing Takes Time
- PTS-related ulcers heal slower than typical venous ulcers
- Recurrence is high without lifelong compression
- Early detection of venous obstruction is critical
- Multidisciplinary care significantly improves outcomes
Take-Home Message
- Post-thrombotic venous ulcers represent the intersection of obstruction, reflux, edema, and microvascular failure.
- Healing requires restoring venous outflow, strict compression, edema reduction, wound bed optimization, and long-term maintenance therapy.
- These wounds can heal – but only with structured, aggressive, and comprehensive venous management.”
Stay informed with Hemostasis Today.
-
May 28, 2026, 17:42Nagendra Sungala: International Clinical Trials Day Validates the Work of Our Hematology Clinical Trials Unit
-
May 28, 2026, 17:41Thomas Pincez: Looking for Great Contributions on Pediatric Hematology
-
May 28, 2026, 17:40Masoabi Sefojane: The Real Cost of a Bleeding Disorder Is More Than Cost Alone
-
May 28, 2026, 17:39Zeyad Kholeif: New Publication on Rapid Plaque Progression Leading to STEMI in a Young Athlete
-
May 28, 2026, 17:39Karina Althaus: Results of the SSC Subcommittee International Survey on HIT
-
May 28, 2026, 16:45Thrilled to Present The ISTH Roberts Award to Donald Arnold – ISTH
-
May 28, 2026, 16:36Connor Webb: IL-6 as a Primer of Platelet Hyperresponsiveness
-
May 28, 2026, 16:19James Farrell: The Power of Linked Electronic Health Records for Understanding Real Patient Journeys
-
May 28, 2026, 16:19Michael Makris: I Hope The Bleeding Disorders Community Supports Kedrion Initiative for FV Deficiency

