Yves Bikorimana: Causes, Diagnosis, and Management of Neonatal Alloimmune Thrombocytopenia
Yves Bikorimana, CEO at MedData-Rwanda and Lab Scientist at The University Teaching Hospital of Kigali-Chuk, shared a post on LinkedIn:
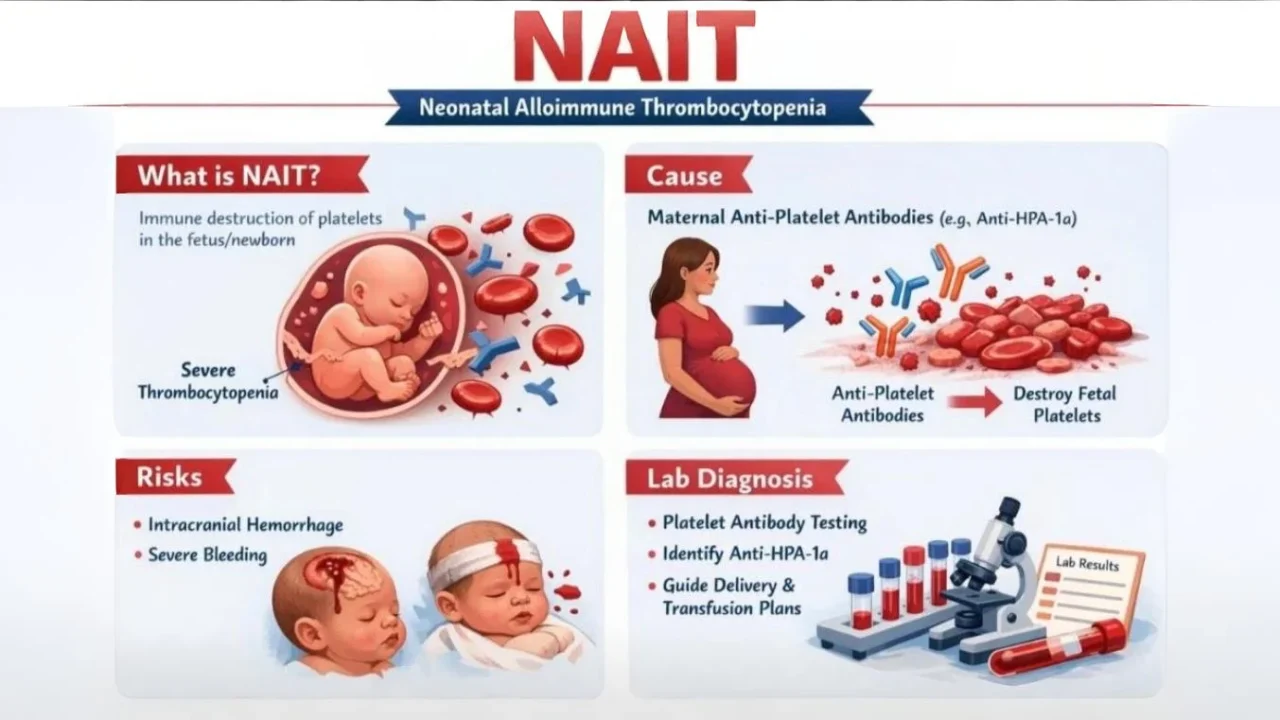
“Neonatal Alloimmune Thrombocytopenia (NAIT)
Neonatal Alloimmune Thrombocytopenia (NAIT) is a condition in which a newborn develops severe thrombocytopenia (low platelet count) due to the destruction of fetal platelets by maternal antibodies.
1. Definition
NAIT is an immune-mediated disorder where the mother’s immune system produces antibodies against fetal platelet antigens inherited from the father. These antibodies cross the placenta and destroy the baby’s platelets.
- Leads to low platelet count in the fetus or newborn
- Similar mechanism to hemolytic disease of the newborn, but it affects platelets instead of red blood cells
2. Cause / Pathophysiology
The main cause is maternal anti-platelet antibodies.
Process:
- The fetus inherits a platelet antigen from the father that the mother does not have.
- The mother’s immune system recognizes it as foreign.
- The mother produces IgG antibodies against this antigen.
- These antibodies cross the placenta.
- They bind to fetal platelets and cause their destruction.
Common antigen involved
Human Platelet Antigen‑1a (HPA‑1a)
3. Clinical Features
Newborns may show signs of severe thrombocytopenia, such as:
- Petechiae (small red spots on skin)
- Purpura
- Bruising
- Bleeding after birth
- Intracranial hemorrhage in severe cases
Sometimes the baby may appear normal at birth but develop bleeding symptoms later.
4. Major Risks / Complications
Severe platelet destruction can lead to:
- Intracranial hemorrhage (brain bleeding)
- Severe internal bleeding
- Neurological damage
- Death in severe untreated cases
Intracranial hemorrhage may occur before or shortly after birth.
5. Laboratory Diagnosis
Diagnosis is mainly done through immunological and platelet tests.
Tests include:
- Platelet count in the newborn (very low)
- Platelet antibody testing
- Identification of anti-HPA-1a antibodies
- Maternal and paternal platelet antigen typing
These tests help confirm the immune incompatibility between mother and fetus.
6. Management
Treatment aims to increase platelet count and prevent bleeding.
During pregnancy
- Maternal intravenous immunoglobulin (IVIG)
- Sometimes corticosteroids
- Careful fetal monitoring
After birth
- Platelet transfusion (preferably antigen-compatible)
- IVIG therapy
- Monitoring for intracranial hemorrhage
7. Key Points
- NAIT is the most common cause of severe thrombocytopenia in otherwise healthy newborns.
- Caused by maternal antibodies against fetal platelet antigens.
- HPA-1a incompatibility is the most common cause.
- Early diagnosis and treatment prevent life-threatening bleeding.”
Stay updated with Hemostasis Today.
-
Apr 30, 2026, 18:19Deva Nanda TK: A Practical Overview of Dural Sinuses and The Venous Drainage of the Brain
-
Apr 30, 2026, 18:08Amrit Kaur Kaler: The Hidden Genetic Drivers of Thrombosis
-
Apr 30, 2026, 18:06Alejandro González Veliz: The Most Dangerous Mistake After Getting a Stent
-
Apr 30, 2026, 18:03Carmen Ruiz: First Arterial Mechanical Thrombectomy in New Zealand Using the ARTIX System
-
Apr 30, 2026, 17:52Simon Senanu: von Willebrand Disease May Be Missed Despite Normal Tests
-
Apr 30, 2026, 17:20José Antonio García Erce: Why Healthy Older Adults Should Keep Donating Blood?
-
Apr 30, 2026, 17:13Paul Logan: Decoding the Words ‘He’s on blood thinners’
-
Apr 30, 2026, 17:01Jason Andrade: A Decade-Long Quest Proves Early Ablation Halves Persistent AF Burden
-
Apr 30, 2026, 16:56Oliver Maracic: Could Co-Targeting ALK with FAK/PYK2 Help Mitigate the High VTE Burden Seen in ALK with NSCLC

