
Ney Carter Borges: Antithrombotic Therapy in 2025 – A Precision-Based Pharmacologic Update
Ney Carter Borges, Member Cardiologist of Global Physician Association at Cleveland Clinic Florida, shared a post on LinkedIn:
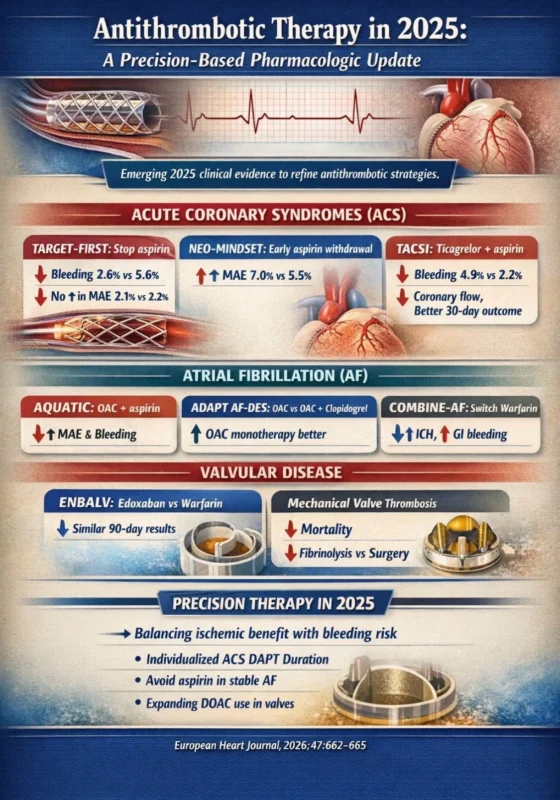
“Antithrombotic Therapy in 2025: A Precision-Based Pharmacologic Update
The 2025 cardiovascular literature substantially refined antithrombotic strategies across acute coronary syndromes (ACS), atrial fibrillation (AF), and prosthetic valve management, emphasizing individualized risk stratification and bleeding mitigation .
In ACS, the Target-first trial demonstrated that discontinuing aspirin after one month of dual antiplatelet therapy (DAPT) and continuing potent P2Y12 inhibitor monotherapy reduced actionable bleeding (2.6% vs 5.6%, P equals .002) without increasing major adverse events (2.1% vs 2.2%).
Conversely, Neo-mindset showed that very early aspirin withdrawal within 4 days post-PCI, although reducing bleeding (2.0% vs 4.9%), failed to maintain non-inferiority for ischemic protection (MAE 7.0% vs 5.5%). These findings confirm that at least one month of DAPT remains essential after ACS.
In post-CABG patients (TACSI), ticagrelor plus aspirin did not reduce ischemic events compared with aspirin alone but doubled major bleeding (4.9% vs 2.2%).
The Celebrate trial further supported early pharmacologic platelet inhibition: pre-hospital subcutaneous zalunfiban improved coronary flow (P equals .012) and 30-day hierarchical outcomes (P equals .028) with only mild-to-moderate bleeding excess.
In AF, the Aquatic trial demonstrated that adding aspirin to oral anticoagulation (OAC) in stable chronic coronary syndrome increased major adverse events (16.9% vs 12.1%), major bleeding (10.2% vs 3.4%), and mortality.
Similarly, Adapt AF-DES confirmed the superiority of OAC monotherapy beyond 12 months after stenting.
In elderly frail patients, Combine-AF showed that switching from warfarin to a direct oral anticoagulant (DOAC) reduced intracranial hemorrhage (0.38%/year vs 1.33%/year) and fatal bleeding, at the cost of increased gastrointestinal bleeding.
Prestige-AF highlighted the complexity of anticoagulation after intracerebral hemorrhage: DOAC therapy markedly reduced ischemic stroke (0.83%/year vs 8.60%/year) but increased recurrent ICH (5.0%/year vs 0.82%/year), underscoring the need for individualized decisions.
In valvular disease, ENBALV demonstrated comparable short-term outcomes between edoxaban and warfarin after bioprosthetic valve surgery, while a randomized pilot study in mechanical valve thrombosis showed lower in-hospital and 1-year mortality with prolonged low-dose fibrinolysis compared with urgent surgery.
Collectively, 2025 data reinforce precision antithrombotic therapy—balancing ischemic benefit against bleeding risk through patient-specific, context-driven pharmacologic selection.”
Stay updated with Hemostasis Today.
-
May 29, 2026, 04:37Josefin Ahnström: How Andexanet Alfa Impacts TFPIα Function
-
May 29, 2026, 03:19Building Safer Systems for Anticoagulation Management – ISTH
-
May 29, 2026, 03:07Early Diagnosis Can Change the Lives of Women With Haemophilia – EHC
-
May 29, 2026, 02:41Ifeanyichukwu Ifechidere: The Biggest DOAC Myth in Coagulation – ‘No Monitoring Required’
-
May 29, 2026, 02:35Mariam Swidan: Why Is LDH the ‘Tattletale’ of the Lab?
-
May 29, 2026, 02:20Yuntian Wang: Multi-View Learning for Predicting Avatrombopag Response in Pediatric Immune Thrombocytopenia
-
May 29, 2026, 01:57Giuseppina Caligiuri: Pathophysiological Challenges and Emerging Therapeutic Strategies in Acute Stroke
-
May 28, 2026, 23:47Hussnain Javaid: The Importance of Targeted Examination in Iron Deficiency Anaemia
-
May 28, 2026, 23:47ASH Heads to ASCO26 with Career Opportunities and Global Hematology Leadership

