
Augustina Isioma Ikusemoro: Kell vs RhD Sensitization – The Difference in RBC Destruction
Augustina Isioma Ikusemoro, Hematology and Transfusion Medicine Specialist at Sharjah Blood Transfusion and Research Center, shared a post on LinkedIn:
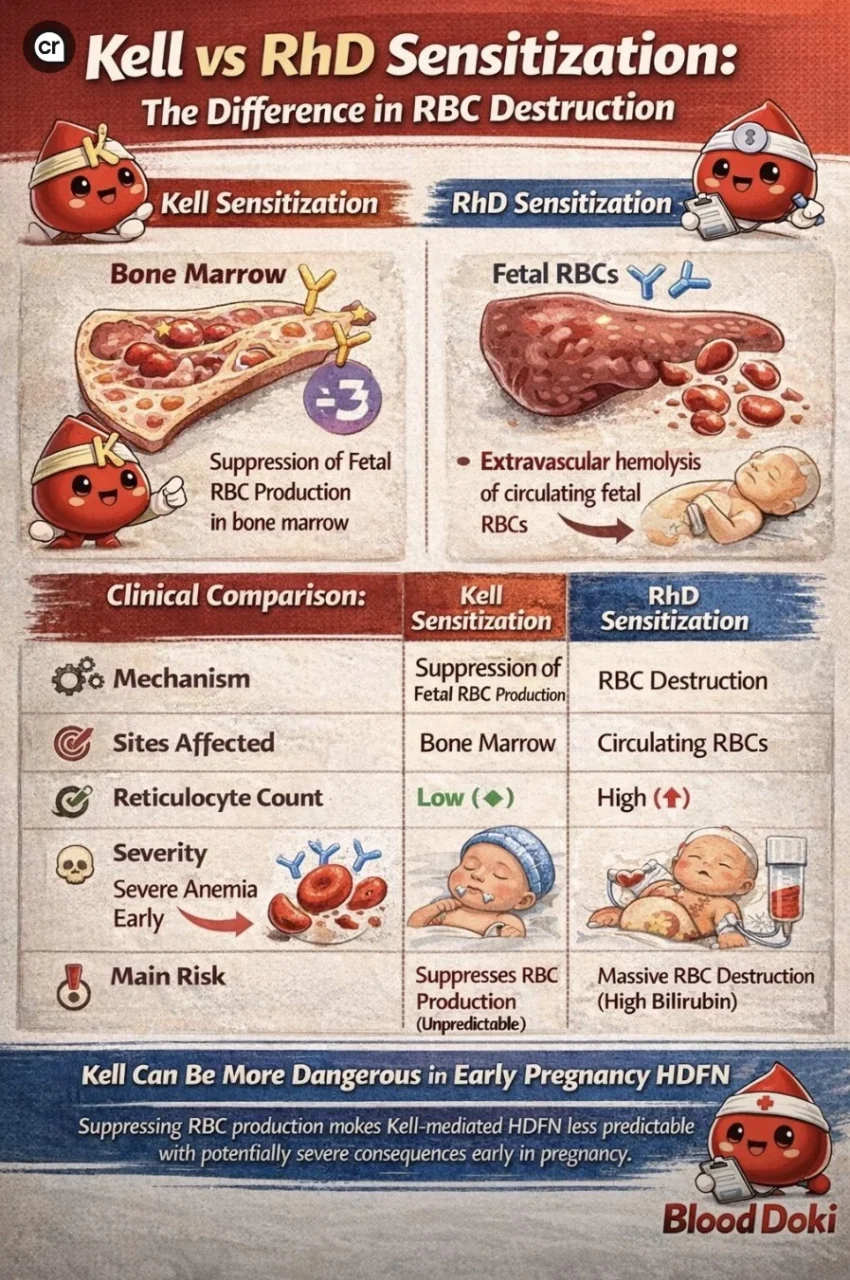
“Anti-D destroys red cells.
Anti-K stops them from being made.
That difference can change everything in fetal survival.
Most clinicians are trained to recognize RhD sensitization as a major cause of Hemolytic Disease of the Fetus and Newborn (HDFN).
But fewer appreciate that Kell sensitization can be equally — and sometimes more — dangerous.
Here’s why this matters
While RhD antibodies destroy circulating fetal red blood cells, Anti-K antibodies suppress fetal red cell production at the bone marrow level.
This means:
- RhD sensitization leads to hemolysis
- Kell sensitization leads to erythropoiesis suppression
And clinically, that distinction is critical.
In RhD HDFN, anemia develops because red cells are destroyed in the fetal spleen.
In Kell-mediated HDFN, anemia develops because red cells are never produced in adequate numbers in the first place.
The result?
- Earlier onset anemia
- Lower reticulocyte counts
- Less predictable disease progression
- Severe fetal compromise even with low antibody titers
Unlike RhD disease — where bilirubin levels often reflect severity — Kell disease can progress silently until fetal anemia becomes critical.
This is why Anti-K detection during pregnancy must always trigger enhanced fetal surveillance.
And why transfusion services must prioritize:
- K- antigen matching for sensitized patients
- Prevention of alloimmunization in women of child-bearing age
- Extended phenotype awareness beyond ABO and RhD
Because transfusion safety doesn’t stop at compatibility.
It continues with anticipation.
Blood Doki
Advancing transfusion safety through education, systems awareness, and clinical insight.”
Stay updated with Hemostasis Today.
-
May 23, 2026, 05:38SIUH Advances Precision Stroke Care with Vena MicroAngioscope – Northwell Health
-
May 23, 2026, 05:31Kalyan Roy: Precision Blood Matching in Transfusion-Dependent Thalassaemia
-
May 23, 2026, 05:29Understanding Hepatitis A, B, and C During Hepatitis Awareness Month – UNC Health
-
May 23, 2026, 03:55WFH Initiative Brings Hope to the Hemophilia Community in India
-
May 23, 2026, 03:47Satyam Arora: Welcoming the New ISBT Board for the 2026 Term
-
May 23, 2026, 03:33Brig Tathagata Chatterjee: Connecting With World Leaders in Hematology at ISH Congress
-
May 23, 2026, 03:18Mathangi Kumar: Dental Management Strategies for Congenital Hemophilia
-
May 23, 2026, 03:02Maitri Vaishnav: Anatomical Variability and Surgical Relevance of Corona Mortis
-
May 23, 2026, 02:26Muhammad Hashim: When the Blood Smear Told a Different Story Behind a ‘Critical’ Platelet Count

