
Ifeanyichukwu Ifechidere: Understanding the Sensitivity and Specificity of D-Dimer
Ifeanyichukwu Ifechidere, Specialist Biomedical Scientist at Sheffield Teaching Hospitals NHS Foundation Trust, shared a post on LinkedIn:
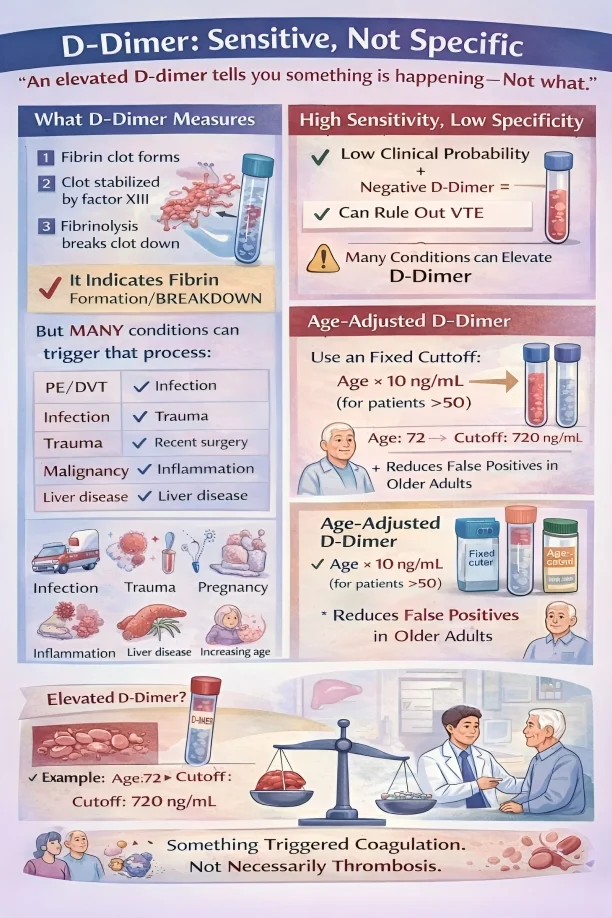
”D-Dimer: Sensitive, Not Specific
‘An elevated D-dimer tells you something is happening — not what.’
In laboratory medicine, few tests are misunderstood as often as D-dimer.
Many clinicians see a raised result and immediately think:
- Pulmonary embolism
- Deep vein thrombosis
But the truth is more nuanced.
D-dimer is a rule-out test — not a rule-in test.
Understanding its sensitivity and specificity is critical for interpreting it correctly.
What D-Dimer Actually Measures
D-dimer is a fibrin degradation product.
It forms when:
- Fibrin clot forms
- The clot is stabilized by factor XIII
- The fibrinolytic system breaks it down
So an elevated D-dimer tells us fibrin formation and breakdown have occurred.
But that process happens in many physiological and pathological states.
High Sensitivity: Why D-Dimer Is Useful
D-dimer tests are designed to be highly sensitive.
That means:
- Most patients with venous thromboembolism (VTE) will have an elevated result.
So if a patient has:
- Low clinical probability
- Negative D-dimer
- VTE can usually be safely excluded.
- This is where D-dimer shines.
Low Specificity: Why It’s Often Misinterpreted
The challenge is specificity.
Many conditions elevate D-dimer, including:
- Infection
- Inflammation
- Trauma
- Recent surgery
- Pregnancy
- Malignancy
- Liver disease
- Increasing age
So a high result simply means:
- ‘Something triggered coagulation and fibrinolysis.’
- Not necessarily thrombosis.
- This is why ordering D-dimer without clinical pre-test probability often leads to unnecessary imaging.
The Importance of Age-Adjusted D-Dimer
- One of the biggest improvements in recent years has been the use of age-adjusted thresholds.
- D-dimer levels naturally increase with age.
- Using a fixed cutoff (often 500 ng/mL) in older adults can lead to large numbers of false positives.
The commonly used adjustment:
Age × 10 ng/mL (for patients over 50)
Example:
Age 70 to cutoff 700 ng/mL
This approach significantly reduces unnecessary CT scans while maintaining safety.
The Real Takeaway
- D-dimer isn’t a diagnosis.
- It’s a signal.
- A normal D-dimer can help exclude thrombosis in the right clinical context.
An elevated D-dimer simply tells us:
The coagulation and fibrinolytic systems have been activated.
And that could be for many reasons.
As biomedical scientists, our role is not just to report the number — but to ensure the limitations and context of the test are understood.
Because in laboratory medicine:
A sensitive test can be powerful.
A misunderstood test can be dangerous.
What’s the biggest D-dimer misconception you’ve seen in practice?
Is it being used as a standalone diagnostic test, or something else entirely?”
Stay updated with Hemostasis Today.
-
May 12, 2026, 16:46Tagreed Alkaltham: Why Apheresis Matters in Modern Transfusion Medicine
-
May 12, 2026, 16:37Reinhold Kreutz: Cardiovascular Burden in Acute Intermittent Porphyria Needs Greater Awareness
-
May 12, 2026, 16:33Pablo Corral: The Truth About Very Low LDL-Cholesterol
-
May 12, 2026, 16:24Mildred Lundgren: We Must Talk About the Invisible Causes of Stroke
-
May 12, 2026, 16:17Irene Scala: The Sex Disparities In Access to Acute Stroke Treatments In Italy
-
May 12, 2026, 16:04May Nour: UCLA Health Mobile Stroke Unit Becomes The 1st In The World to Perform mCTA In the Field
-
May 12, 2026, 15:57Leonardo Roever: Prognostic Impact of Lipoprotein(a) and CAR in Elderly Acute Ischemic Stroke Patients
-
May 12, 2026, 15:54Bruno Pougault: Prioritizing Laboratory Tests in Resource-Limited Emergency Care
-
May 12, 2026, 15:37Jennifer Holter Chakrabarty: Supporting the Next Generation of Hematology Researchers

