
Arun Chervu: Most DVT Patients Do Well on Anticoagulation Alone
Arun Chervu, Physician at Hyperbaric Physicians of Georgia, Founder and CEO and Medical Consultant at AIC Medical Consultants LLC, shared a post on LinkedIn:
”Most DVT patients do well on anticoagulation alone.
A small minority truly qualify for catheter‑directed thrombolysis (CDT) or mechanical thrombectomy (removing the clot with a device)
Those patients usually have:
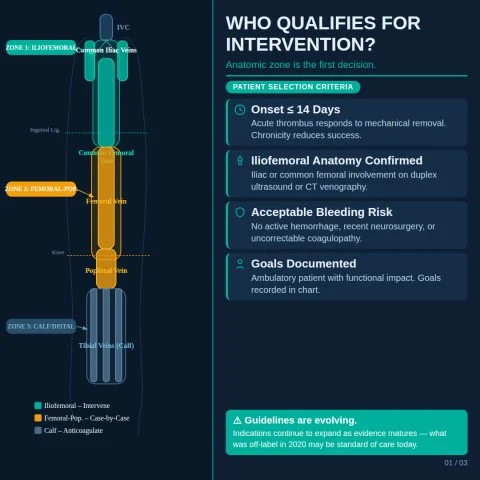
- Iliofemoral DVT, not just calf or femoral clot.
- Symptoms under about 14 days.
- Significant pain/swelling or threatened limb.
- Acceptable bleeding risk and reasonable life expectancy.
ATTRACT taught us something important.
No mortality benefit.
Modest reduction in moderate–severe post‑thrombotic syndrome.
Clear increase in major bleeding with lytic (clot dissolving) therapy.
Since then, the field has moved.
We are using more mechanical thrombectomy with little or no lytic in carefully selected iliofemoral DVT.
Propensity‑matched data now show lower post-thrombotic syndrome (PTS) rates and better Villalta scores with mechanical thrombectomy than with anticoagulation alone in these patients.
The benefit is functional: less long‑term leg damage, not ‘saving a life.’
Not all thrombectomy is the same.
Large‑bore, purely mechanical systems look safer and more efficient than older rheolytic or aspiration devices.
We are seeing lower transfusion rates, lower in‑hospital mortality, and fewer ICU days in some of these series.
But we still see complications: re‑thrombosis, access‑site bleeding, occasional PE, and the need for transfusion.
For plaintiff teams:
- Was this a true iliofemoral, high‑symptom, low‑bleeding‑risk patient?
- Was early thrombus removal even considered or documented?
- If intervention was done, did anyone explain that the goal was symptom and PTS reduction-not survival-and that device‑specific risks exist?
For defense teams:
Does the record show the team correctly classified the DVT and applied modern criteria?
Is there a clear note walking through:
- Anatomy.
- Symptom duration.
- Bleeding risk.
- And patient goals before choosing anticoagulation alone vs CDT vs mechanical thrombectomy?
If mechanical thrombectomy was used.
Is there a documented, thoughtful device choice tied to bleeding risk and long‑term limb function?
After three decades in vascular surgery, this is where I see cases turn.
Not on whether a hospital owned a specific device.
On whether the treating team:
- Recognized the right candidates.
- Understood the limits of the evidence.
- And documented their reasoning.
Indications and guidelines for iliofemoral DVT intervention and mechanical thrombectomy are evolving; what was experimental a decade ago may now be a reasonable option for carefully selected patients.”
Stay updated with Hemostasis Today.
-
May 12, 2026, 14:01Moses Wasswa: Tackling Sickle Cell Disease in Uganda
-
May 12, 2026, 13:49Shashank Joshi: Antiphospholipid Antibodies and Risk of Thrombotic Cardiovascular Events
-
May 12, 2026, 13:44Hayley Evans: Variability in Perioperative TXA Practice Despite Strong Evidence
-
May 12, 2026, 11:13Matteo Foschi: Grateful To Be Selected for The WSO Future Stroke Leaders Programme
-
May 12, 2026, 11:05Omid Seidizadeh: Strategies to Guide The 2nd 100 years of VWD Care and Research
-
May 12, 2026, 11:01Kate Scrivener: The Big Picture of Exercise Trials to Prevent Falls After Stroke
-
May 12, 2026, 10:39Rucha Patil: Our ”Factor VIII Inhibitor Point-of-Care Diagnostic” Is Successfully Transferred at Science-Tech
-
May 12, 2026, 10:26Fabrice Cognasse: The EFS Is First and Foremost Part of a Medical Discipline – Transfusion
-
May 11, 2026, 16:52Luke McLaughlin: Raising Awareness on Haemophilia Issues at ENIL Lead On

