
Ifeanyichukwu Ifechidere: Anaemia is not a Diagnosis – It’s a Symptom
Ifeanyichukwu Ifechidere, Biomedical Scientist at Sheffield Teaching Hospitals NHS Foundation Trust, posted on LinkedIn:
”’Anaemia is not a diagnosis – it’s a symptom.’
As biomedical scientists, one of the most important mindset shifts we can make is this:
- Anaemia doesn’t tell you what the problem is.
- It tells you there is a problem.
Low haemoglobin is the starting point – not the conclusion.
The real work begins when we ask:
What type of anaemia is this? And why?
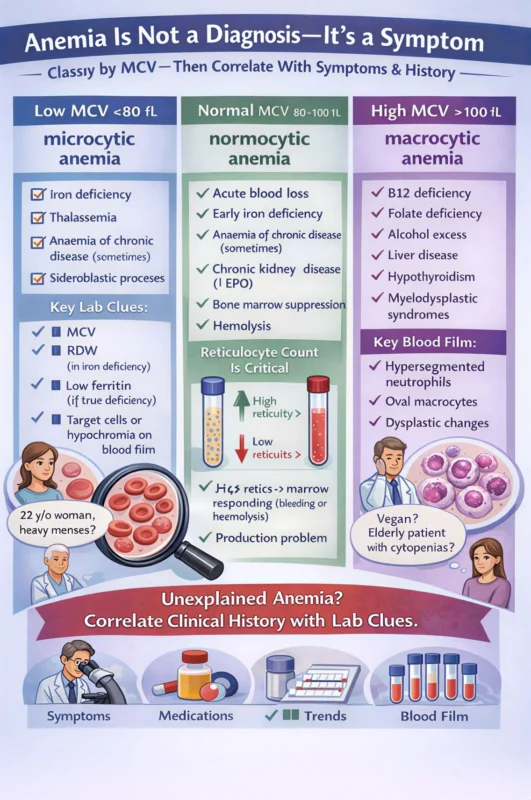
Step 1: Classify by MCV – Microcytic, Normocytic, or Macrocytic
The Mean Corpuscular Volume (MCV) is more than a number.
It’s a diagnostic compass.
Microcytic Anaemia (Low MCV)
Think: Impaired haemoglobin production
Most common causes:
- Iron deficiency
- Thalassaemia trait
- Anaemia of chronic disease (sometimes)
- Sideroblastic processes
Key lab clues:
- Increased MCV
- Deceased RDW (in iron deficiency)
- Low ferritin (if true deficiency)
- Target cells or hypochromia on blood film
But here’s where clinical-lab correlation matters:
A 22-year-old woman with heavy menses?
Very different from a 68-year-old man with new microcytosis.
Same indices. Very different implications.
Normocytic Anaemia (Normal MCV)
This is where many clinicians get stuck.
Normocytic does not mean normal physiology.
Think:
- Acute blood loss
- Early iron deficiency
- Anaemia of chronic disease
- Chronic kidney disease (decrease EPO)
- Bone marrow suppression
- Haemolysis
Now the reticulocyte count becomes critical:
- High retics to marrow responding (bleeding or haemolysis)
- Low retics to production problem
Without reticulocytes, you’re only seeing half the picture.
Macrocytic Anaemia (High MCV)
Think: DNA synthesis or marrow dysfunction
Common causes:
- Vitamin B12 deficiency
- Folate deficiency
- Alcohol excess
- Liver disease
- Hypothyroidism
- Myelodysplastic syndromes
Blood film can be transformative here:
- Hypersegmented neutrophils
- Oval macrocytes
- Dysplastic changes
And again — context matters.
Macrocytosis in a vegan patient?
Different from macrocytosis in a 72-year-old with cytopenias.
The Most Important Step: Clinical–Laboratory Correlation
A haemoglobin value in isolation is a number.
Add:
- Symptoms (fatigue, weight loss, bleeding)
- Medication history
- Renal function
- Inflammatory markers
- Serial trends
- Blood film morphology
Now it becomes a narrative.
As biomedical scientists, our role is not just to validate results – it’s to interpret patterns, question inconsistencies, and know when something doesn’t fit.
Because:
- Not all iron deficiency is dietary.
- Not all macrocytosis is B12.
- Not all normocytic anaemia is ‘chronic disease.’
Anaemia is the smoke.
Our job is to help locate the fire.
How do you approach unexplained anaemia?
Do you start with indices, reticulocytes, iron studies – or the blood film first?
Let’s discuss the frameworks that have shaped your practice.”
Stay updated with Hemostasis Today.
-
Apr 29, 2026, 17:25Robert Brodsky: Ravulizumab Appears To Be Safe And Effective In Pregnancy
-
Apr 29, 2026, 16:53Chokri Ben Lamine: IV Iron Showdown – FCM vs Ferric Derisomaltose vs Iron Dextran
-
Apr 29, 2026, 16:46Deep Vein Thrombosis Risk in Jobs with Prolonged Sitting – NBCA
-
Apr 29, 2026, 16:41Vikramaditya Gangakar: Essential Pharmacy Facts You Should Know About Aspirin
-
Apr 29, 2026, 16:17W. Alberto Sifuentes Giraldo: Non-Criteria Manifestations of Antiphospholipid Syndrome
-
Apr 29, 2026, 16:12Mavis Agnes Kisakye: Concluding a Successful Entrepreneurs Training for Empowering Ptients’ Mothers
-
Apr 29, 2026, 15:48Kriti Batni: Happy to Share Current Use and Future Directions of Monoclonal Antibodies in Medicine Update 2026
-
Apr 29, 2026, 15:46Dima Shulkin: Comparing HALP and PIV for Mortality Prediction in ACS
-
Apr 29, 2026, 15:44Sonal Sonu: Securing First Prize in Research Oral Presentation at the CME

