
Ifeanyichukwu Ifechidere: Argatroban – Its ‘Rescue Mission’ in Heparin-Induced Thrombocytopenia
Ifeanyichukwu Ifechidere, Specialist Biomedical Scientist at Sheffield Teaching Hospitals NHS Foundation Trust, shared a post on LinkedIn:
”Argatroban: Its ‘Rescue Mission’ in Heparin-Induced Thrombocytopenia (HIT)
Introduction
Heparin-induced thrombocytopenia (HIT) represents one of the most paradoxical and dangerous complications in modern anticoagulant therapy. Despite being triggered by a drug designed to prevent thrombosis, HIT instead creates a highly prothrombotic state, placing patients at significant risk of life-threatening complications.
In this setting, rapid recognition and immediate therapeutic intervention are critical. Among the available treatment options, Argatroban has emerged as a key agent-often described as a ‘rescue therapy’- due to its rapid onset, predictable pharmacology, and effectiveness in preventing thrombotic progression.
This article explores HIT in depth, including its pathophysiology, clinical severity, laboratory diagnosis, and the pivotal role of argatroban. It also examines alternative treatment options, particularly relevant in settings where argatroban availability is limited.
Understanding Heparin-Induced Thrombocytopenia (HIT)
What is HIT?
HIT is an immune-mediated adverse drug reaction that occurs following exposure to heparin. It is characterised by:
- A drop in platelet count (typically a drop of more than 50% from baseline)
- A marked increase in thrombotic risk
Unlike other causes of thrombocytopenia, HIT is not primarily a bleeding disorder. Instead, it is a prothrombotic syndrome, with thrombosis occurring in up to 50% of untreated cases.
Pathophysiology of HIT
At the core of HIT lies an immune response involving:
- Platelet factor 4 (PF4)
- Heparin
- IgG antibodies
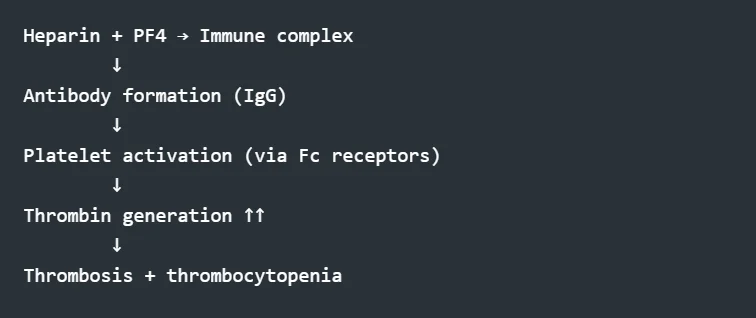
Mechanism
- Heparin binds to PF4 released from platelets
- This complex becomes immunogenic
- The immune system produces anti-PF4/heparin antibodies
- Antibodies bind to platelet Fc receptors
- Platelets become activated and then release procoagulant microparticles
- Result: widespread thrombin generation
Visualising HIT Mechanism
Clinical Severity of HIT
HIT is a medical emergency due to its thrombotic potential.
Complications include:
- Deep vein thrombosis (DVT)
- Pulmonary embolism (PE)
- Arterial thrombosis (stroke, limb ischemia)
- Myocardial infarction
Mortality rates can reach 20–30% if untreated.
Laboratory Investigation of HIT
Accurate diagnosis requires a combination of clinical assessment and laboratory testing.
1․ Clinical Pre-test Probability: The 4Ts Score
The 4Ts scoring system evaluates:
- Thrombocytopenia
- Timing of platelet fall
- Thrombosis
- other causes
A high score suggests strong suspicion of HIT.
2․ Immunological Assays
These detect antibodies against PF4-heparin complexes.
Common test:
ELISA for PF4 antibodies
Advantages:
High sensitivity
Limitations:
Low specificity means it detects non-pathogenic antibodies
3․ Chemiluminescent Assays
ACL Acustar
Advantages:
High Specificity and sensitivity
4․ Functional Assays
These assess whether antibodies actually activate platelets.
Gold standard:
Serotonin Release Assay (SRA)
Other tests:
Heparin-induced platelet activation (HIPA)
Key point:
Functional assays confirm true HIT
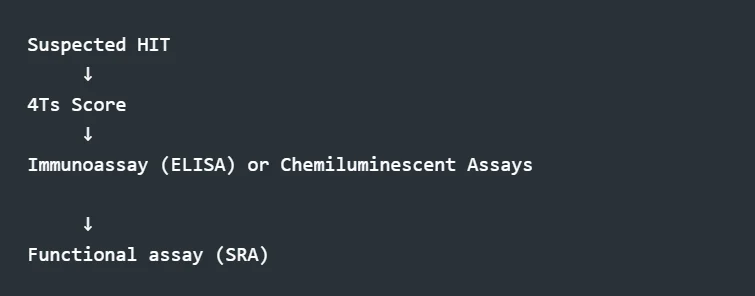
Diagnostic Workflow
The Role of Argatroban in HIT Treatment
Why Heparin Must Be Stopped Immediately
Once HIT is suspected:
- All heparin must be discontinued
- Alternative anticoagulation must be started
Failure to anticoagulate exposes patients to rapid thrombotic progression.
What is Argatroban?
Argatroban is a direct thrombin inhibitor (DTI) administered intravenously.
It is specifically indicated for:
- Treatment of HIT
- Anticoagulation in patients with HIT undergoing procedures
Mechanism of Action
Argatroban works by:
- Directly inhibiting Thrombin (Factor IIa)
- Blocking fibrin formation
- Preventing platelet activation
Key advantage:
It does not interact with PF4, so it does not worsen HIT
Mechanism Diagram

Pharmacological Advantages
- Rapid onset and offset
- Short half-life (~45 minutes)
- Hepatic metabolism (useful in renal impairment)
- Predictable anticoagulant effect
Monitoring Argatroban
Argatroban prolongs:
- aPTT/Heparin Ratio (primary monitoring tool)
- PT/INR (important when transitioning to warfarin)
- Argatroban Assay (drug level confirmation)
Important:
Argatroban can falsely elevate INR, complicating warfarin bridging.
Why Argatroban is Considered a ‘Rescue Therapy’
Argatroban is particularly valuable because:
- It provides immediate anticoagulation
- It is effective in critically ill patients
- It is safe in renal failure
- It reduces thrombotic complications in HIT
In acute HIT, time is critical-and argatroban acts quickly to interrupt thrombin-driven thrombosis.
Alternatives to Argatroban
In some settings, argatroban may be unavailable or limited. Several alternatives can be used.
1. Bivalirudin
Features:
- Direct thrombin inhibitor
- Short half-life
- Commonly used in cardiac procedures
Limitations:
- Renal clearance
- Cost
2. Fondaparinux
Features:
- Indirect Factor Xa inhibitor
- Subcutaneous administration
- Increasingly used off-label for HIT
Advantages:
- Convenient dosing
- Lower risk of HIT
3. Direct Oral Anticoagulants (DOACs)
Examples include:
- Rivaroxaban
- Apixaban
Role:
Emerging option for HIT management
Benefits:
- Oral administration
- No routine monitoring
4. Danaparoid (where available)
- Indirect anti-Xa activity
- Low cross-reactivity with HIT antibodies
Choosing an Alternative
Drug Route Clearance Key Use
Argatroban IV Liver First-line in many settings
Bivalirudin IV Kidney Cardiac patients
Fondaparinux SC Kidney Resource-limited settings
DOACs Oral Mixed Long-term management
Laboratory Considerations During Argatroban Therapy
Argatroban interferes with coagulation tests:
- Prolongs aPTT
- Elevates INR
- Affects thrombin time
Laboratories must:
- Be aware of therapy
- Adjust interpretation
- Use appropriate monitoring protocols
Challenges in Resource-Limited Settings
In many healthcare systems:
- Argatroban availability is limited
- Cost is prohibitive
Practical approaches:
- Use fondaparinux where safe
- Transition to DOACs early
- Avoid heparin re-exposure
- Strengthen laboratory diagnosis
Clinical Case Example
A 65-year-old patient receiving heparin develops:
- Platelet drop from 250 to 90 ×10⁹/L
- New DVT
Action:
- Calculate 4Ts score to assess for a high probability
- Stop heparin immediately
- Start argatroban
Outcome:
- Platelet recovery
- No further thrombosis
Conclusion
Heparin-induced thrombocytopenia is a serious, immune-mediated condition that transforms anticoagulation into a prothrombotic crisis. Early recognition, accurate laboratory diagnosis, and prompt treatment are essential to prevent life-threatening complications.
Argatroban plays a critical role in this setting. As a direct thrombin inhibitor, it bypasses the immune mechanisms of HIT and provides rapid, effective anticoagulation. Its pharmacological properties-particularly its hepatic clearance and short half-life-make it especially valuable in critically ill patients.
However, the realities of global healthcare require flexibility. Alternatives such as bivalirudin, fondaparinux, and DOACs provide viable options where argatroban is unavailable.
Ultimately, successful management of HIT depends on a combination of:
- Clinical vigilance
- Laboratory expertise
- Appropriate anticoagulant selection
In this context, argatroban truly serves as a “rescue mission” drug, intervening at a critical moment to restore balance in a dangerously dysregulated haemostatic system.
References
- Warkentin TE. Heparin-induced thrombocytopenia. New England Journal of Medicine.
- Cuker A, et al. American Society of Hematology guidelines for HIT management. Blood Advances.
- Greinacher A. Clinical practice of HIT. Journal of Thrombosis and Haemostasis.
- Linkins LA, et al. Treatment and prevention of HIT. Chest Guidelines.
- Favaloro EJ. Laboratory testing for HIT. Seminars in Thrombosis and Hemostasis.
- Lewis BE, et al. Argatroban therapy in HIT. Circulation.”
Other posts featuring Ifeanyichukwu Ifechidere on Hemostasis Today.
-
May 31, 2026, 16:29José Antonio García Erce: Collaborative PBM Implementation in Transfusion Centers and Services
-
May 31, 2026, 16:22Vera Ignjatović: How Do We Rigorously Study These Drugs in Children to Understand Their True Benefits and Risks?
-
May 31, 2026, 16:21Ksenija Stach: Is This The Future of Lipid-Lowering Lherapy?
-
May 31, 2026, 15:42Antonio Greco: Balancing Bleeding and Thrombotic Risk After PCI
-
May 31, 2026, 15:41Eric Topol: Replication of Plasma p-tau217 Blood Test for Predicting Alzheimer’s Disease
-
May 31, 2026, 15:32ASH Invites Dynamic Members to Apply for 2027 Leadership and Committee Roles
-
May 31, 2026, 14:39Monique Gore-Massy: Redefining Lupus Innovation Through Patient Partnership
-
May 31, 2026, 14:31Mirjam Teboe: The Golden Rule Behind Reliable Lupus Anticoagulant Testing
-
May 31, 2026, 14:20Improving Access to Care for People Living with Haemophilia and Haemoglobinopathies – NNHF

