
Soroush Sohrabi: Foam or Liquid for Spider Veins?
Soroush Sohrabi, Consultant Vascular and Endovascular Surgeon in Dubai, shared a post on LinkedIn:
“Foam or Liquid for Spider Veins? The Evidence Might Surprise You.
We treat telangiectasias every day. We choose between foam and liquid almost instinctively. But when you actually look at the evidence — it’s thinner than you think.
I reviewed approximately 15 publications spanning 1987 to 2024 comparing foam and liquid sclerotherapy for telangiectasias, including the Cochrane systematic review of 10 RCTs involving 484 patients.
Here’s what stands out:
- Only one study within the Cochrane review directly compared foam to liquid for telangiectasias. It had 20 patients. No statistics were performed. It was unblinded.
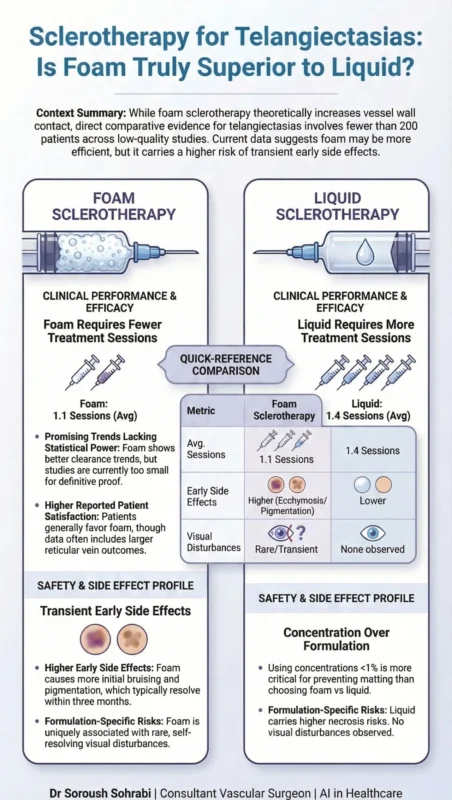
- Foam trends toward better efficacy and fewer sessions — but this has never been confirmed by a well-powered, blinded trial for spider veins specifically.
- Foam causes more early side effects – more pain in the first hours, more ecchymosis, more hyperpigmentation at one week. All resolve by three months.
- Concentration matters more than formulation. Using polidocanol or STS above one percent for veins under 1 mm drives most of the reported complications.
- Polidocanol is consistently less painful than STS regardless of whether you use foam or liquid. POL causes no more pain than placebo injection.
- Transient visual disturbances have been reported exclusively with foam — rare but worth discussing during consent.
- No formal clinical practice guideline makes a direct evidence-graded recommendation comparing foam to liquid for telangiectasias. Existing consensus documents suggest liquid is the preferred approach for C1 disease, with foam acceptable at lower concentrations — but this reflects expert opinion, not high-quality comparative evidence.
The bottom line: we don’t have a definitive answer. The field has invested heavily in comparing foam vs. liquid for truncal veins, but for the most common indication in cosmetic phlebology — spider veins — the comparative evidence is remarkably weak.
I created a poster summarising these findings. Swipe to see the full breakdown.
What’s your preference in practice — foam or liquid for telangiectasias? And why?”
Stay updated with Hemostasis Today.
-
Apr 30, 2026, 18:19Deva Nanda TK: A Practical Overview of Dural Sinuses and The Venous Drainage of the Brain
-
Apr 30, 2026, 18:08Amrit Kaur Kaler: The Hidden Genetic Drivers of Thrombosis
-
Apr 30, 2026, 18:06Alejandro González Veliz: The Most Dangerous Mistake After Getting a Stent
-
Apr 30, 2026, 18:03Carmen Ruiz: First Arterial Mechanical Thrombectomy in New Zealand Using the ARTIX System
-
Apr 30, 2026, 17:52Simon Senanu: von Willebrand Disease May Be Missed Despite Normal Tests
-
Apr 30, 2026, 17:20José Antonio García Erce: Why Healthy Older Adults Should Keep Donating Blood?
-
Apr 30, 2026, 17:13Paul Logan: Decoding the Words ‘He’s on blood thinners’
-
Apr 30, 2026, 17:01Jason Andrade: A Decade-Long Quest Proves Early Ablation Halves Persistent AF Burden
-
Apr 30, 2026, 16:56Oliver Maracic: Could Co-Targeting ALK with FAK/PYK2 Help Mitigate the High VTE Burden Seen in ALK with NSCLC

