
Pauline Nerwande: Hemostasis and the Balance Between Bleeding and Thrombosis
Pauline Nerwande, Aspiring Medical Laboratory Technologist in AI‑Driven Healthcare, shared a post on LinkedIn:
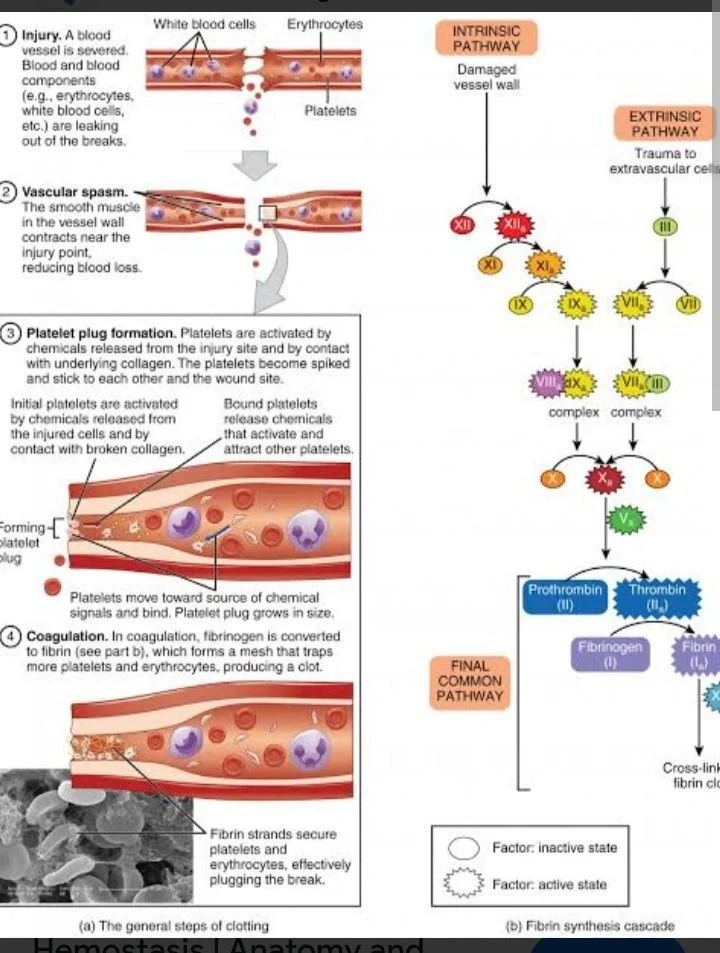
“Understanding Hemostasis: How the Body Stops Bleeding
Imagine a water pipe gets damaged.
If nothing blocks the leak, water keeps flowing out.
Your blood vessels work the same way. When a vessel is injured, the body immediately activates a repair system called hemostasis to stop blood loss while still keeping blood flowing normally elsewhere.
Hemostasis happens in four major stages:
- Vasoconstriction (The Vessel Tightens)
The moment a blood vessel is damaged, the vessel wall contracts and becomes narrower.
Think of squeezing a leaking hose pipe to reduce water flow.
This narrowing:
- Reduces blood loss
- Slows blood flow to the injured area
- Gives the body time to start repairs
Damaged tissues release chemicals such as endothelin that help the vessel constrict.
2. Platelet Plug Formation (Temporary Repair)
Platelets are tiny cell fragments circulating in blood.
Normally, they move smoothly without sticking to vessels.
But when injury exposes the inner collagen layer of the vessel:
What happens?
- Adhesion: Platelets stick to the damaged area using a protein called von Willebrand factor (vWF).
- Activation: The platelets change shape and become “sticky.”
They release chemicals like:
- ADP
- Thromboxane A₂
- Serotonin
These chemicals attract more platelets.
- Aggregation
More and more platelets gather together, forming a platelet plug.
This plug is only temporary and weak, like using tape to close a crack before proper repair.
3. Coagulation (Blood Clot Formation)
Now the body builds a stronger seal.
Special proteins called clotting factors activate one another in a chain reaction called the coagulation cascade.
The main goal is to produce thrombin.
Fibrin forms long thread-like fibers that create a mesh over the platelet plug.
Think of it like steel bars reinforcing wet cement.
This forms a stable blood clot that firmly seals the damaged vessel.
4. Clot Retraction and Fibrinolysis (Cleanup and Healing)
After the vessel heals:
- Clot Retraction: Platelets contract and pull the clot edges closer together.
This helps: Strengthen the repair and reduce the size of the wound
- Fibrinolysis
The body must remove the clot once healing is complete.
An enzyme called plasmin breaks down fibrin.
This prevents unnecessary blockage inside blood vessels.
Why Hemostasis Matters in Hematology?
Problems in hemostasis can cause serious diseases:
- Hemophilia: Blood fails to clot properly
- Thrombosis: Excessive clot formation
- Stroke and heart attack: Clots blocking blood vessels
This is why coagulation studies are very important in laboratories and hospitals.”
Stay updated with Hemostasis Today.
-
May 14, 2026, 13:54Abdul Mannan: The Dual Biology of the Sickle Cell Mutation
-
May 14, 2026, 13:53Anna Oleksiak: Managing Anticoagulation Decisions in Critically Ill Cardiac Patients
-
May 14, 2026, 13:46Muhammad Usman: A Practical Overview of Major Blood Components and Their Clinical Use
-
May 14, 2026, 13:34Cynthia Lua: Mental Health Support for Hemophilia Caregivers at the HFA Symposium
-
May 14, 2026, 13:34Nicolas Hubacz: Mapping the Brain’s Mesoscopic Vascular Infrastructure
-
May 14, 2026, 13:20Marcel Émond: When to Restart Anticoagulation After Complex MTBI in the Patient?
-
May 14, 2026, 13:17Amelia Carro Hevia: Improving Heart Failure Care Through Sex-Informed Strategies
-
May 14, 2026, 12:46Ali Sohail: Presenting GI Bleeding and AI Research at DDW 2026
-
May 14, 2026, 11:57Luke Runion: Closing a Chapter with HFA While Continuing the Mission

