
Ifeanyichukwu Ifechidere: ‘Almost Normal’ CBC Results Can Be the Most Dangerous
Ifeanyichukwu Ifechidere, Specialist Biomedical Scientist at Sheffield Teaching Hospitals NHS Foundation Trust, shared a post on LinkedIn:
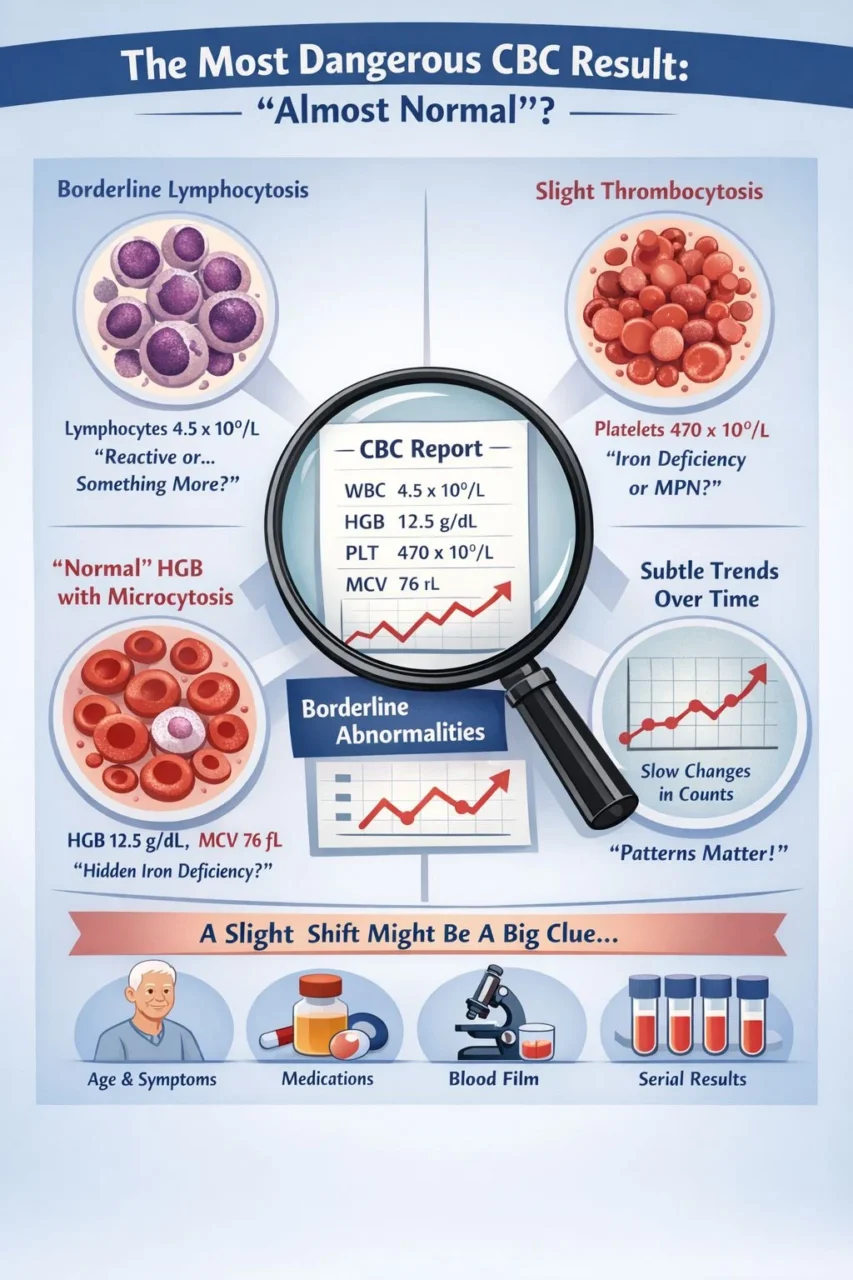
“‘The most dangerous CBC result is often the one that looks almost normal.’
As biomedical scientists, we’re trained to flag the bold, the red, the critical.
But it’s often the borderline Full Blood Count (FBC) that carries the real clinical weight.
- Not the haemoglobin of 6 g/dL.
- Not the platelets of 12 ×10⁹/L.
Those are obvious.
I’m talking about:
- A lymphocyte count just nudging above the upper reference limit
- A platelet count sitting at 470 ×10⁹/L
- A haemoglobin drifting downward but still technically “normal”
- An MCV creeping upward by 2–3 fL over serial tests
Individually? Easy to dismiss.
Together or trending? A story waiting to be told.
Borderline lymphocytosis
A lymphocyte count of 4.2–4.8 ×10⁹/L might be labelled ‘reactive.’
But persistent subtle elevation – especially in adults – should prompt a closer look at morphology and clinical context.
Early lymphoproliferative disorders don’t always shout. Sometimes they whisper.
Slight thrombocytosis
Platelets at 450–500 ×10⁹/L are frequently attributed to inflammation, iron deficiency, or recent infection.
But sustained mild thrombocytosis?
That’s when you consider:
- Iron studies
- Inflammatory markers
And yes – the possibility of early myeloproliferative disease
‘Normal’ haemoglobin with microcytosis
A haemoglobin of 12.5 g/dL might not trigger alarms.
But pair it with an MCV of 76 fL and rising RDW – and you may be catching iron deficiency before anaemia declares itself.
Prevention lives in the margins.
Subtle trends matter more than single values
The FBC is dynamic physiology captured in numbers.
One ‘almost normal’ result rarely means much.
But:
- A slow platelet climb over 18 months
- A steady lymphocyte increase
- A gradual MCV rise
These patterns separate technicians from scientists.
The real danger?
Normalising abnormalities because they don’t look dramatic.
In laboratory medicine, context is king:
- Age
- Symptoms
- Medications
- Serial results
- Blood film morphology
The FBC is not just a test.
It’s an early warning system – if we’re paying attention.
As biomedical professionals, our value isn’t in printing numbers.
It’s in interpreting patterns.
What’s the most easily missed abnormality you’ve seen?
Let’s share the cases that taught us to look twice.”
Stay updated with all scientific advances on Hemostasis Today.
-
May 10, 2026, 18:07Recurrent DVT and PE in Young Adults May Indicate an Underlying Cause – The Lancet Group
-
May 10, 2026, 18:06Noemi Zampatti: Pediatric Celiac Crisis Complicated by Refeeding Syndrome and Proposed Diagnostic Criteria
-
May 10, 2026, 18:05Giovanni Solimeno: When the Common Femoral Artery Wall is Diseased, Closure is Not a Step
-
May 10, 2026, 18:04Maitri Vaishnav: The Bombay Blood Group and the Critical Role of the H Antigen
-
May 10, 2026, 18:03Nicolas Hubacz: Mesenchymal Stem Cells Are Some of the Most Fascinating Cells in Regenerative Medicine
-
May 10, 2026, 16:20Joshua Ngimbwa: How Sex and Socioeconomic Factors Influence Stroke Outcomes in Tanzania
-
May 10, 2026, 16:18Gustavo Monnerat: How Thousands of Fake References Slipped Into Biomedical Literature
-
May 10, 2026, 16:13Dalius Jatužis: Our AI-Driven Automated Stroke Registry Data Extraction Gets Best Poster Award at ESOC 2026
-
May 10, 2026, 16:11Full House for Breakfast with the Experts – American Society for Apheresis

