
Sadia Rao: Mechanism of Clopidogrel in Platelet Aggregation Inhibition
Sadia Rao, Pharmacologist, Founder and Lead Content Creator at PharmCept, shared a post on LinkedIn:
“Clopidogrel is an antiplatelet drug used in various cardiovascular conditions. To understand how clopidogrel works, it’s important first to understand the role of platelets in forming a hemostatic plug.
The Role of Endothelial Cells in Preventing Platelet Aggregation
- Endothelial cells line the interior of blood vessels, forming the vascular endothelium.
- Healthy endothelial cells produce chemical mediators like prostacyclin (PGI2) which act as inhibitors of platelet aggregation.
Prostacyclin binds to platelet membrane receptors that increases cAMP, an intracellular messenger. Increased cAMP levels reduce intracellular calcium, preventing platelet activation and the release of platelet aggregation agents.
Role of Thromboxane and Thrombin:
When the endothelium is intact:
- Circulating levels of thromboxane and thrombin are low. (Thromboxane is produced by activated platelets and thrombin is generated by coagulation cascade after vascular injury).
- Subendothelial collagen remains covered.
- Platelet membrane receptors for thromboxane, thrombin, and collagen remain unoccupied.
As a result, platelet aggregation is not initiated under normal conditions.
What Happens When the Endothelium Is Damaged
Endothelial injury triggers platelet aggregation through multiple mechanisms:
- Reduced Prostacyclin Production: Less prostacyclin means reduced stimulation of platelet receptors, lower cAMP levels, and increased platelet activation.
- Platelet Adhesion and Activation: Platelets adhere to exposed collagen in the subendothelium. This activates intracellular signaling, increasing calcium levels. Activated platelets release granules containing ADP, platelet-activation factors, and serotonin and simultaneously synthesize thromboxane A₂ (txa₂). These mediators bind to and activate nearby platelets, promoting aggregation.
- Activation of GP IIb/IIIa Receptors: Resting platelets have inactive GP IIb/IIIa receptors. ADP released from platelet granules binds P2Y12 receptors on platelets, which activates GP IIb/IIIa receptors. These GP IIb/IIIa receptors bind fibrinogen, enabling platelet-to-platelet interaction and thrombus formation.
Fibrinogen: A soluble plasma glycoprotein, binds GP IIb/IIIa receptors on two platelets, cross-linking them and promoting aggregation.
Thrombin: It is formed by local stimulation of coagulation, catalyzes the conversion of fibrinogen to fibrin. Cross-linked fibrin stabilizes the clot, forming a primary platelet-fibrin plug at the injury site.
After looking at the mechanism of platelet plug formation lets now see where does clopidogrel target…
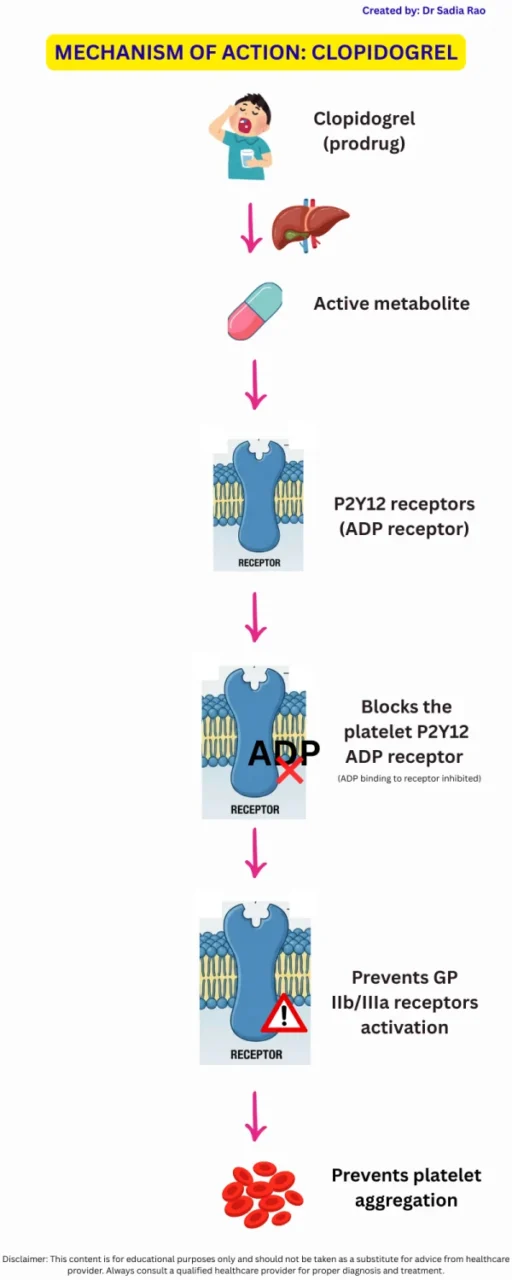
Clopidogrel binds irreversibly to P2Y12 receptors on platelets and inhibits the binding of ADP to these platelet receptors, which prevents activation of GP IIb/IIIa receptors. This inhibition blocks platelet binding to fibrinogen and other platelets, ultimately preventing platelet aggregation.
Bonus information: Clopidogrel is a prodrug and requires activation in the liver.
Active metabolite then targets platelet P2Y12 ADP receptor.
Disclaimer: This newsletter content is for educational purposes only and should not be taken as a substitute for advice from healthcare provider.
Always consult a qualified healthcare provider for proper diagnosis and treatment.”
Stay updated with Hemostasis Today.
-
Mar 21, 2026, 15:40Adeniji Mustapha: Breaking Down the Myths of High Blood Pressure
-
Mar 21, 2026, 15:36Akinchan Bhardwaj: The Real Silent Shift in the 2026 ACC/AHA Dyslipidemia Guideline
-
Mar 21, 2026, 15:32Marwa Mostafa: Iron Metabolism in the Differential Diagnosis of Anemia
-
Mar 21, 2026, 15:30Moustafa Abdou: The Value of Peripheral Blood Smear Examination in Hematology
-
Mar 21, 2026, 15:29Integrated Imaging in the Diagnosis of Prosthetic Valve Thrombosis and Coronary Embolism – ASE
-
Mar 21, 2026, 13:51Aroosa Zafar: DOACs in Atrial Fibrillation After Intracranial Hemorrhage
-
Mar 21, 2026, 13:47Kanishk Kumar: Evolving Therapeutic Landscape in Post-Polycythemia Vera Myelofibrosis
-
Mar 21, 2026, 13:32Jean-Baptiste Thibert: Protecting Fundamental Human Rights to Improve Patient Access and Donor Health
-
Mar 21, 2026, 12:47Georgiana Toma: From Cytoreduction to Vascular Protection in Essential Thrombocythemia

