Tagreed Alkaltham: WB Donation vs Apheresis Donation – Understanding Donor Reactions and Why They Differ
Tagreed Alkaltham, Transfusion Medicine Lab Supervisor at KSMC, shared a post on LinkedIn:
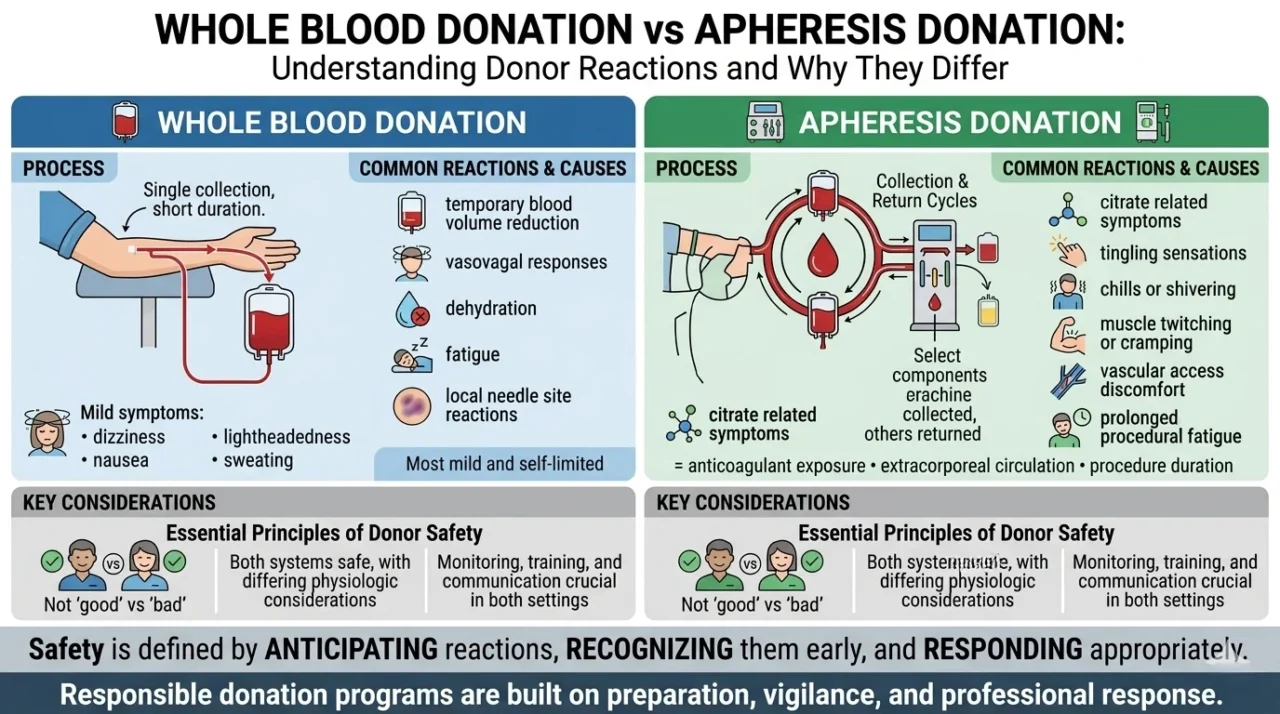
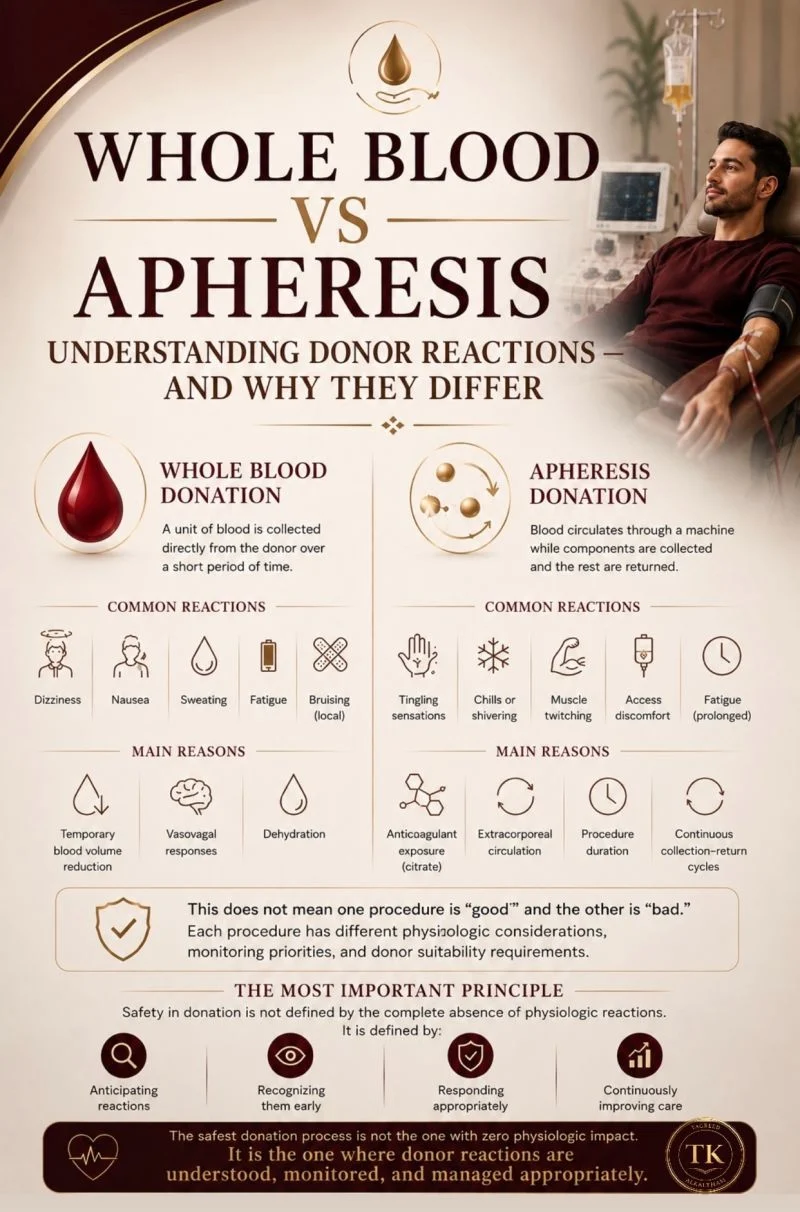
“Whole Blood Donation vs Apheresis Donation
Understanding Donor Reactions and Why They Differ
Not all donation reactions happen for the same reason. And not all donation procedures affect the body in the same way. That distinction matters.
Because whole blood donation and apheresis donation are fundamentally different processes physiologically, even though both are performed within structured donor safety systems.
In whole blood donation:
A unit of blood is collected directly from the donor over a relatively short period of time.
The most common donor reactions are often related to:
- temporary blood volume reduction
- vasovagal responses
- dehydration
- fatigue
- or local needle site reactions such as bruising
Some donors may experience:
- dizziness
- lightheadedness
- nausea
- sweating
- temporary weakness
Most reactions are mild and self limited.
In apheresis donation:
Blood continuously circulates through an extracorporeal circuit while selected components are collected and the remaining components are returned to the donor.
Because the procedure is different, the physiologic considerations are also different.
Apheresis reactions may involve:
- citrate related symptoms
- tingling sensations
- chills or shivering
- muscle twitching or cramping
- vascular access discomfort
- or prolonged procedural fatigue in some donors
These reactions are often associated with:
- anticoagulant exposure
- extracorporeal circulation
- procedure duration
- and continuous collection return cycles.
This does not mean one procedure is ‘good’ and the other is ‘bad.’
And it does not mean one donor reaction profile automatically makes one approach universally safer than the other. Each procedure has different physiologic considerations, monitoring priorities, and donor suitability requirements.
That is why donor selection, procedural monitoring, staff training, and communication remain essential in both settings.
The most important principle is this:
Safety in donation is not defined by the complete absence of physiologic reactions.
It is defined by:
- anticipating reactions
- recognizing them early
- responding appropriately
- and continuously improving donor care systems.
Because responsible donation programs are not built on perfect physiology. They are built on preparation, vigilance, and professional response.
The safest donation process is not the one with zero physiologic impact. It is the one where donor reactions are understood, monitored, and managed appropriately.”
Other posts featuring Tagreed Alkaltham on Hemostasis Today.
-
May 10, 2026, 15:14Could You Recognize Thrombotic Thrombocytopenic Purpura (TTP) in Time? – ASH
-
May 10, 2026, 15:13Deepak Lodha: PT and aPTT Mixing Study is a Key Tool in Coagulation Diagnosis
-
May 10, 2026, 15:12Marc Wittwer: Excellent Days at the 7th Coagulation Days in Zagreb
-
May 10, 2026, 15:11Divyaswathi Citla Sridhar and Leonard Valentino Congratulate Roshni Kulkarni on Her Recognition as Advocate for Women and Girls with Bleeding Disorders
-
May 10, 2026, 15:09Haroun Gajraj: How Much of a Problem are Brown Marks after Sclerotherapy, Really?
-
May 10, 2026, 15:05Arun Chandran Nhattuvalappil: Simplifying Anticoagulation Decisions for Regional Anaesthesia with ASRA 2025 Guideline
-
May 10, 2026, 15:02Jean-Jacques Kiladjian: Inserm Grand Est Meeting on Clinical Research at CIC Strasbourg
-
May 10, 2026, 14:31Thomas Rocco: Humanity in the Age of AI
-
May 10, 2026, 14:03Educational Grant Opportunities for Post–Secondary Students with Inherited Bleeding Disorders – Irish Haemophilia Society

