
Reza Shojaei: Designing Blood Systems for Chronic Demand
Reza Shojaei, Chief Operating Officer at Canadian Plasma Resources, shared a post on LinkedIn:
“Special Edition: Marking World Thalassemia Day

Thalassemia is often framed as a genetic disorder requiring lifelong care.
From a systems perspective, however, it represents something far more consequential:
- A permanent, predictable, and non-discretionary demand signal on national blood systems.
In an era where most blood demand is episodic (trauma, surgery, acute care), Thalassemia introduces a fundamentally different dynamic, chronic transfusion dependency.
Understanding this distinction is critical because it exposes structural weaknesses in how blood systems are designed, funded, and scaled.
This is not just about one disease. It is about how future blood supply systems must evolve to support chronic demand at scale.

Thalassemia as a Structural Demand Driver
Thalassemia, particularly β-thalassemia major, requires regular red blood cell (RBC) transfusions every 2–4 weeks to sustain life (World Health Organization, 2023). Unlike acute transfusion needs, this demand is:
- Predictable (scheduled lifelong therapy)
- Non-elastic (cannot be deferred without clinical consequences)
- Cumulative (patients require hundreds of transfusions over a lifetime)
Globally, it is estimated that over 300,000 children are born annually with severe hemoglobin disorders, including Thalassemia and sickle cell disease (Thalassemia International Federation, 2021).
In high-prevalence regions, such as the Mediterranean, Middle East, South Asia, and Southeast Asia, this creates a continuous baseline demand for RBC units that persists irrespective of seasonal or emergency fluctuations.
From a supply chain standpoint, this shifts blood demand from a reactive model to a programmatic obligation.
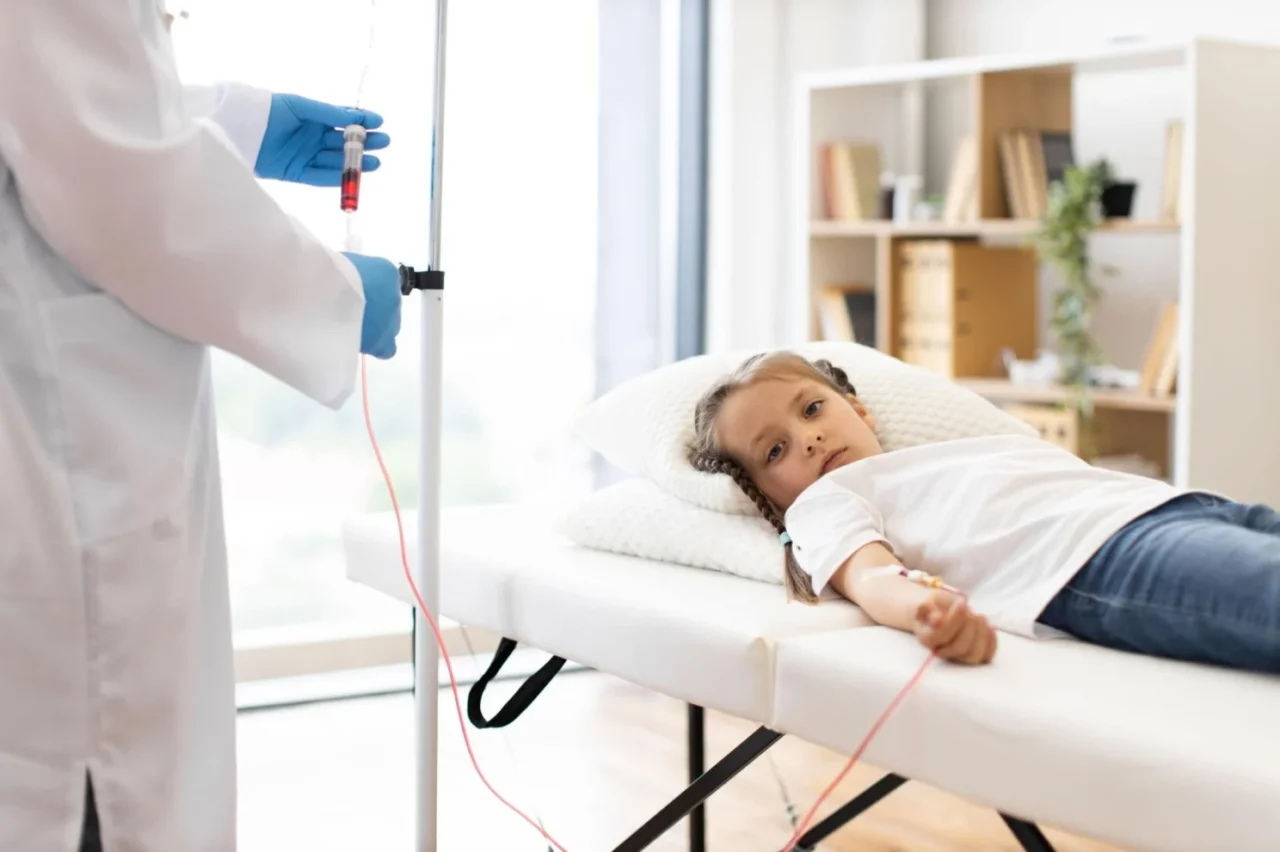
For transfusion-dependent patients, blood is not emergency medicin; it is ongoing life support.
The Mismatch: Chronic Demand vs Episodic Supply
Most national blood systems are architected around episodic demand patterns:
- Trauma and emergency care
- Elective surgeries
- Short-term clinical interventions
Donor recruitment strategies, inventory management, and collection campaigns are typically designed around variability and surge response, not steady-state chronic consumption.
This creates a structural mismatch:

Red blood cells have a shelf life of nearly 42 days, imposing strict inventory turnover constraints (American Association of Blood Banks, 2022).
For chronic patients, however, demand is indefinite and recurring, requiring highly synchronized supply planning.
The result is systemic fragility:
- Periodic shortages
- Allocation prioritization
- Increased reliance on emergency imports
Geographic Reality: Where the Pressure Is Highest
The burden of Thalassemia is not evenly distributed. Regions with the highest disease prevalence often face:
- Lower donor participation rates
- Fragmented blood infrastructure
- Limited inventory management capabilities
For example:
- In parts of South Asia and the Middle East, transfusion-dependent patients may face inconsistent access to safe blood
- In some low- and middle-income countries (LMICs), screened blood availability remains below demand thresholds (World Health Organization, 2023)
This creates a dual challenge:
- High chronic demand plus constrained supply systems equal to systemic inequity in patient access
Even in developed markets, the challenge is shifting.
Aging populations, declining donor pools, and increasing chronic disease burdens are beginning to replicate similar pressures at a different scale.
Blood systems are increasingly interconnected, yet chronic demand continues to outpace structural preparedness.
Forecasting Failure: Why Traditional Models Fall Short
Traditional blood demand forecasting models are often built on:
- Historical utilization trends
- Hospital activity projections
- Seasonal adjustments
However, Thalassemia exposes a key limitation:
Historical models underweight chronic, non-variable demand signals
For transfusion-dependent populations:
- Demand is fixed per patient
- Growth is driven by diagnosis rates and survival improvements
- Variability is minimal, but volume is guaranteed
This requires a shift toward patient-based demand modelling, where:
- Total demand equal to (Number of transfusion-dependent patients) times (Units per patient per year)
Such models enable:
- More accurate national demand planning
- Long-term donor recruitment strategies
- Infrastructure investment alignment
Operational Implications: What Must Change
To align supply systems with chronic demand realities, several structural shifts are required:
- From Campaign-Based to Programmatic Collection: Blood systems must transition from event-driven donor campaigns to continuous donor engagement ecosystems that support a stable baseline supply.
- Donor Retention Over Acquisition: Chronic demand favors high-frequency, repeat donors, making retention strategies more valuable than episodic recruitment.
- Advanced Inventory Optimization: Real-time inventory visibility, predictive analytics, and regional redistribution capabilities are essential to balance supply-demand mismatches.
- Integrated National Planning: Thalassemia care programs must be fully integrated with national blood services to ensure alignment between patient registries and supply planning.
- Quality and Compatibility Focus: Repeated transfusions increase the risk of alloimmunization, necessitating more sophisticated matching protocols and inventory segmentation (Taher et al., 2021).
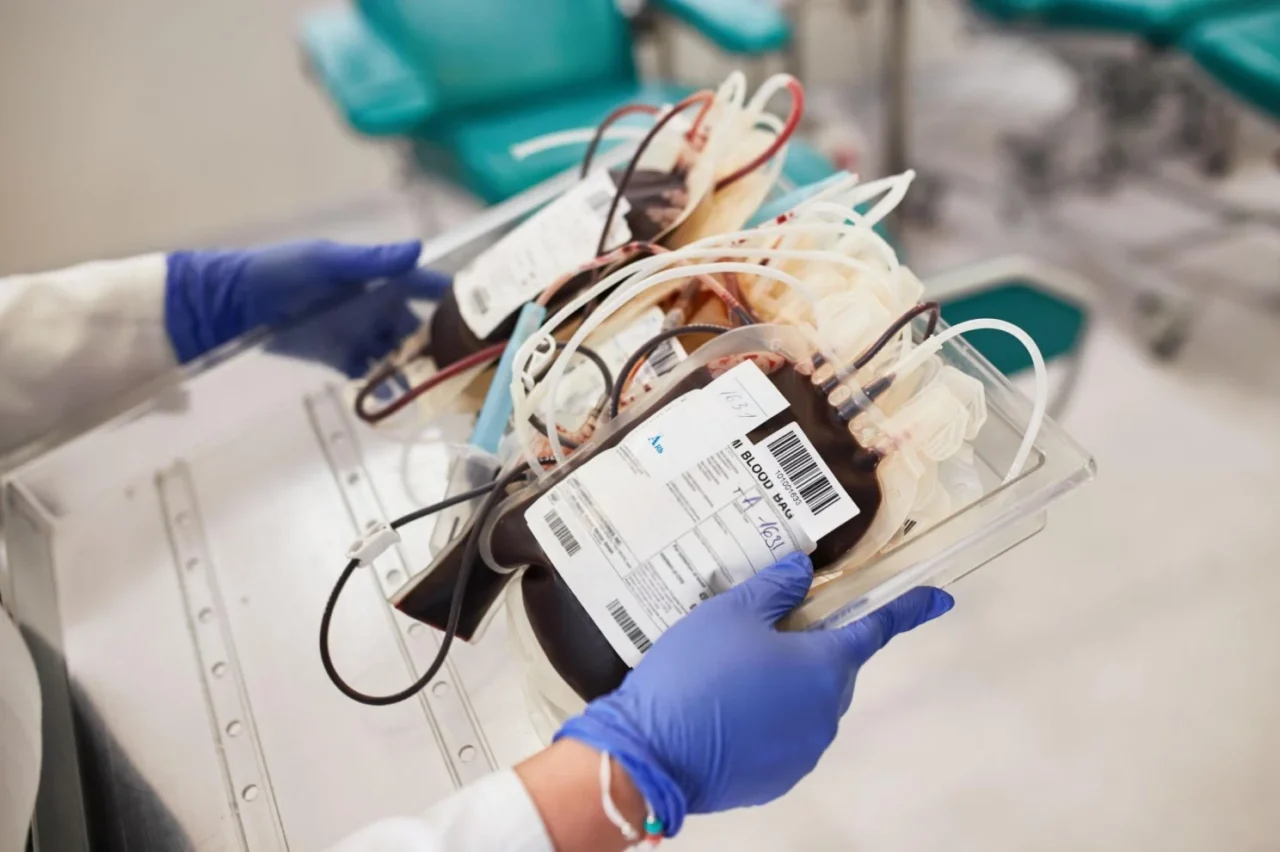
Chronic demand requires infrastructure designed for continuity, precision, and resilience.
The Future: Blood Systems as Chronic Care Infrastructure
Thalassemia is not an outlier; it is a preview of future healthcare demand dynamics.
As chronic diseases increase globally, healthcare systems will increasingly depend on:
- Continuous biologic supply chains
- Predictable, long-term treatment models
- Integrated patient–supply ecosystems
- Blood systems must evolve accordingly, from reactive service providers to strategic healthcare infrastructure platforms.
This includes:
- Digital donor ecosystems
- National patient registries
- AI-driven demand forecasting
- Cross-border supply coordination
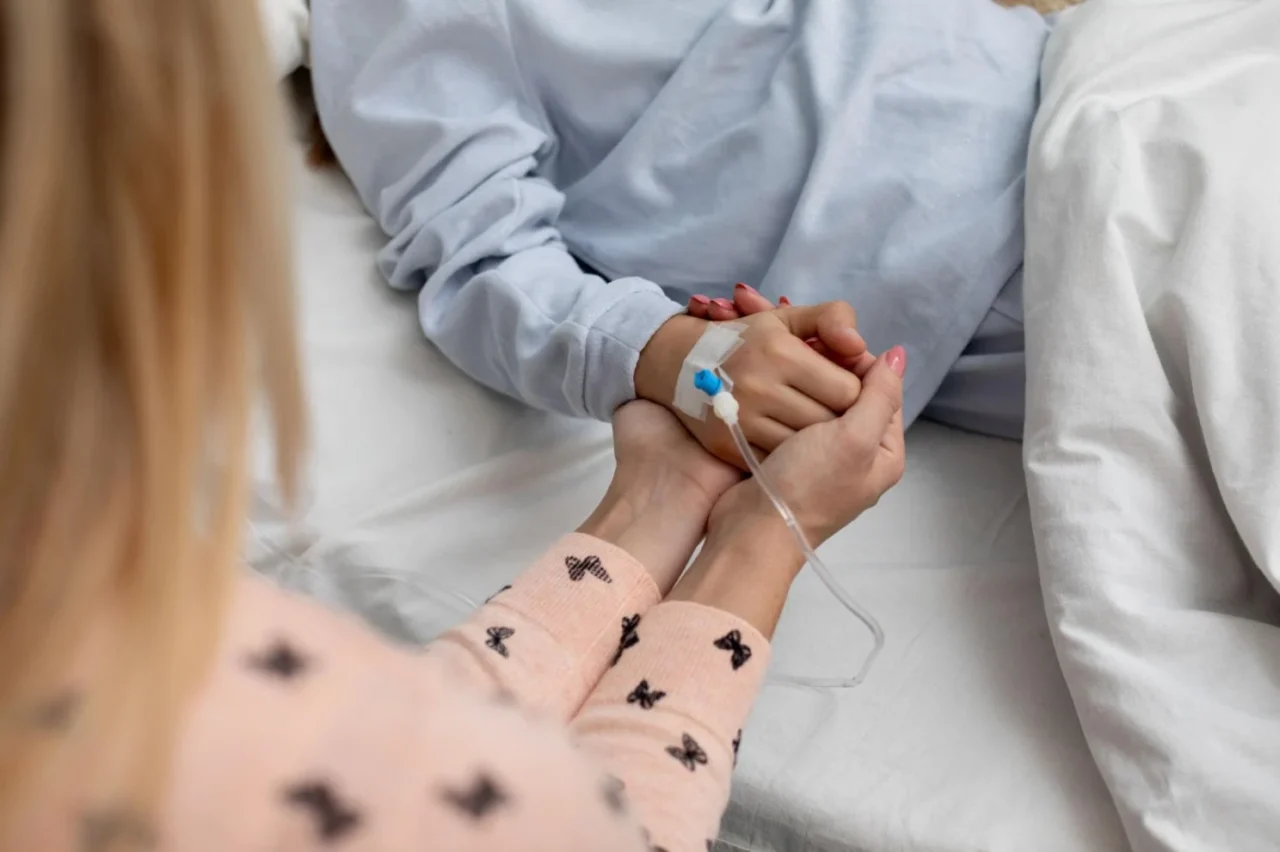
Reliable blood systems are not just operational assets; they are lifelines for patients and families.
Executive Perspective
From an operational standpoint, the lesson is clear:
- Blood supply systems designed for episodic demand cannot sustainably support chronic disease burdens.
Thalassemia forces us to confront this reality and to redesign systems accordingly.
The strategic question for leaders is not How do we manage shortages?
It is: How do we redesign blood systems for predictable, lifelong demand?
Final Thought
Behind every unit of blood is a patient whose life depends on the system’s reliability, not just its availability.
Thalassemia patients do not need blood occasionally. They need it consistently, safely, and indefinitely.
- The future of blood systems will be defined not by how they respond to emergencies, but by how well they sustain chronic care at scale.
References
World Health Organization. (2023). Blood safety and availability.
Thalassemia International Federation. (2021). Guidelines for the management of transfusion dependent thalassemia.
American Association of Blood Banks. (2022). Standards for blood banks and transfusion services.
Taher, A. T., Musallam, K. M., Cappellini, M. D., & Weatherall, D. J. (2021). Optimal management of β-thalassemia major. The Lancet Haematology, 8(6), e421–e433.”
More posts featuring Reza Shojaei on Hemostasis Today.
-
May 12, 2026, 11:13Matteo Foschi: Grateful To Be Selected for The WSO Future Stroke Leaders Programme
-
May 12, 2026, 11:05Omid Seidizadeh: Strategies to Guide The 2nd 100 years of VWD Care and Research
-
May 12, 2026, 11:01Kate Scrivener: The Big Picture of Exercise Trials to Prevent Falls After Stroke
-
May 12, 2026, 10:39Rucha Patil: Our ”Factor VIII Inhibitor Point-of-Care Diagnostic” Is Successfully Transferred at Science-Tech
-
May 12, 2026, 10:26Fabrice Cognasse: The EFS Is First and Foremost Part of a Medical Discipline – Transfusion
-
May 11, 2026, 16:52Luke McLaughlin: Raising Awareness on Haemophilia Issues at ENIL Lead On
-
May 11, 2026, 16:49Jeff Sternlicht: Normal LDL Does Not Always Mean Low Risk
-
May 11, 2026, 16:42Archil Jaliashvili: From Managing Blood to Managing Oxygen Metabolism
-
May 11, 2026, 16:42Heghine Khachatryan: Celebrating One Hundred Years of von Willebrand Disease with EHC

