
Dr Abdul Mannan: What’s Your Approach to Diagnosing Iron Deficiency in Tricky Cases?
Dr Abdul Mannan, Consultant Haematologist at Betsi Cadwaladr University Health Board, posted on LinkedIn:
“After years of managing anaemia across different patient populations, I’ve learned one thing: that single ferritin number on your screen? It’s not telling you the whole truth.
Let me explain with three patients I see regularly.
Patient 1: The “Normal” Pregnant WomanHer ferritin comes back at 20 µg/L.
“Normal range,” says the lab slip.
But here’s what the lab doesn’t know: she’s growing a human being. That baby needs iron. Her expanding blood volume needs iron. We’re talking about 1 gram of additional iron over 9 months.
A ferritin of 20 in pregnancy? That’s not normal. That’s a deficiency waiting to cause problems.
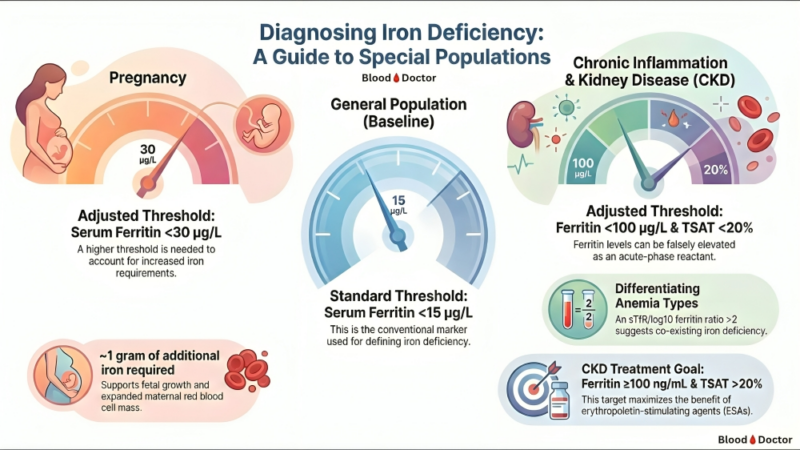
The fix: In pregnancy, think <30 µg/L as your red flag.
Patient 2: The CKD Patient with “Adequate” Iron
Ferritin: 85 µg/L.
Looks fine, right?
Wrong.
This patient has chronic kidney disease. Inflammation. Ferritin is an acute phase reactant — it rises when the body is inflamed, regardless of actual iron stores.
I’ve seen CKD patients with ferritin of 200 who were profoundly iron deficient.
The fix: In CKD and inflammation, you need TWO numbers: → Ferritin <100 µg/L AND → Transferrin saturation <20%
Both. Not one. Both.
And when you’re really stuck? The sTfR/log10 ferritin ratio >2 points toward true iron deficiency hiding behind inflammation.
Patient 3: The Textbook Case
Healthy adult. No inflammation. No pregnancy.
Ferritin <15 µg/L = iron deficiency.
Simple. Clean. The one time ferritin actually behaves.
The Bottom Line:
One number. Three completely different interpretations depending on who’s sitting in front of you.
Medicine isn’t about memorizing reference ranges. It’s about knowing when those ranges don’t apply.
The best doctors I know don’t just read results. They read context.
Quick Reference:
General population: Ferritin <15 µg/L
Pregnancy: Ferritin <30 µg/L
CKD/Inflammation: Ferritin <100 µg/L + TSAT <20%
Save this. Share it. Your patients will thank you.
What’s your approach to diagnosing iron deficiency in tricky cases?”
Follow the latest with Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

