
ASH25: Wolfgang Miesbach on Why No Single Haemophilia Therapy Is the “Winner”
Wolfgang Miesbach, Professor of Medicine at Frankfurt University Hospital, shared on LinkedIn:
The “Paradox of Choice” is very real in Haemophilia right now.
I just caught Dr. Mark Reding’s insightful presentation at ASH25, and it really highlighted that having more options doesn’t actually make the decision easier. In fact, it makes it much harder.
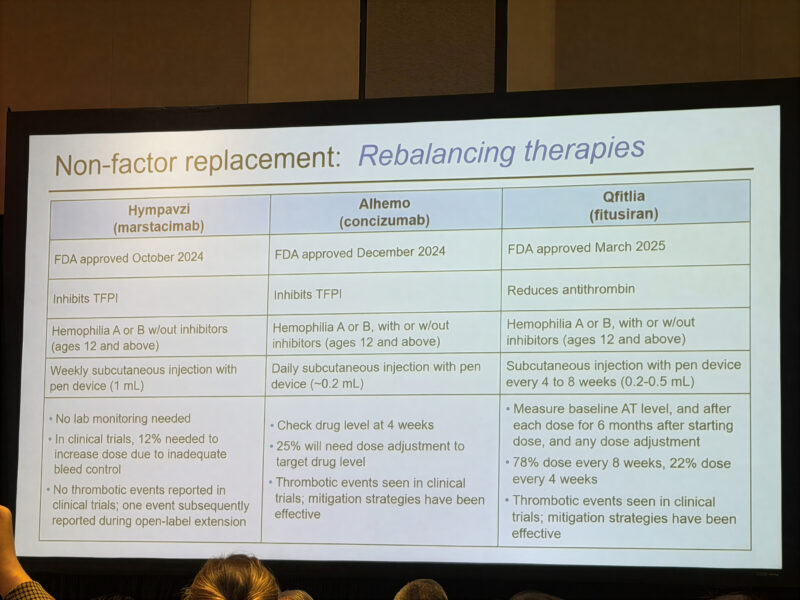
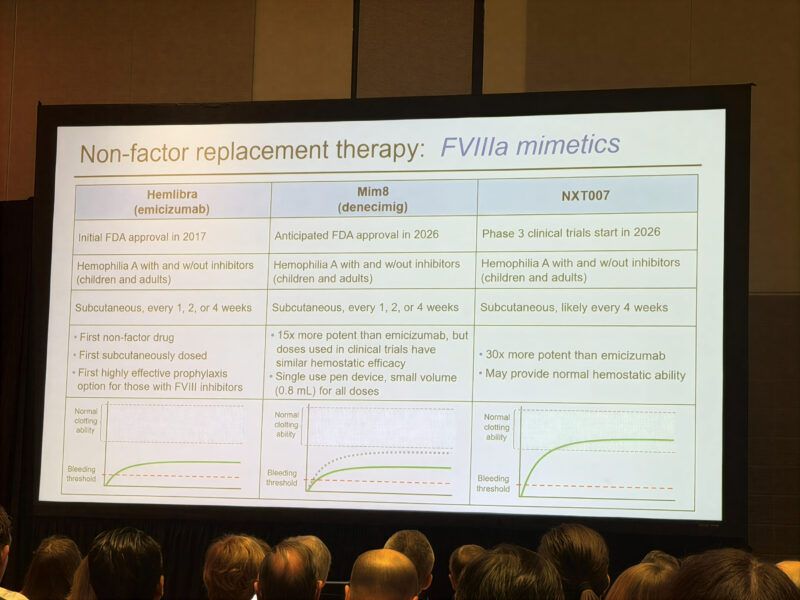
We’re looking at a massive toolkit now—extending half-life, bypassing (like the upcoming Mim8 or NXT007), rebalancing (Hympavzi, Alhemo, Qfitlia), or gene therapy (Roctavian, Hemgenix).
But Dr. Reding made a crucial point: the ‘menu’ isn’t actually open to everyone. You can’t just pick the one with the best marketing. The choice is heavily gated by biology (Type A vs B), age (Rebalancers ≥12y, gene Tx ≥18y), inhibitor Status, distribution and reimbursement issues.
But once you get past those gates, how do you actually choose? Dr. Reding laid out specific factors to break the tie:
– Venous Access is the First Filter: Before debating mechanism, look at the veins. For infants or adults with joint damage, a SubQ option isn’t just a preference – it’s a necessity.
– Risk Aversion is Personal: Some patients want the newest ‘zero bleed’ potency; others prioritize 20 years of safety data. As Dr. Reding noted, both are valid perspectives.
– Activity Level: Bleed risk isn’t static. A high-impact athlete needs a completely different protection profile than someone with a sedentary job.
The tricky part? There is no ‘winner.’
Because we have zero head-to-head data, we can’t say one is medically better than the other. We’re just trading attributes.
The solution? Realizing that the ‘best’ choice isn’t permanent.
What works for young children likely won’t be the right fit for an active adult. The goal isn’t to find the perfect drug for life, but the right fit for right now.
Shared decision-making has never been more important – because we aren’t just prescribing a drug anymore, we’re matching a mechanism to a lifestyle.
Stay updated with Hemostasis Today.
-
May 5, 2026, 16:28Nikolay Novitski: A New Era in Cardiovascular Prevention
-
May 5, 2026, 16:23Satyam Arora: Best Abstract Award in Pediatric Apheresis at ASFA 2026 Congress
-
May 5, 2026, 16:17Hannah Omunakwe: Your Sick Child Has a Clot. Did You See That Coming?
-
May 5, 2026, 15:57Venous Thromboembolism Risk in Pregnancy and the Postpartum Period – NBCA
-
May 5, 2026, 15:28Soumen Bhattacharyya: Hyperhomocysteinemia and Thrombosis – What Clinicians Should Know
-
May 5, 2026, 15:06Wolfgang Miesbach: How Should We Approach GI Angiodysplasia in VWD?
-
May 5, 2026, 14:48What Constitutes High Risk for Venous Thromboembolism? – JTH
-
May 5, 2026, 14:41How Real-Time Data, Rehabilitation Registries, and Patient-Reported Outcomes Can Transform Practice – European Stroke Organisation
-
May 5, 2026, 14:41Driving National Change for Bleeding Disorders – WFH

