
Jim Hoffman on the Gut-Vascular Axis: How a Poor Diet Fuels NETosis and Immunothrombosis
Jim Hoffman, Former Technical Advisor at Cygnus Technologies, LLC, posted on LinkedIn:
“A poor gut microbiome, nurtured by prolonged consumption of unhealthy foods, particularly those high in sugar (HFCS and sucrose), can exacerbate NETosis dysregulation, impair fat metabolism and increase the risk of immunothrombotic damage to the all-important gut lining that protects the blood supply from unwanted gut hypertoxicity. “Leaky gut” is a consequence of bacteria and/or their endotoxin and enterotoxin byproducts translocating too easily from the gut into the bloodstream, which can further amplify unwanted neutrophil hyperactivation in the blood, aggravating NETosis induction, and compromising the efficiency of macrophage-mediated NET clearance from the blood and tissues.
NETosis hyperactivation in the blood can also put distant organs and their vascular blood supply at increased risk of tissue-damaging immunothrombosis, both vasculitis and thrombosis, most characteristically observed in severe sepsis and critically ill ICU patients with confirmed disseminated intravascular coagulation, who are known to experience accelerated life-threatening NETosis-mediated damage to the systemic vasculature.
Often, NETosis-mediated vascular and intestinal injury may also originate outside the gut, triggered by respiratory infections, resulting from other non-respiratory infections, and also from other non-infectious toxin overexposures. All of these exposures can potentially hyperactivate NETosis dysregulation, causing immunothrombotic injury to the gut lining and the systemic vasculature of other vulnerable distant tissues and organs.
Fadini et al provides greater insight into how a poor diet, high in sugar and fat, can adversely impact NETosis dysregulation to the detriment of the host.
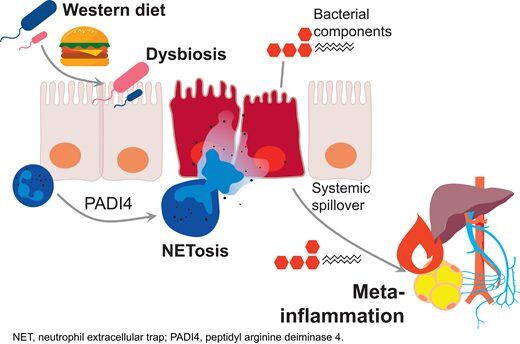
Padi4-Dependent NETosis Enables Diet-Induced Gut Hyperpermeability, Translating Dysbiosis Into Systemic Inflammation and Dysmetabolism. Fadini et al 2025″
Explore more posts for deeper insights into hemostasis with Hemostasis Today.
-
Jun 8, 2026, 16:00Despina Fotiou: Advancing Recognition Through Global Case Collaboration
-
Jun 8, 2026, 15:43Jigyasa Pal: Beyond Care – Empowering Lives with HPAP
-
Jun 8, 2026, 15:36New Approaches in Bleeding Disorders Care – SAHF
-
Jun 8, 2026, 15:34Besher Shami: A Unique Presentation of Warfarin-Associated Aortic Perforation
-
Jun 8, 2026, 15:29Shreyashree Sarkar: Oxidative Stress and Neutrophil-Driven Mechanisms in Cancer-Associated Thrombosis at Vascular Discovery 2026
-
Jun 8, 2026, 15:23Gloria Duah: Can a Blood Transfusion Change Your Blood Type?
-
Jun 8, 2026, 14:52Indunil Karunarathna: A Comprehensive New Guide to Haemolytic Uremic Syndrome
-
Jun 8, 2026, 14:45Vikramaditya Gangakar: A Comprehensive Overview of Enoxaparin
-
Jun 8, 2026, 14:42Abdul Muqtadir Abbasi: Hematology Cheat Sheet – Blood Transfusion Reactions

