Yves Bikorimana: Hemolysis – Why It Ruins Laboratory Results
Yves Bikorimana, CEO at MedData – Rwanda and Lab Scientist at The University Teaching Hospital of Kigali – Chuk, shared a post on LinkedIn:
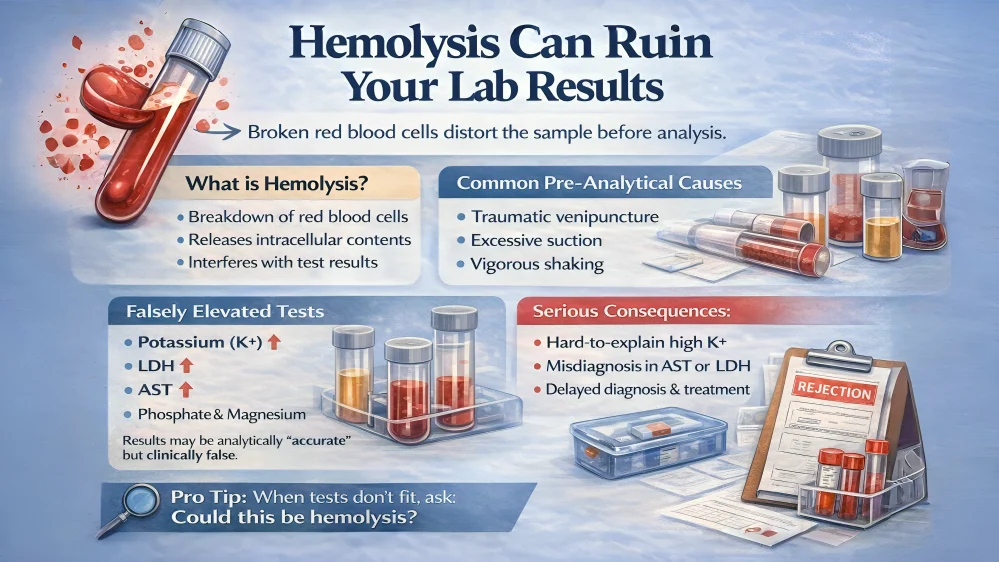
”Hemolysis—Why It Ruins Laboratory Results
Hemolysis happens when red blood cells break open before a blood sample is properly analyzed in the laboratory. When these cells rupture, they release their internal contents, such as potassium, LDH, AST, and other substances into the serum or plasma. Laboratory analyzers are designed to test blood assuming the cells are intact. So even if the machine works perfectly and prints a result, the biology of the sample has already been altered. This means the result may look accurate on paper but does not truly reflect what is happening inside the patient’s body.
Importantly, hemolysis usually does not occur inside the analyzer. It happens before the testing process even begins, during what we call the pre-analytical phase. This includes the time of blood collection, handling, and transport. Common causes include traumatic venipuncture, using a needle that is too small, pulling the syringe too forcefully, shaking the tube vigorously instead of gently inverting it, delaying centrifugation, or transporting the sample roughly. In simple terms, hemolysis is most often a collection or handling error, not a machine error.
Hemolysis can significantly affect laboratory results. For example, potassium levels may appear falsely elevated (a condition called pseudo-hyperkalemia). LDH and AST levels may also increase, which can falsely suggest tissue damage, liver disease, or muscle injury. Phosphate and magnesium may rise, and total protein values may be altered. The analyzer may measure these substances correctly, but because they leaked out of broken cells, the result becomes clinically misleading.
The clinical consequences of hemolysis can be serious. A patient might receive unnecessary treatments, such as calcium, insulin, or even dialysis, due to falsely high potassium levels. A doctor might suspect liver or muscle injury when none exists. This can delay the correct diagnosis, increase patient anxiety, and sometimes prolong hospital stays.
This is why laboratories sometimes reject hemolyzed samples. Sample rejection is not bureaucracy, it is patient safety. Reporting a known false result can lead to inappropriate treatment. Recollecting a new sample may take more time, but it is far safer than acting on incorrect information. One redraw is always better than one wrong treatment.
As a healthcare professional or laboratory student, it is important to think critically. If you see unexpected hyperkalemia, elevated AST without ALT changes, or high LDH without clinical symptoms, always ask yourself: Could this be hemolysis? Recognizing this possibility can prevent misdiagnosis and protect patients.
In summary, hemolysis is a preventable pre-analytical error that distorts laboratory results. Proper blood collection, gentle handling, and timely processing are essential to ensure accurate and clinically meaningful results.”

Stay updated with Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

